Want to catch up with other articles from this series?
- The straight dope on cholesterol – Part I
- The straight dope on cholesterol – Part II
- The straight dope on cholesterol – Part III
- The straight dope on cholesterol – Part IV
- The straight dope on cholesterol – Part V
- The straight dope on cholesterol – Part VI
- The straight dope on cholesterol – Part VII
- The straight dope on cholesterol – Part VIII
- The straight dope on cholesterol – Part IX
Previously, in Part I, Part II and Part III of this series, we addressed these 5 concepts:
#1 — What is cholesterol?
#2 — What is the relationship between the cholesterol we eat and the cholesterol in our body?
#3 — Is cholesterol bad?
#4 — How does cholesterol move around our body?
#5 –How do we measure cholesterol?
Quick refresher on take-away points from previous posts, should you need it:
- Cholesterol is “just” another fancy organic molecule in our body but with an interesting distinction: we eat it, we make it, we store it, and we excrete it – all in different amounts.
- The pool of cholesterol in our body is essential for life. No cholesterol = no life.
- Cholesterol exists in 2 forms – unesterified or “free” (UC) and esterified (CE) – and the form determines if we can absorb it or not, or store it or not (among other things).
- Much of the cholesterol we eat is in the form of CE. It is not absorbed and is excreted by our gut (i.e., leaves our body in stool). The reason this occurs is that CE not only has to be de-esterified, but it competes for absorption with the vastly larger amounts of UC supplied by the biliary route.
- Re-absorption of the cholesterol we synthesize in our body (i.e., endogenous produced cholesterol) is the dominant source of the cholesterol in our body. That is, most of the cholesterol in our body was made by our body.
- The process of regulating cholesterol is very complex and multifaceted with multiple layers of control. I’ve only touched on the absorption side, but the synthesis side is also complex and highly regulated. You will discover that synthesis and absorption are very interrelated.
- Eating cholesterol has very little impact on the cholesterol levels in your body. This is a fact, not my opinion. Anyone who tells you different is, at best, ignorant of this topic. At worst, they are a deliberate charlatan. Years ago the Canadian Guidelines removed the limitation of dietary cholesterol. The rest of the world, especially the United States, needs to catch up. To see an important reference on this topic, please look here.
- Cholesterol and triglycerides are not soluble in plasma (i.e., they can’t dissolve in water) and are therefore said to be hydrophobic.
- To be carried anywhere in our body, say from your liver to your coronary artery, they need to be carried by a special protein-wrapped transport vessel called a lipoprotein.
- As these “ships” called lipoproteins leave the liver they undergo a process of maturation where they shed much of their triglyceride “cargo” in the form of free fatty acid, and doing so makes them smaller and richer in cholesterol.
- Special proteins, apoproteins, play an important role in moving lipoproteins around the body and facilitating their interactions with other cells. The most important of these are the apoB class, residing on VLDL, IDL, and LDL particles, and the apoA-I class, residing for the most part on the HDL particles.
- Cholesterol transport in plasma occurs in both directions, from the liver and small intestine towards the periphery and back to the liver and small intestine (the “gut”).
- The major function of the apoB-containing particles is to traffic energy (triglycerides) to muscles and phospholipids to all cells. Their cholesterol is trafficked back to the liver. The apoA-I containing particles traffic cholesterol to steroidogenic tissues, adipocytes (a storage organ for cholesterol ester) and ultimately back to the liver, gut, or steroidogenic tissue.
- All lipoproteins are part of the human lipid transportation system and work harmoniously together to efficiently traffic lipids. As you are probably starting to appreciate, the trafficking pattern is highly complex and the lipoproteins constantly exchange their core and surface lipids.
- The measurement of cholesterol has undergone a dramatic evolution over the past 70 years with technology at the heart of the advance.
- Currently, most people in the United States (and the world for that matter) undergo a “standard” lipid panel which only directly measures TC, TG, and HDL-C. LDL-C is measured or most often estimated.
- More advanced cholesterol measuring tests do exist to directly measure LDL-C (though none are standardized), along with the cholesterol content of other lipoproteins (e.g., VLDL, IDL) or lipoprotein subparticles.
- The most frequently used and guideline-recommended test that can count the number of LDL particles is either apolipoprotein B or LDL-P NMR which is part of the NMR LipoProfile. NMR can also measure the size of LDL and other lipoprotein particles, which is valuable for predicting insulin resistance in drug naïve patients (i.e., those patients not on cholesterol-lowering drugs), before changes are noted in glucose or insulin levels.
Concept #6 – How does cholesterol actually cause problems?
If you remember only one factoid from the previous three posts on this topic, remember this: If you were only “allowed” to know one metric to understand your risk of heart disease it would be the number of apoB particles (90-95% of which are LDLs) in your plasma. In practicality, there are two ways to do this:
- Directly measure (i.e., not estimate) the concentration of apoB in your plasma (several technologies and companies offer such an assay). Recall, there is one apoB molecule per particle;
- Directly measure the number of LDL particles in your plasma using NMR technology.
If this number is high, you are at risk of atherosclerosis. Everything else is secondary.
