Hussein Yassine is a physician and researcher who studies brain lipid utilization in the context of finding preventative measures for cognitive impairment, specifically Alzheimer’s disease (AD). In my conversation with Hussein, we begin with a fundamental coursework in brain biology—including its architecture and energy systems. We go on to discuss what these systems look like when something goes wrong and cognitive decline ensues. We talk about the evolutionary origins of the ApoE genotype, with specific attention to the ApoE4 allele and its association with AD. We spend time discussing ApoE4 implications for the brain’s fuel utilization, notably omega-3 fatty acids: EPA and DHA. We briefly pivot to the implications of recent omega-3 trials for cardiovascular disease and return to what we currently understand about EPA/DHA and brain health; we contemplate potential dietary interventions across the lifespan to preserve and prolong cognitive function.
Subscribe on: APPLE PODCASTS | RSS | GOOGLE | OVERCAST | STITCHER
We discuss:
- Hussein’s Background and introduction to brain composition (3:00);
- The blood-brain barrier and brain filtration (8:00);
- Lipids and brain function (13:00);
- How the brain utilizes energy (18:00);
- Apolipoprotein E (ApoE) structure and function in the periphery (27:30);
- ApoE function in the brain (38:15);
- Evolutionary origins of ApoE isoforms (43:45);
- ApoE4 variant and Alzheimer’s Disease (AD) risk (53:30);
- Dietary fuel preference with the ApoE4 allele (1:03:00);
- The role of omega-3 fatty acids in the brain (1:13:30);
- Comparing findings from the REDUCE-IT and STRENGTH trial (1:21:45)
- The relationship between dietary omega-3 intake and brain health (1:34:15);
- Preventing cognitive decline: A critical window for DHA in ApoE4 carriers? (1:42:30);
- Hussein’s ongoing research and recommendations for E4 carriers (1:54:00); and
- More.
Hussein’s Background and introduction to brain composition [3:00]
- Hussein grew up in Beirut, Lebanon and went to medical school there and moved to the U.S. to do residency training and his fellowship
- Did a fellowship in endocrinology
- Comes from a family with heart disease and diabetes so decided to subspecialize in lipid disorders
- He studied blood lipids for 2-3 before moving to brain lipids
The brain is composed of 3 main types of cells
- The brain is a unique compartment that is mostly lipid
- Contains a large amount of lipids—from sterols to different forms of fatty acids
- Neurons which are responsible for firing and forming synapses; the regulate how the brain functions
- Helper cells help neurons function in the brain
- glial cells are the immune cells responsible for clean up
- Microglial cells are cleanup specialists and have been linked to neurodegenerative diseases
- astrocytes repair and supply nutrients; regulate energy storage production
The blood-brain barrier and brain filtration [8:00]
The brain is surrounded by the blood-brain barrier
- separates the blood vessels and the blood inside the blood vessels from the brain
- designed to protect the brain and to maintain a stable environment
- composed of:
- endothelial cells called capillary cells that have a lining of tight junctions
- Pericytes surround those endothelial cells and support the maintenance of the barrier
- mural cells, or wall cells, make up the matrix surrounding pericytes and capillary cells
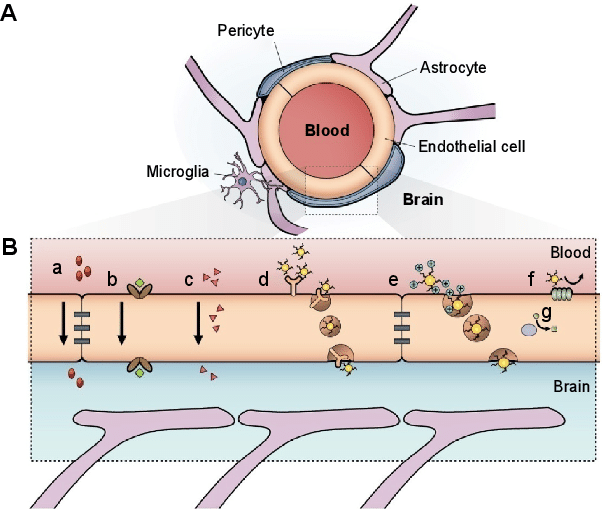
Figure 1. Schematic representation of the blood–brain barrier. (A) Scheme of the neurovascular unit that constitutes the BBB and (B) the main routes of the crossing of molecules to the CNS are represented [source]
Cerebral spinal fluid (CSF) os the “sewage system” of the brain
- Allows drainage from the brain cells, from the interstitial fluid
{end of show notes preview}

Hussein Yassine, M.D.
