A couple of weeks ago Tim Ferriss and I were having dinner and the topic of cancer came up. As some of you may know my background is in oncology, specifically in exploring immune-based therapies for cancer by exploiting the properties of regulator T-cells. But that was a long time ago. Like many of you, I expect, I’ve also been personally impacted by cancer having lost a friend to glioblastoma multiforme (GBM). I often describe GBM to people as one of the cancers that gives cancer a bad name. When I went to medical school I planned on becoming a pediatric oncologist, and though I ultimately chose to pursue surgical oncology, my interest in helping people with cancer never wavered.
Over dinner that night, Tim asked me if I could write – in about 1,000 words! – a post on cancer that would be interesting and digestible to a broad audience. “1,000 words?!,” I asked. “How about 30,000 words?,” I responded only half kidding. After explaining why I couldn’t possibly write such an abridged version, Tim talked me into it. And so, I plan to accept the challenge and hope to provide readers with such a post (it will be on Tim’s blog when I do so), hopefully in the next month or two.
For an introduction, however, I’d like take a step back and place this topic in a broader context. I don’t need to say much about cancer that you don’t already know. You probably know that about one in three Americans will develop cancer in their lifetime, and you probably know that about half of them will succumb to the disease. What you may not know, however, is that we have made virtually no progress in extending survival for patients with metastatic solid organ tumors since the “War on Cancer” was declared over 40 years ago. In other words, when a solid organ tumor (e.g., breast, colon, pancreatic) spreads to distant sites, the likelihood of surviving today is about what it was 40 years ago with rare exceptions. We may extend survival by a few months, but not long-term (i.e., overall) survival.
We screen better today for sure, but subtracting lead-time bias, it’s not clear this extends overall survival. We’ve had success in treating and even curing hematologic cancers (e.g., some forms of leukemia and lymphoma). Certainly testicular cancer patients (especially seminomatous) are better off today and those with GI stromal tumors (GIST), too. Surgical control of cancer is much better today and some local treatments (e.g., specific radiation), too. But for the most part, when a patient has metastatic cancer today, the likelihood of living 10 more years is virtually unchanged from 40 years ago.
About a year ago, I was asked to give a talk about metabolic disease to a group of physicians. But before I spoke, a very astute and soft-spoken oncologist, Dr. Gary Abrass, gave the following introduction as a way to frame the context of my talk. After all, I’m sure many in the audience were wondering what could a discussion of insulin resistance have to do with cancer. I have thought often of his words that night in the many months since he so eloquently and informally introduced me.
I asked Dr. Abrass if I could have a copy of his talk and share it with you, to which he kindly agreed. Below is, nearly verbatim, the talk he delivered that night. (Dr. Abrass did give me the liberty of tweaking the text a bit, for emphasis and clarity.)
How have we fared in the War on Cancer?
On December 23, 1971, President Nixon declared war on cancer by signing the National Cancer Act. I was going to title this, “40 years in 4 minutes,” but I think this will take me a bit longer. At the time I was a third year medical student. Two years before, Neil Armstrong had inflated our national pride by setting foot on the moon, and there seemed no scientific goal unachievable. Activist Mary Lasker published a full-page advertisement in The New York Times: “Mr. Nixon: You Can Cure Cancer.” And she went on to quote Dr. Sidney Farber, Past President of the American Cancer Society and whose name now sits atop the Harvard Cancer Center, “We are so close to a cure for cancer. We lack only the will and the kind of money and comprehensive planning that went into putting a man on the moon.” Since then, the federal government has spent well over $105 billion on the effort.
Forty years later, Dr. Farber’s prophecy remains unfulfilled. In 2012 cancer killed an estimated 577,190 people in the United States. The death rate, adjusted for the size and age of the population, has decreased by only 5 percent since 1950. And most of this decline is due to mammography screening in breast cancer and cessation of smoking, resulting in less lung cancer in men.