Does having lots of HDL particles help? Probably, especially if they are “functional” at carrying out reverse cholesterol transport, but it’s not clear if it matters when LDL particle count is low. In fact, while many drugs are known to increase the cholesterol content of HDL particles (i.e., HDL-C), not one to date has ever shown a benefit from doing so. Does having normal serum triglyceride levels matter? Probably, with “normal” being defined as < 70-100 mg/dL, though it’s not entirely clear this is an independent predictor of low risk. Does having a low level of LDL-C matter? Not if LDL-P (or apoB) are high, or better said, not when the two markers are discordant.
But why?
As with the previous topics in this series, this question is sufficiently complex to justify several textbooks – and it’s still not completely understood. My challenge, of course, is to convey the most important points in a fraction of that space and complexity.
Let’s focus, specifically, on the unfortunately-ubiquitous clinical condition of atherosclerosis – the accumulation of sterols and inflammatory cells within an artery wall which may (or may not) narrow the lumen of the artery.
Bonus concept: It’s important to keep in mind that this disease process is actually within the artery wall and it may or may not affect the arterial lumen, which is why angiograms can be normal in persons with advanced atherosclerosis. As plaque progresses it can encroach into the lumen leading to ischemia (i.e., lack of oxygen delivery to tissues) as the narrowing approaches 70-75%, or the plaque can rupture leading to a thrombosis: partial leading to ischemia or total leading to infarction (i.e., tissue death).
To be clear, statistically speaking, this condition (atherosclerotic induced ischemia or infarction) is the most common one that will result in the loss of your life. For most of us, atherosclerosis (most commonly within coronary arteries, but also carotid or cerebral arteries) is the leading cause of death, even ahead of all forms of cancer combined. Hence, it’s worth really understanding this problem.
In this week’s post I am going to focus exclusively on what I like to call the “jugular issue” – that is, I’m going to discuss the actual mechanism of atherosclerosis. I’m not going to discuss treatment (yet). We can’t get into treatment until we really understand the cause.
“It is in vain to speak of cures, or think of remedies, until such time as we have considered of the causes . . . cures must be imperfect, lame, and to no purpose, wherein the causes have not first been searched.”
—Robert Burton, The Anatomy of Melancholy, 1621
The sine qua non of atherosclerosis is the presence of sterols in arterial wall macrophages. Sterols are delivered to the arterial wall by the penetration of the endothelium by an apoB-containing lipoprotein, which transport the sterols. In other words, unless an apoB-containing lipoprotein particle violates the border created by an endothelium cell and the layer it protects, the media layer, there is no way atherogenesis occurs.
For now, let’s focus only on the most ubiquitous apoB-containing lipoprotein, the LDL particle. Yes, other lipoproteins also contain apoB (e.g., chylomicrons, remnant lipoproteins such as VLDL remnants, IDL and Lp(a)), but they are few in number relative to LDL particles. I will address them later.
The endothelium is the one-cell-thick-layer which lines the lumen (i.e., the “tube”) of a vessel, in this case, the artery. Since blood is in direct contact with this cell all the time, all lipoproteins – including LDL particles – come in constant contact with such cells.
So what drives an LDL particle to do something as sinister as to leave the waterway (i.e., the bloodstream) and “illegally” try to park at a dock (i.e., behind an endothelial cell)? Well, it is a gradient driven process which is why particle number is the key driving parameter.
As it turns out, this is probably a slightly less important question than the next one: what causes the LDL particle to stay there? In the parlance of our metaphor, not only do we want to know why the ship leaves the waterway to illegally park in the dock, but why does it stay parked there? This phenomenon is called “retention.”
Finally, if there was some way an LDL particle could violate the endothelium, AND be retained in the space behind the cell (away from the lumen on the side aptly called the sub-endothelial side) BUT not elicit an inflammatory (i.e., immune) response, would it matter?
I don’t know. But it seems that not long after an LDL particle gets into the sub-endothelial space and takes up “illegal” residence (i.e., binds to arterial wall proteoglycans), it is subject to oxidative forces and as one would expect an inflammatory response is initiated. The result is full blown mayhem. Immunologic gang warfare breaks out and cells called monocytes and macrophages and mast cells show up to investigate. When they arrive, and find the LDL particle, they do all they can to remove it. In some cases, when there are few LDL particles, the normal immune response is successful. But, it’s a numbers game. When LDL particle invasion becomes incessant, even if the immune cells can remove some of them, it becomes a losing proposition and the actual immune response to the initial problem becomes chronic and maladaptive and expands into the space between the endothelium and the media.
The multiple-sterol-laden macrophages or foam cells coalesce, recruit smooth muscle cells, induce microvascularization, and before you know it complex, inflamed plaque occurs. Microhemorrhages and microthrombus formations occur within the plaque. Ultimately the growing plaque invades the arterial lumen or ruptures into the lumen inducing luminal thrombosis. Direct luminal encroachment by plaque expansion or thrombus formation causes the lumen of the artery to narrow, which may or may not cause ischemia.