Hussein is a physician and researcher who is an Associate in the Department of Medicine, Keck School of Medicine of USC. His lab studies how changes in lipid metabolism and nutrition affect cognition and the risk of developing Alzheimer’s disease, paying specific attention to how the APOE4 allele affects lipid metabolism and response to diet. He directs the Roybal Alzheimer’s disease Research program focused on understanding how obesity, diabetes, and vascular risk factors in Los Angeles’s Latinx population affect cognition and Alzheimer’s disease risk. He also runs the Lipid Clinic at Roybal Healthcare Center in East LA, providing care for a large population of complex lipid and diabetes disorders that are referred from all LA county clinics.





Corrections: contrary to the author’s comments, the STRENGTH trial was NOT “an EPA trial”. “Epanova is a mixture of polyunsaturated free fatty acids, also referred to as carboxylic acids, the most abundant of which are EPA and DHA (0.550 g EPA and 0.200 g DHA in each 1-g capsule).” STRENGTH was yet another in an extensive list of the “graveyard of failed epa/dha trials” failing to show cvd event reduction, in STARK contrast to the two pure EPA trials (JELLIS and REDUCE-IT) which DID show highly clinically and statistically significant event reductions (IN REDUCE-IT even more cvd event reductions were seen in the USA ( very dysmetabolic) sub-population. Why does this seem to puzzle the author ? EPA has significantly different effects form DHA on inflammation, lipid movement/ accumulation in membranes, and many other properties. The significance of the mineral oil placebo’s effects has long since been dismissed as having a trivial effect, if any, on the cvd event reductions. “lack of a clear moa for cvd event reduction” worries the lecturer? I cannot explain how my plane (or my car ) gets me home, but it gets me there safely , and that’s all that matters ! Widesperead use of IPE ( EPA only Omega 3) is recommended by virtually ALL international CVD societies now (for appropriate patients based on REDUCE-IT) and would result in massive cvd event reductions if used properly. Time to move forward and reduce events in our patients, not hesitate whiles lives are lost and cvd morbidity mounts!
As I mentioned in a previous post, DHA also seems to be prone to raising apoB (and in studies where apoB is not measured, LDL-C), whereas most studies have not found this for EPA:
https://peterattiamd.com/tomdayspring6/comment-page-1/#comment-34949
Peter,
Thanks for this really informative podcast.
One topic you two walked up to but didn’t address is whether the blood brain barrier’s lost functionality – resulting in the slow “starvation” of the CNS – could be addressed via pharmaceuticals. What exactly happens to epithelial cells that compromises their “nutrient transporter” abilities?
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4292164/
“Nutrient transporters facilitate the movement of specific nutrients down their concentration gradient. CNS ECs express a wide variety of these transporters to deliver very specific nutrients across the physical barrier of the CNS ECs into the CNS parenchyma. Many of these belong to the solute carrier class of facilitated transporters, including slc2a1 (glucose), slc16a1 (lactate, pyruvate), slc7a1 (cationic amino acids), and slc7a5 (neutral amino acids, l-DOPA) (Zlokovic 2008; Daneman 2012). Slc2a1, also called glut1, has been largely studied for its role in providing the CNS with glucose. Expression of this transporter is highly enriched in CNS ECs compared with ECs in nonneural tissues, and it facilitates the transport of glucose down its concentration gradient from the blood into the brain (Cornford et al. 1994)”
Thank you. My mother died of Alzheimer’s at the age 67. She was diagnosed at age 60.
It looks as though my comments about cholesterol were not posted.
Again, if you are going to discuss lipids and the brain, I recommend looking at cholesterol trafficking in the brain. There are multiple studies showing a dysregulation pf cholesterol in several neurodegenerative disease. You need to explore the work of Dr Pikuleva on CYP46a1 at Case Western.