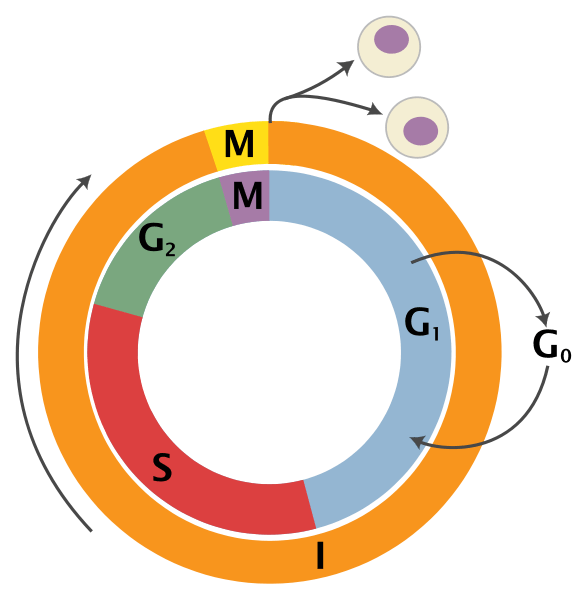
We have however developed a greater understanding of the biological and molecular basis of cancer. When I was a medical student, this graphic summarized what we knew about the growth cycle of the cancer cell.
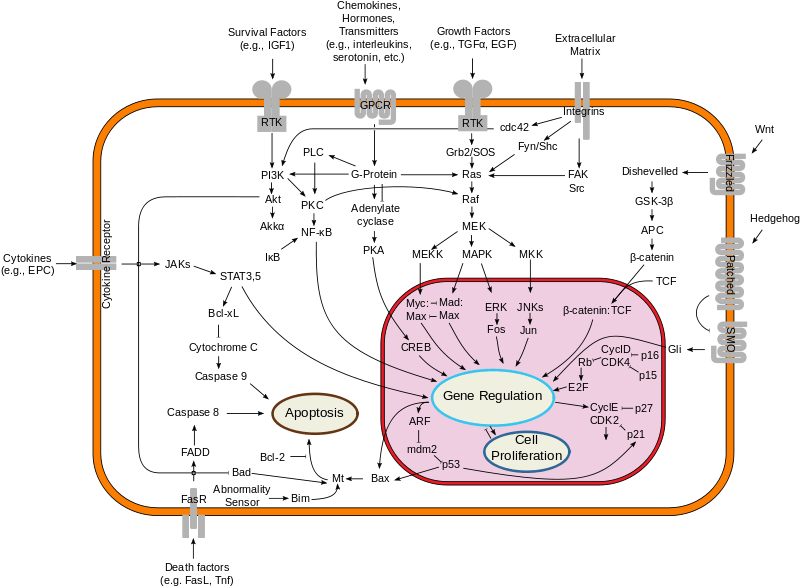
The next graphic demonstrates what we have learned, a truly overwhelming accomplishment, a dizzying array of interconnecting signaling “pathways,” and spawned a whole new field, “translational medicine.”
With the completion of the Human Genome Project, new sequencing technologies have also opened up the prospect of personal genome sequencing as an important diagnostic tool. A major step toward that goal was the completion of the sequencing of the full genome, first on James D. Watson, one of the co-discoverers of the structure of DNA. In fact, Steve Jobs had personal genome sequencing. The price is down to $1,000 and Mayo Clinic Proceedings recently had an article raising the concern of direct to consumer advertising for genomic sequencing. We are now able to sequence gene by gene, pathway by pathway, the genetic code of some cancers. New “smart” drugs have been developed that target various mutations in these pathways. And currently there are over 800 “targeted agents” in clinical development. These drugs have been described by some investigators as “The Holy Grail,” but the clinical results suggest more of a commemorative cup for a “Happy Meal.”
While there is nothing unique about this paper, it is a good example of a typical negative trial targeting the IGF-1 receptor with a monoclonal antibody. The lack of response does not make us question the role of the IGF pathway as a prime driver of malignancy, but rather demonstrates the ability of the cancer to resist therapy. It seems there is so much redundancy in the system that the cancer finds alternate pathways. The cancer cell continues to defend itself, to bob-and-weave like the arcade game “Whack-a-Mole.”