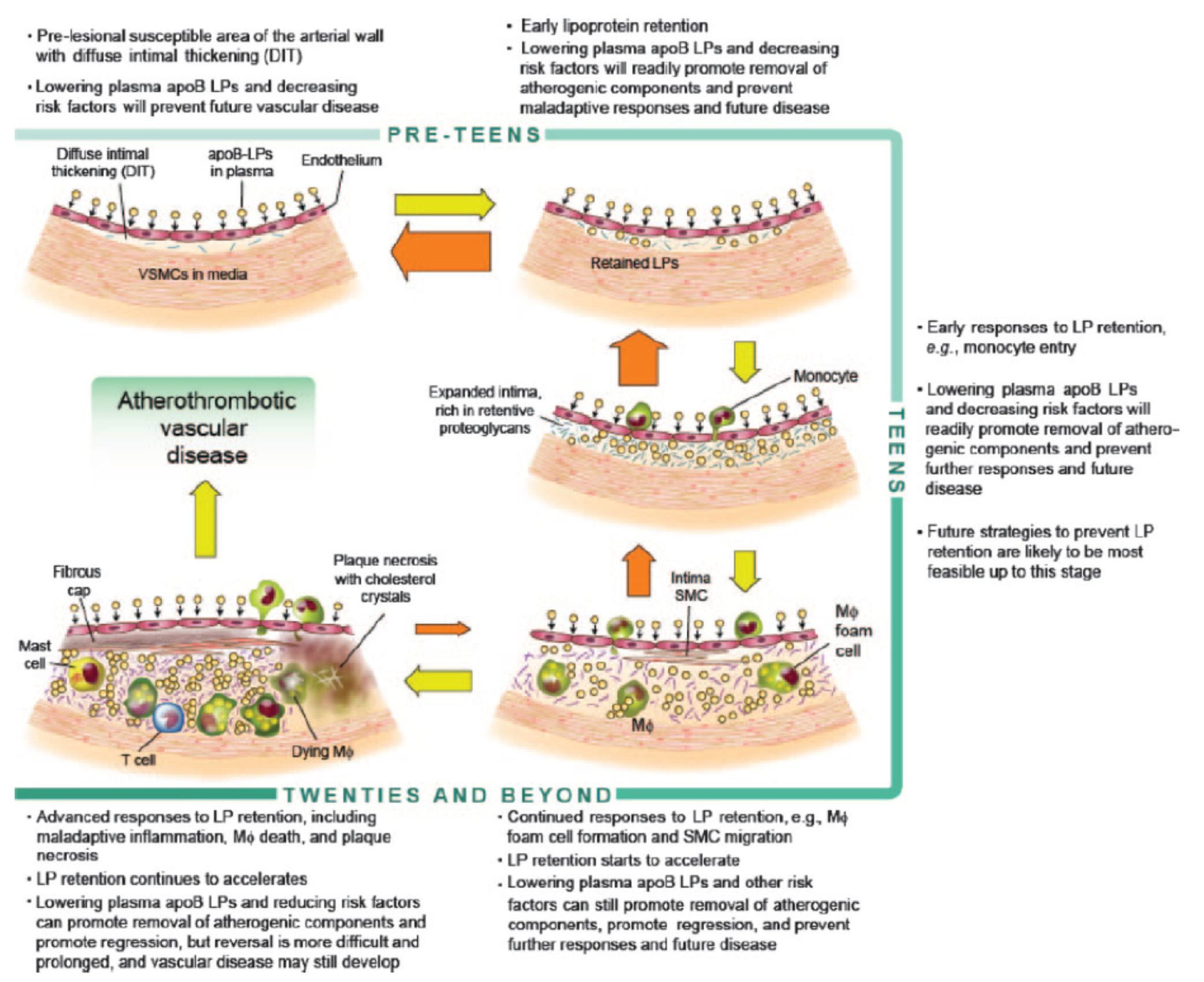
Before we go any further, take a look at the figure below from an excellent review article on this topic from the journal Circulation – Subendothelial Lipoprotein Retention as the Initiative Process in Atherosclerosis. This figure also discuss treatment strategies, but for now just focus on the pathogenesis (i.e., the cause of the problem).
In this figure you can see the progression:
- LDL particles (and a few other particles containing apoB) enter the sub-endothelium
- Some of these particles are retained, especially in areas where there is already a bit of extra space for them (called pre-lesion susceptible areas)
- “Early” immune cells initiate an inflammatory response which includes the direct interaction between the LDL particle and proteins called proteoglycans.
- The proteoglycans further shift the balance of LDL particle movement towards retention. Think of them as “cement” keeping the LDL particles and their cholesterol content in the sub-endothelial space.
- More and more apoB containing particles (i.e., LDL particles and the few other particles containing apoB) enter the sub-endothelial space and continue to be retained, due to the existing “room” being created by the immune response.
- As this process continues, an even more advanced form of immune response – mediated by cells called T-cells – leads to further retention and destruction of the artery wall.
- Eventually, not only does the lumen of the artery narrow, but a fibrous cap develops and plaques take form.
- It is most often these plaques that lead to myocardial infarction, or heart attacks, as they eventually dislodge and acutely obstruct blood flow to the portion of muscle supplied by the artery.