Cholesterol 24-Hydroxylation by CYP46A1: Benefits of Modulation for Brain Diseases
https://link.springer.com/article/10.1007/s13311-019-00731-6
Her efforts to repurpose low dose Efavirenz to activate CYP46a1.
https://link.springer.com/article/10.1007/s13311-019-00737-0
CYP46A1 gene therapy deciphers the role of brain cholesterol metabolism in Huntington’s disease
https://academic.oup.com/brain/article/142/8/2432/5529274
In Vitro Activation of Cytochrome P450 46A1 (CYP46A1) by Efavirenz-Related Compounds
https://pubs.acs.org/doi/10.1021/acs.jmedchem.9b01383
Efavirenz for Patients With Alzheimer’s Disease (EPAD)
https://www.clinicaltrials.gov/ct2/show/NCT03706885?term=cyp46a1&draw=2&rank=1
Interestingly, Pikuleva’s early work focused on Omega 3 as means to activated cyp46a1. However, it was unclear how much EPA/DHA was getting past the blood brain barrier.
Marked variability in hepatic expression of cytochromes CYP7A1 and CYP27A1 as compared to cerebral CYP46A1. Lessons from a dietary study with omega 3 fatty acids in hamsters
https://www.sciencedirect.com/science/article/abs/pii/S1388198110000612
Hi,
Great podcast, like always. I have a question about ketones body and E4 and disease – you put a link to DHA study, not to ketones body supplementation:
“Once E4 carriers have disease there is likely less benefit from ketone supplementation compared to non-carriers
The largest studies to date do not demonstrate beneficial response to supplementation once E4 carriers have disease”
Best,
Pawel
None of the studies on ketogenic diets or enhanced ketogenesis via enriched MCT oil in AD or even mild cognitive impairment (MCI, the prodrome) are convincing in any group. But Dr. Hussein is correct that APOEε4 carriers don’t even show the hints of possible efficacy seen in the subjects as a whole:
https://www.nutritionandmetabolism.com/content/6/1/31
https://www.biomedcentral.com/1471-2350/12/137
https://www.researchgate.net/publication/8582818_Effects_of_beta-hydroxybutyrate_on_cognition_in_memory-impaired_adults
This is supported by surrogate markers:
https://pubmed.ncbi.nlm.nih.gov/30006299/
https://bmcmedgenet.biomedcentral.com/articles/10.1186/1471-2350-12-137
Re: the dose and ratio of EPA:DHA in STRENGTH: they used 4 g/day of omega-3s from Epanova, which contains “50-60% eicosapentaenoic acid (EPA) and 15-25% docosahexaenoic acid (DHA).”
https://www.pbm.va.gov/PBM/clinicalguidance/drugmonographs/Omega_3_Carboxylic_Acids_EPANOVA_Drug_Monograph.pdf
So anywhere from 4:1 and 2:1. That seems reasonably consistent with the Vascepa hypothesis that DHA is somehow limiting or counteracting the beneficial effects of EPA, although there’s still that pesky mineral oil question. And of course, their effects on cognitive decline may be a different kettle of fish (pardon the pun) entirely: no one has yet shown a compelling result with any combination, although no one has tried an EPA-only formula as far as I know.
Re: the “(NIH) landmark studies in mouse model showed that pregnant mice deprived of DHA had offspring with neurons that did not make enough synapse”: as I had expected, the paper did not actually provide or withdraw DHA itself, but the precursor esssential fatty acid, alpha-linolenic acid. Of course, mice and many land-based mammals are vegetarian or nearly so, and could hardly be reliant on animal- (let alone marine-) derived preformed DHA. The mice, like cattle and many nonhuman primates, formed their brains using DHA derived from ALA conversion. It’s only when NO omega-3 source was provided that microcephaly ensued.
Similarly, there’s no evidence for cognitive deficits in children born of vegetarian or vegan mothers, and the most obvious problems they do show are related to other micronutrient deficiencies if the children themselves are put on such a diet.
I am late in listening to this podcast. I am wondering how one would go about getting genetically tested for the ApoE4 genetic variant aside from 23 and me? Thanks.