So the investigators combined the IGF-1 monoclonal antibody with various other therapies: standard platinum based chemotherapy regimens, the “small molecule” tyrosine kinase inhibitor gefitinib (Iressa) targeting another common pathway (EGFR), and also the mTOR inhibitor temsirolimus (Torisel) which targets the IGF-1 pathway a bit further along. In any case, the point is, it still didn’t work. But why?
Investigators have mapped the genome of a typical lung cancer patient and found over 50,000 mutations. That’s a lot of targets! Granted they are not all ‘driver’ mutations, some are ‘passenger’ mutations. The patient whose genome was mapped was a 51-year-old man who’d reported smoking 25 cigarettes a day for 15 years. At 50,000 mutations, it works out to one mutation for every 2.7 cigarettes.
Last year the New England Journal of Medicine published a study by Gerlinger and colleagues. These investigators looked at intra-tumor heterogeneity. They performed a molecular dissection. They found diversity within the tumor itself. Each cancer is not cancer but, indeed, it is CANCERS. In other words “all cancers are rare cancers.” Let me repeat this point. Each tumor is a collection of heterogeneous – not homogenous – mutated cells. This article has engendered some discussion and some controversy. Many say that the results of the study bring the idea of personalized medicine to a halt, or at least dramatically slow it down. Are there exceptions? Yes, but they are rare. One example of an exception to this revelation is chronic myelogenous leukemia (CML), a cancer with a known single driver mutation.
In September 2011, biologist Dr. Alasdair MacKenzie of the University of Aberdeen, speaking at the British Science Festival in Bradford, explained that researchers trying to fully understand how our DNA causes disease might not be looking in all the right parts of the genome. The past decade of genetic studies has revealed that our 3.2-billion-long-DNA-letter code is more complex than anyone could have thought. More than 98% of the human genome does not encode protein sequences. It’s been referred to as “Junk DNA” and thought not to have a function, but maybe more correctly is that we do not know the function. He refers to this as the “dark matter” of the genome. And it’s thought that some of these “alternate pathways”, in which our resourceful cancer cell seeks refuge, may reside here. If this was not complicated enough, the new field of Epigenetics has grown exponentially resulting in a widening of the battlefield.
These are factors that can affect the expression of genes without causing mutations, turning switches on and off. In terms of cancer, much of this research has concentrated on what are called “Nononcogenic stress targets.” We can stress an organism in many ways: heat, poison, starvation, suffocation or more scientifically thermal, chemical, metabolic and oxidative stress. Organisms have an ingenious way of responding to such stress. In the 1960s an assistant in FM Ritossa’s lab accidentally boosted the incubation temperature of Drosophila (fruit flies), and when later examining the chromosomes, Ritossa found a “puffing pattern” that indicated the elevated gene transcription of an unknown protein.
This was later described as the “Heat Shock Response” and the proteins were termed the “Heat Shock Proteins.” This same HSP increases survival under a great many pathophysiological conditions. The HSP70s are an important part of the cell’s machinery for protein folding and help to protect cells from stress. While it enhances the organism’s survival and longevity under most circumstances, HSF1 has the opposite effect in supporting the lethal phenomenon of cancer. These proteins enhance the growth of cancer cells and protect tumors from treatments. This remarkable protein affords a protective response to other proteins in the cell, acting as a “chaperone” preventing them from mis-folding or “denaturing,” like when a boiled egg white turns opaque. These heat shock proteins are expressed at high levels in many tumor types: breast, endometrial, lung, prostate, even brain tumors. HSP overexpression signals a poor prognosis in terms of survival and response to therapy. HSP’s are now on the radar as a key target in the ongoing battle. This protein folding stress response is a hot topic in current cancer research. I have been communicating with Dr. Debu Tripathy who is currently studying epigenetic changes and protein folding stress responses associated with obesity. This protein folding stress response affords the cancer cell a survival advantage, and we share this protective mechanism with a fly, such a distant relative in our family tree, that one can only conclude that the cancer cell has hijacked this maneuver, this protective drive for immortality from the legacy of 100’s of millions of years of evolution…such a resourceful and formidable opponent.