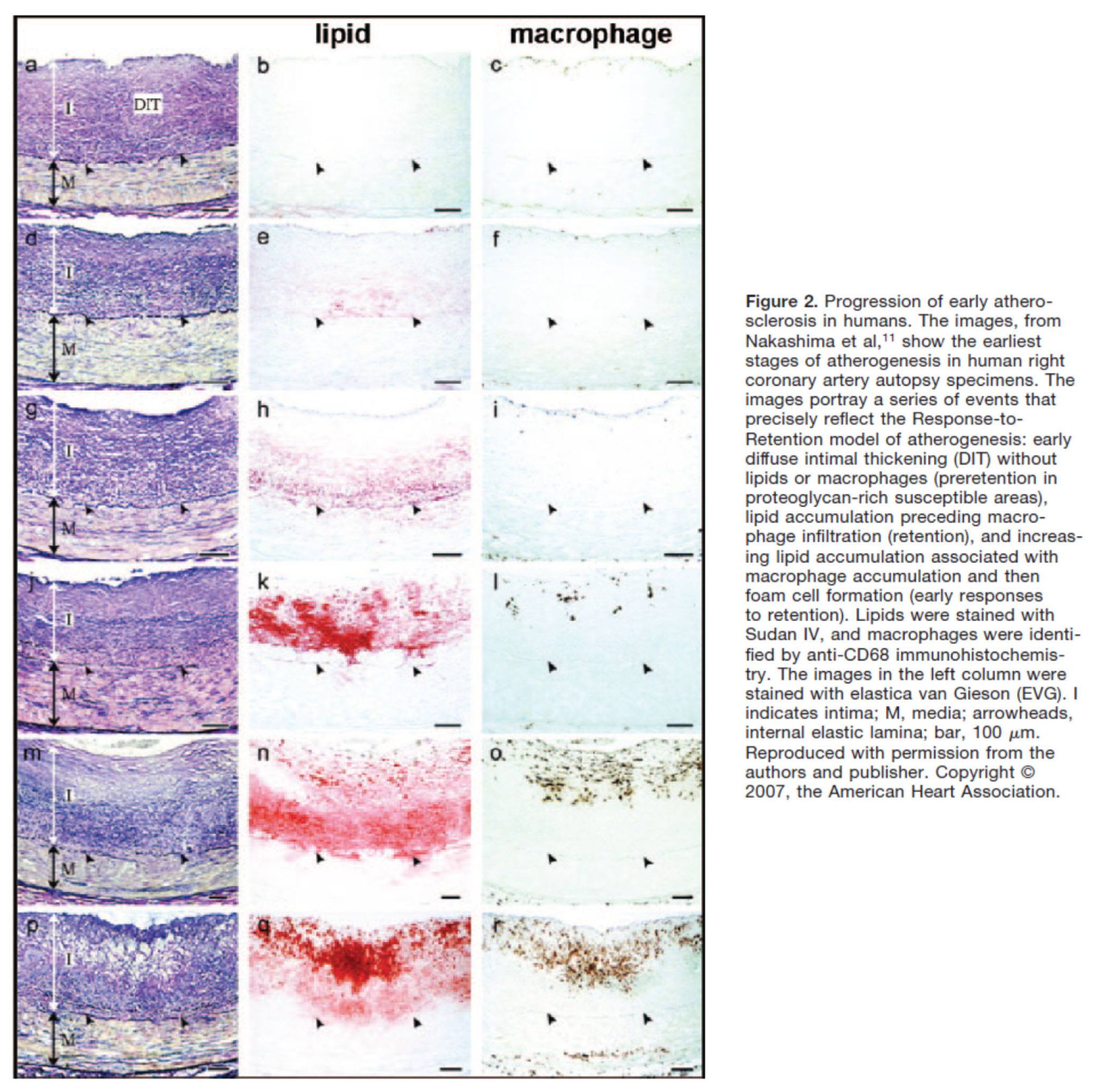
Another way to see this progression is shown in the figure below, which shows the histologic progression of atherosclerosis in the right coronary artery from human autopsy specimens. This figure is actually a bit confusing until you understand what you’re looking at. Each set of 3 pictures shows the same sample, but with a different kind of histological stain. Each row represents a different specimen.
- The column on the left uses a stain to highlight the distinction between the intimal and media layer of the artery call. The intima, recall, is the layer just below the endothelium and should not be as thick as shown here.
- The middle column uses a special stain to highlight the presence of lipids within the intimal layer.
- The right column uses yet a different stain to highlight the presence of macrophages in the intima and the media. Recall, macrophages are immune cells that play an important role of the inflammatory cascade leading to atherosclerosis.
What is particularly compelling about this sequence of figures is that you can see the trigger of events from what is called diffuse intimal thickening (“DIT”), which exacerbates the retention of lipoproteins and their lipid cargo, only then to be followed by the arrival of immune cells, which ultimately lead the inflammatory changes responsible for atherosclerosis.
Why LDL-P matters most
You may be asking the chicken and egg question:
Which is the cause – the apoB containing LDL particle OR the immune cells that “overreact” to them and their lipid cargo?
You certainly wouldn’t be alone in asking this question, as many folks have debated this exact question for years. The reason, of course, it is so important to ask this question is captured by the Robert Burton quote, above. If you don’t know the cause, how can you treat the disease?
Empirically, we know that the most successful pharmacologic interventions demonstrated to reduce coronary artery disease are those that reduce LDL-P and thus delivery of sterols to the artery. (Of course, they do other things also, like lower LDL-C, and maybe even reduce inflammation.)
Perhaps more compelling is the “natural experiment” of people with genetic alterations leading to elevated or reduced LDL-P. Let’s consider an example of each:
- Cohen, et al. reported in the New England Journal of Medicine in 2006 on the cases of patients with mutations in an enzyme called proprotein convertase subtilisin type 9 or PCSK9 (try saying that 10 times fast). Normally, this proteolytic enzyme degrades LDL receptors on the liver. Patients with mutations (“nonsense mutations” to be technically correct, meaning the enzyme is somewhat less active) have less destruction of hepatic LDL receptors. Hence, they have more sustained expression of hepatic LDL receptors, improved LDL clearance from plasma and therefore fewer LDL particles. These patients have very low LDL-P and LDL-C concentrations (5-40 mg/dL) and very low incidence of heart disease. Note that a reduction in PCSK9 activity plays no role in reducing inflammation.
- Conversely, patients with familial hypercholesterolemia (known as FH) have the opposite problem. While there are several variants and causes of this disease, the common theme is having decreased clearance of apoB-containing particles, often but not always due to defective or absent LDL receptors, leading to the opposite problem from above. Namely, these patients have a higher number of circulating LDL particles, and as a result a much higher incidence of atherosclerosis.
So why does having an LDL-P of 2,000 nmol/L (95th percentile) increase the risk of atherosclerosis relative to, say, 1,000 nmol/L (20th percentile)? In the end, it’s a probabilistic game. The more particles – NOT cholesterol molecules within the particles and not the size of the LDL particles – you have, the more likely the chance a LDL-P is going to ding an endothelial cell, squeeze into the sub-endothelial space and begin the process of atherosclerosis.
What about the other apoB containing lipoproteins?
Beyond the LDL particle, other apoB-containing lipoproteins also play a role in the development of atherosclerosis, especially in an increasingly insulin resistant population like ours. In fact, there is some evidence that particle-for-particle Lp(a) is actually even more atherogenic than LDL (though we have far fewer of them). You’ll recall that Lp(a) is simply an LDL particle to which another protein called apoprotein(a) is attached, which is both a prothrombotic protein as well as a carrier of oxidized lipids – neither of which you want in a plaque. The apo(a) also retards clearance of Lp(a) thus enhancing LDL-P levels. It may foster greater penetration of the endothelium and/or greater retention within the sub-endothelial space and/or elicit an even greater immune response.
In summary
- The progression from a completely normal artery to an atherosclerotic one which may or may not be “clogged” follows a very clear path: an apoB containing particle gets past the endothelial layer into the sub-endothelial space, the particle and its cholesterol content is retained and oxidized, immune cells arrive, an initially-beneficial inflammatory response occurs that ultimately becomes maladaptive leading to complex plaque.
- While inflammation plays a key role in this process, it’s the penetration of the apoB particle, with its sterol passengers, of the endothelium and retention within the sub-endothelial space that drive the process.
- The most numerous apoB containing lipoprotein in this process is certainly the LDL particle, however Lp(a) (if present) and other apoB containing lipoproteins may play a role.
- If you want to stop atherosclerosis, you must lower the LDL particle number.
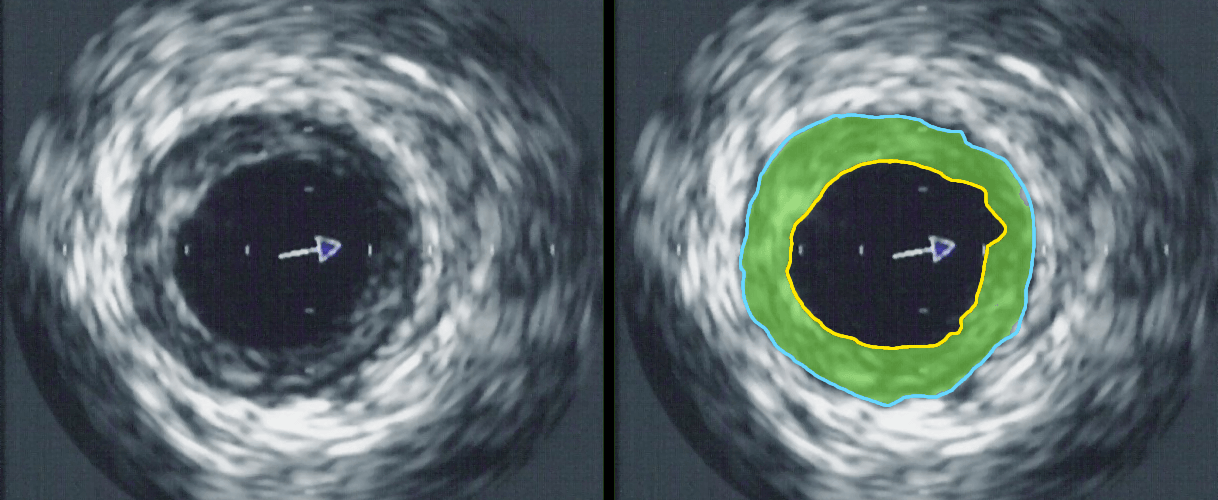
Intravascular ultrasound image of a coronary artery (left), with color coding on the right, delineating the lumen (yellow), external elastic membrane (blue) and the atherosclerotic plaque burden (green). The original uploader was Ksheka at English Wikipedia [CC BY-SA 2.5], via Wikimedia Commons


Why do particles get past the endothelial layer? Are the endothelial cells like tiles on the floor? If they are stuck down securely nothing can penetrate. Perhaps when Vitamin C is in short supply, the “glue” becomes weak or dissolves. Then LDL violates the endothelium. If we eat too much carbohydrate is the requirement for Vitamin C higher? The heart is active around the clock. Perhaps it pulls itself apart when Vitamin C is in short supply. Is heart disease a symptom of scurvy?