In any case, when the Human Genome Project was near completion, President Clinton hosted a White House ceremony and announced that, “it will revolutionize the diagnosis, prevention and treatment of most, if not all, human diseases, and that humankind is on the verge of gaining immense new power to heal.”
The hubris of it all. It’s reminiscent of the quote of Sidney Farber. Hopefully this is not tempting fate. Theologians tell us the only unforgivable sin is pride. The increasing complexity of the science is affording us quite a dose of humility. British Physicist Brian Cox said that “being at the junction of the known and the unknown is a beautiful place to be for a scientist,” but it seems the more we know, the more we don’t know. Not unlike Winston Churchill’s characterization of Russia as “a riddle wrapped in a mystery inside an enigma.” Not unlike modern theoretical physics, one questions whether we are capable of understanding the complexity of the science. Hopefully it’s not like trying to teach my dog quantum theory. We are so smart, but it seems that the cancer cell is smarter. It bobs and weaves, slips our punches, and when we back it into a corner, it defends itself in remarkable ways borne of millions of years of evolutionary acumen much of it hidden in the dark matter of our genome.
Maybe we should call a truce in the War on Cancer and concentrate on prevention. Besides smoking, the most preventable cause of cancer seems to be obesity. It is generally thought that obesity may account for about a third of many cancer types, particularly breast, colon, uterus, kidney and esophagus. Obesity is a risk factor for type II diabetes and these patients are not only more likely to get cancer, but to have poor outcomes. Other speakers will explore the relationship of obesity and cancer, the epidemiology and the science, and see if this lends support to any practical prevention measures.
Gary Abrass, M.D.
April 19, 2012
Afterword
Just as the best way to get in shape is not to ever get out of shape, the best treatment for cancer is almost assuredly not to get cancer. And that’s clearly the theme of the introduction Dr. Abrass gave me. But I’m sure many of you are asking a more important question — what happens if I or someone I care about has cancer? If you can be patient with me, I do plan to address this, to the best of my understanding, in the coming months.




Peter,
you said you were in the Seyfried “camp” on the basis of cancer; most excellent! I have become fascinated with the subject (first year medical student at Campbell University School of Osteopathic Medicine!) and have recently learned of Loran dwarfism. Are you familiar with this? I speculate as to whether the faulty GH receptors and, thus, decreased rises in insulin and glucose over their lifetime could be a reason for their seeming resistance to diabetes and cancer. Interesting stuff, and there are a few here in NC with me looking forward to joining NuSI in the fight in the coming decade.
Yes, familiar with this.
Peter: first, my apologies for being off-topic – I’m a bit freaked and am looking for some pointers to information that may calm me down. I had my first physical in years 2 days ago and my labs just came back great on lipids but with 110 fasting glucose and 5.8 A1C (estimated average glucose 120). The reason this freaked me out is that I’m pretty constantly very lo-carb (no bread, no cereals, no sodas, no sugar, a bit of fruit – chocolate, ice cream and alcohol on rare cheat binges on holidays etc.) and very high fat (bacon and egg breakfasts, cook with real lard, make my own biltong, whole milk dairy all around) in my diet so I’d have expected a lecture on lipids, not sugar! I’m also an occassional dabbler in intermittent fasting (I sometimes go a few weeks with no meals between 10pm and 1pm the next day) when I want to lean out a bit or just to cope with getting the kids off to school on time. I have this vague feeling that you may have addressed this at some point – that fasting sugars can appear (or are?) elevated on a low-carb / IF type diet but that this is to be expected and not cause for concern? If so, could you, or one of your helpful fans on these forums, please point me to that article? I’ve tried searching the site but with no luck so far. Also, do you think its worth asking for a glucose tolerance test to be sure that this isn’t a “real” problem with insulin resistance rather than whatever happens to fasting glucose on this type of diet? THANK YOU!
Hard to say, Al, without doing some detective work. I’m assuming this is an increase from your previous A1C, or you would not be freaked out, right?