Cellular barriers are actually more complex than “walls” or other structures we tend to anthropomorphize them to. They are dynamic systems. I don’t actually know the answer to your question, but I am unaware of a link between HD and scurvy, and I do know there has never been shown a proven benefit of vitamin C for reducing HD.
Non cholesterol question, but somewhat related. Would it make more sense to eat about 1/2lb to 1lb or so of fatty fish per week vs.daily intake of fish oil? Fish oil is highly susceptible to oxidation particularly at higher levels. I believe the Japanese eat about 2-4 ounces of fish per day.
Depends on the type of fish. Not all equal in n-3, and the larger the fish, the more chance of contamination. A good fish oil supplement uses bait fish to reduce this problem.
I sense a disturbance in the force! I see an enormous crack in the Large/Fluffy LDL wall…
…correct.
Steve, I’m taking Crestor because I have a lot of coronary calcium (1222 Agatston units), it is growing every year, and my carotids are 50% stenosed, so I do have evidence of atherosclerosis. And there is a family history of stroke, although at 80+ years old. If you believe the lipid hypothesis, the best way to arrest plaque growth is to lower LDL. I am somewhat skeptical of this, but there isn’t much downside to Crestor that I have noticed, and even if the lipid hypothesis is wrong, there appear to be pleiotropic benefits to statins.
Thanks Harry35:
If plaque is progressing that is very interesting in light of your low particle count,particularly if it has been low for many years. From Dr.Attia’s writing here one would think that keep particles low and you will preclude material plaque progression. NOt sure that is the case.
What is your diet like- number of carbs you ingest,etc.
Hopefully Dr. Attia may get in to a discussion of endothelial dysfunction which might mean more particles at any level penetrate artery wall and contribute to plaque growth in. Particles seem to be the new hot area, and while I agree with their contribution to CAD there are likely other contributing factors,particularly with those with family histories/genetics.
Thanks again for reply and best wishes for good health.
Dr. Attia, I can definitely tell you your time has not been wasted. This series is amazing and I am so glad you are doing it. I am learning so much! Can’t wait for the next installment. Thank you, Thank you.
Great article peter. How does exercise (and type of exercise) affect LDL levels?
I’ve never seen convincing data to suggest it does.
What is the minimal time to retest lipids for apob and LDL-p after making a drug or dietary change?6 weeks?
About 6 to 8 weeks.
Hi Peter –
Very interesting facts and arguments from all sides of this controversy.
I have never fit the Framingham model. I weigh the same as in high school, don’t smoke, have always eaten a mediterranean diet, and am very active (as you know, Peter!). And I never had a high cholesterol count until about 7 years ago. At that time I was diagnosed with Chronic Lymphocytic Leukemia (CLL. It is fairly low-level o far and for that I am very thankful. However, my White Blood Cell count has been above normal for all those years. My research tells me that an elevated WBC is predcivtive of many other health problems,and so I began to wonder if it is a cauasal factor in the genesis of atherosclerosis in otherwise very healthy people because… a high WBC is a form of inflammation.
I found an article by Professor Coller of the Rockerfeller Institute who wrote there is “reason to believe that leukocytosis directly enhances acute thrombosis and chronic atherosclerosis.” I wrote to him because it seemed strange to me that I have come down with athersclerosis,and I have been looking for the reason. He replied that the epidemiology is very suggestive but that very little work has been done to trace a direct causal relation between elevated WBC counts and Athersoslcerosis. But he feels there is “reason to believe.”
What are your thoughts on this possible cause of athersclerosis?
Papa G, you are certainly correct that low-normal levels of WBC are correlated with longevity and health, which includes reduced heart disease. WBC is a pretty crude marker, of course, of general inflammation. For example, the first time I swam from Catalina Island to LA I had a friend draw all of my labs right before I jumped in the water, and again 10 hours later at the completion of the swim. My WBC rose from 5 to 20! So clearly the stress of swimming for 10 hours caused some inflammation (a normal level is considered between 4 and 11). There are other, more specific, markers of inflammation as it pertains to atherosclerosis, such as Lp-PLA2, myeloperoxidase, hs-CRP, and fibrinogen. (By the way, we will be checking all of these in you and Billy.) I think it safe to make the following statement: A high number of LDL particles is necessary, though in rare cases probably not sufficient to cause atherosclerosis. A normal (or hyperactive) inflammatory response is also necessary, but along not sufficient to induce atherosclerosis.