Sadly, yes, the readings are worse now than they were 3.5 years ago when I was over 30 pounds heavier, eating lots of whole grains and fruit on the advice of a workplace nutritional counsellor, and had miserable HDL numbers (38). I went LCHF to drop the weight and rebounded on the HDL quite dramatically (49) but I have noticed fasting glucose creep up over time (I bought a precision Xtra reader but never got around to measuring ketones) especially since I got into IF. I had a routine to lift weights before lunch and found that if I’d had even a reasonably sized breakfast the workout would trigger reflux so the idea of skipping breakfast entirely seemed logical, especially if it would (apparently) stimulate fat burning in the process. I have appeared leaner when doing IF but the amount of glucose coursing around, particularly in the mornings, has me concerned. This morning a self-test also came back 116, had 2 eggs for breakfast and retested 90 minutes later at work and it was 121! (so much for morning cortisol!). I asked the doctor that ordered the tests whether he’d rather have me do a glucose tolerance test or a repeat of the fasting glucose and he opted for a repeat of the fasting glucose. I think I’m going to start exercising again (been off for 2 months due to an injury and work travel) and eating breakfast regularly before going in again but wondering if there is anything else I could be doing to get to a better fastng glucose number. We have a 10 month old that is a frequent source of sleep disruption but I’m not sure that a 20-30 point jump in fasting glucose can be ascribed to sleeping patterns, can it? The only other thing I can think of is coffee… I drink a lot of it (6-8 cups most days), sometimes with cream, butter and coconut oil, often black. Could this be messing with overnight insulin response?
Certainly possible. See what happens when you stop that.
Hi Al
My husband and I have both experienced increased fasting blood glucose levels since going on a high fat low carb diet almost 12 months ago. I’ve tried researching why but haven’t had a lot of success with a clear answer. The link below is the clearest explanation that I could find. We want to stay on this way of eating and I hope it isn’t causing any additional health problems.
https://thepaleodietitian.com/2012/02/14/paleo-diets-lead-to-higher-fasting-blood-sugars/
Regards
Anne
https://high-fat-nutrition.blogspot.com/2007/10/physiological-insulin-resistance.html
Hi Al,
there might be no reason to worry about the glucose level you have. Nowdays there might be less than one out of 1000 who is doing a kind of low carb/ketogenic diet and there is no valuable statistics availabel at all. Dr. JAN KWANIEWSKI in Poland has adviced his patients to use optimum nutrient for more than 40 years to cure all kinds of deseases. In his book, “Optimal Nutrition” ,translated from Polish, (I read the German one), he indicated that those who do optimum nutrition (carbo intake less than 40g per day) use to have glucose level of 110-140mg% and most conventional doctors then get alert and the patients get concerned as this used to be an indication of diabetes!
JAN didn´t deliver an explanation. But given the facts that he has had extensive expereiences and the lack of valid statistics I reckon that he might be right. After all, there has been over hunderts of thousands who have benefited from his optimal nutrition …
Hi Peter,
Great work!
I’m a doctor in Nutrition nad Corrective Exercise Specialist from Costa Rica and to my knowledge, the only one here teaching “out side the box” nutrition and have been doing that for 9 years now plus 6 more years in the Corrective Exercise domain.
I study no less than two hours every day and a few months ago I crashed into your website where I found the explanation for a theory that I had in my mind while working with triathletes. I was sure that there definetely had to be a way that an endurance athlete could access their fat as energy during competition instead of just glucose. Of course, ketone bodies were taught in nutrition school only as an undesireable effect of a diabetic state and not as you clearly explain them in your blog (my god, thank you for that!).
To make a long story short, I have found in your work a very scientific, yet, practical approach to nutrition and consider you a real teacher for me and would love to study more from you apart form the material presented here (I’m in the process of devouring all your blog).
Do you have a training system or can take someone for a week or two to learn from you?
Thank you and keep up the good work!
I don’t, Donald. But there are lots of great resources out there.
Peter,
Saw this article on my R&D newsletter, thought you might be interested in looking at it further. Looks like sugar is a pretty good culprit for increasing the chances of certain types of cancer.