Million dollar question: For *most* folks, which is easier to control to the level necessary to prevent atherosclerosis?
Steve, my LDL-P has been low for 4.5 years, with one excursion when I went without Crestor for 3 months. When I started back on Crestor, LDL-P slowly came back down until it was again around 300 18 months after restarting Crestor 10 mg. During the 4.5 years that I’ve been tracking LDL-P and CAC score, CAC has doubled, so I don’t have this under control yet. LDL-P is the most important lipoprotein, but that’s not always enough, it’s just a start.
I’ve been on warfarin for the past 18 years due to hereditary coagulopathy, so that may have caused my CAC score to increase due to lack of vitamin K2. I’m hoping so, because I switched from warfarin to pradaxa a year ago, and have been supplementing a lot of vitamin K2 since then in hopes of carboxylating every molecule that needs it.
As far as diet goes, I was on a low-fat Ornish-style diet for 20 years or so, but 3 years ago I found that I am pre-diabetic and can’t tolerate carbs. Since then I’ve been limiting carbs to 30-40 grams/day, protein to 100 g/day, and total fat is 175 g/day. Saturated fat is around 50 g/day, and omega-6 fat is 10-15 g/day, omega-3 is 5-6 g/day. I’m hoping that Feynman, Volek, & Westman are correct that saturated fat is not a problem on a very low-carb diet. So far, my carotid stenosis is stable, but CAC score is going up 15-20%/year, which is not good, because CAC score is the best marker for all-cause mortality out there.
Harry 35: Keep working at it! I think Dr. Attia probably concurs with the the hi sat fat low carb crowd. Not sure i could do 30-40 carb grams a day. The interesting thing for me is the diversity of opinion regarding diet. Several lipidologists i have seen are ok with hi fat- mon and poly, but look askance regarding sat fat. Dr.Dayspring seems to be on board the sat fat is ok viewpoint and when it comes to lipid disorders/knowledge he is about the best.Calcium score is an indicator,but there are many with high calcium scores who do not show arterial closure on agiography. Arterial remodeling can take place. Again, best wishes
Maybe because of receptor GPR109A is involved;
https://www.life-enhancement.com/article_template.asp?ID=2425
Maybe is because of MGmin-LDL
https://www.sciencedaily.com/releases/2011/05/110526204953.htm
Maybe because heart disease has many factors involved;
https://integrativehealthinstitute.org/nutraceutical-approaches-to-coronary-artery-disease/
Or maybe you could try less conventional advice first;
Visit the blog of Dr. William Davis a cardiologist; he has excellent advice on how to treat heart problems.
https://heartscanblog.blogspot.com/
That said, here are a number of unconventional ways that can significantly reduce your LDL cholesterol:
• Ground flaxseed-Similar to oat bran but essentially devoid of digestible carbohydrates, it is a wonderful way to reduce LDL (small and large) and obtain healthy fiber. Use it just as you would oat bran, as a hot cereal or added to other foods.
• Elimination of wheat products-Yes, that’s right. I know it sounds weird. Elimination of wheat products is an enormously-enormously-effective strategy that reduces the small LDL particles drastically.
• Avoidance of high-glycemic index foods-Along with wheat, this includes candies, soft drinks, cookies, white potatoes, white rice, etc. This effect develops if small LDL is present.
• Raw nuts-A really great way to reduce LDL. Nuts got a bad name from the processed, salted, hydrogenated-oil soaked products that dominated supermarket shelves. Instead, look for raw almonds, walnuts, pecans, and pistachios. ¼-1/2 cup per day can yield significant reductions in LDL and do not make you fat, since high fiber and monounsaturated fat content provide a feeling of fullness that diminishes appetite for other foods.
• Niacin-Yes, yes, I know: The hot-flush effect is annoying. Niacin is vitamin B3 and I have well over a thousand patients taking it. Niacin is as effective as statin drugs in reducing LDL; it’s also the best agent available (after weight loss and elimination of wheat) for reducing the dreaded small LDL particles.
Or you could try another cardiologist;
https://blog.drsinatra.com/blog/heart-health-nutrition/choose-coq10-and-your-dentist
Or other alternatives treatment to statins first;
https://www.medscape.com/viewarticle/712122
https://en.wikipedia.org/wiki/Berberine
JohnJ — gotta say thanks for your flaxseed tip — I keep a bag of ground flax handy but hadn’t quite figured out how to add it into my diet. So just now I mixed a couple tablspoons with boiling water, mixed in a dash of cream, butter and xylitol, and it was just awesome. Like cream of wheat.
A good flax muffin (ground) in the morning is a much nicer way to get a good dose of flax. I could certainly provide the recipe if anyone wants it. I am type 2 diabetic tightly controlling by diet, eating essentially no starch which drives my sugar sky high. The essence of the flax muffin, besides the breadth of nutrition, and as you said is the almost effective absence of carb. thanks.
Dr Attia,
A statement you made above sounded like you do not like managing lipids by using serial CAC scores.Am I correct?If so why,besides the radiation?
See previous reasons given in comments. Once you establish risk, what else is it telling you? Not to mention it can be misleading. Also, don’t minimize the risk of radiation.
I use serial CAC scores to track atherosclerosis because it is the best non-invasive method of measuring risk. Dr. Budoff did a study of 25,253 patients showing that the risk of all-cause mortality, adjusted for all other known risk factors, rises smoothly from a relative hard coronary event risk of 1 at a CAC score of zero to a risk ratio of 12.5 at a score of > 1000. See https://content.onlinejacc.org/cgi/content/abstract/49/18/1860
Even tracking stenosis using CTA gives only about a factor of 6 to 7 greater risk between 0 stenosis and >70% stenosis, and the risk doesn’t get much worse going from 30% to >70% stenosis, which doesn’t allow good discrimination with increased stenosis if you have >30% stenosis, which many people have. See https://circ.ahajournals.org/cgi/content/meeting_abstract/122/21_MeetingAbstracts/A17461
The reason why CAC score is better than stenosis is that CAC score is the best noninvasive measure we have of overall coronary plaque burden, which correlates better with risk than does stenosis, because most heart attacks don’t occur at the point of maximum stenosis, and stenosis can remain the same as plaque burden increases considerably due to positive remodeling, where the artery expands to maintain the same lumen diameter even as plaque grows considerably.
CAC score is not perfect, because it doesn’t perfectly track vulnerable plaque, but it’s the best marker we currently have for total plaque burden. No noninvasive method we have yet can track plaque necrotic core and atheroma cap thickness, which would likely be a better measure. Also, CAC score can increase when vulnerable lipid-rich plaque is decreasing through calcification stabilizing vulnerable plaque. Finally, CAC score is only approximately reproducible, due to variations in the scan starting point and in interpreting the results. See https://www.ajronline.org/content/185/6/1546.full
As far as radiation goes, yes, it’s definitely always a consideration. However, a CAC score on an EBCT machine gives about 1 mSv, and on a multislice machine with >128 slices, considerably less than that. Compared to background radiation at around 3 mSv at sea level, that’s not a lot. And compared to a thallium stress test at 25 mSv, it’s very small potatoes.
If you have a high calcium score, why not supplement K2? Its cheap and relatively low toxicity… good discussion here:
https://wholehealthsource.blogspot.com/2009/03/are-mk-4-and-mk-7-forms-of-vitamin-k2.html
It may be cheap and may be well tolerated. This does not imply it actually does anything. It might, but I am not aware of any clinical data saying if you take K2 you will reduce your risk of heart disease. My advice, Ed. Worry about getting LDL-P in the zone, then take care of vit K all the other things.
Thank you for a fantastic series of articles. i am particularly impressed with the clear summeries you provide. This is science communication at its best.
One comment. can you PLEASE commment on how hypertension affects all of this? It may be somewhat selfish, but I have been lo carbing and exercising for some years but can only control my hypertension with drugs. How dangerous is hypertension anyway?
Thanks for your blog and information.
Epidemiologically, hypertension is “bad,” but this comes the standard caveats of epidemiology. Maybe it’s not “bad” but it’s a marker for something ELSE that is. Mechanistically, hypertension probably disrupts the intimal later and accelerates the atherogenic process. My personal believe is that hypertension is not a good thing and should be controlled. Many people, though not all, can do so by greatly reducing carbs.
That was such a good thought provoking post. I have so many questions but will not unload them yet. The only way science truly advances is with argument, disagreement and copious experimentation. One thing that has always worried me with this routine testing is that venous blood is tested for lipid profiling when it is what is in arterial blood that is more relevant. Obviously sampling arterial blood is a little difficult. Is there any work showing correlation (or not) of lipid measurements between types of blood? (Apologies if you have covered this somewhere.)
Not sure how much of a difference exists, but more importantly, it’s better to calibrate in the form of testing (i.e., venous) that will apply to the masses.
Hi Peter,
What is a coronary calcium score, and is this a useful test if APO-B is elevated?
Thanks,
Debbie
Speak with your doctor about whether you should have one.
I understand – thanks. 🙂
What do you consider an acceptable range for BP? I think many say ok up to 130.
Most would suggest systolic below 130, diastolic below about 80-90.
Awesome, 107 and 62 here.
Peter, finally got my LPL-P score back. I guess I’m disconcordant as LPL-P = 1486 LDL-C = 116. Met with my physician today and she prescribed Niacin. It’s good to know that there can be a disconnect between the Particles and the LDL-C. Will retest in 3 months. Triglycerides were at 33. HDL-C was at 53. I am posting info as a guide to others and not seeking medical advice. 🙂
What sort of diet did you follow to get these numbers? How about your physical specs, ie height, weight, body fat, age, sex?
thanks Paul
Just another comment on previous comments. I think veins grafted on to arteries in by pass surgery become atherosclerotic-although morphology of plaque is different and the intima layer becomes thickened. Also the pulmonary artery can become atherosclerotic despite carrying deoxygenated blood. It is such a complex area but it is good to hear about the current findings.Thanks for this whole series. I am looking forward to what is to come.
Is there an advantage to having apoB-containing particles penetrate the endothelium? Is it a beneficial function in small amounts?
I do not know of such an advantage.