Role of sugar uptake in breast cancer revealed
https://www.rdmag.com/news/2013/12/role-sugar-uptake-breast-cancer-revealed?et_cid=3668296&et_rid=54724808&location=top
“A dramatic increase in sugar uptake could be a cause of oncogenesis… we have discovered two new pathways through which increased uptake of glucose could itself activate other oncogenic pathways….
“We found that overexpression of GLUT3 in the non-malignant human breast cells activated known oncogenic signaling pathways and led to the loss of tissue polarity and the onset of cancerous growth,” Bissell says. “Conversely, the reduction of GLUT3 in the malignant cells led to a phenotypic reversion, in which the oncogenic signaling pathways were suppressed and the cells behaved as if they were non-malignant even though they still contained the malignant genome.”
I’m working on my cancer post for Tim’s blog right now and this feeds right into it…
Thanks for pointing this out for others who are interested.
Have you read Dr. Seyfried’s book Cancer as a Metabolic Disease? From the reviews by other MDs he recommends a ketogenic diet. This would seem to be something of interest to you and your readers. It would be great if you would comment on this book.
I have read it.
Processes are unique but principles of how they work are much wider in application. Oxidative stress is listed as one of many sources of stresses when in fact it is the underlying reason for the effects of almost all the rest. Because oxidative stress is the chemical interaction both normal and induced from other stresses.
For the bit where it seems they will never find the end or the start of it reminds of
“Even time indefinite he has put in their heart, that mankind may never find out the work that the true God has made from the start to the finish.”—Ecclesiastes 3:11.
Here is a much longer comment on Tim’s blog page
https://www.fourhourworkweek.com/blog/2014/01/28/cancer-treatment/#comment-256505
https://www.healthtruthrevealed.com/articles/1150/article
Cancer Survivor Jerry Brunetti Attributes Healing To Nutritional Principles of the Weston A. Price Foundation
INTERVIEWER: Pam Killeen October 6, 2006
I love this interview. Jerry Brunetti is still going strong today. He’s very down on sugar (his expertise is natural remedies for soil, cattle issues, etc. The Mennonites have him come speak to them – he had to use his nature/animal knowledge on himself. Here’s just part of the interview which agrees with Peter’s analysis in so many ways:
Jerry: In 1999, I was diagnosed with an aggressive form of Non-Hodgkins lymphoma (follicular cell). Based upon the tumor size found in my abdominal cavity, I was advised that, if I didn’t take aggressive chemotherapy, I was looking at 6 months to 2 years of life left. When I checked out the details associated with that, I found out that the survivability rates with this treatment were 35% within 5 years. I wasn’t given very good odds. I researched the MSDS and PDR to find out the side effects of the chemo agents the doctors wanted to use. Needless to say, after I reviewed the research, I declined mainstream medical treatment. The chemotherapy treatment mainstream medicine offered was called, ‘M.O.P’ and ‘C.H.O.P.’ Their approach was destructive to bone marrow, kidney and liver. My quality of life would have been pretty dismal had I chosen their protocol. I decided that they didn’t give me much of a chance. I wasn’t very excited about taking products that were cytotoxic (creating a lot of collateral damage to my own healthy tissues). In order to solve the problem, I chose my own protocols. I began searching for answers by finding out where the cancer came from in the first place. I started studying cell gene defects. The cell that has gene defects is what causes the malignancy to really take off. There are genes that are called ‘tumor
suppressor genes’ and there are cells that are activating the carcinoma. Many things can cause cancer: environmental toxins, stress and something I call ‘western malnutrition’ (not eating enough of the right things such as the different types of good fats, amino acids, trace elements, macro elements and eating the
wrong kinds of foods such as the bad fats, and sugar). Sugar is one of the main things that can predispose people to cancer. If they do get cancer, sugar really increases their susceptibility from dying from cancer because cancer is a ‘sugar junkie’. We’re consuming about 170 pounds of sugar per capita per year here in
the United States. In the early 1800’s, we consumed about 10 pounds and sugar consumption translates into insulin production. Insulin is associated with inflammatory processes. All of the drugs, COX-2 inhibitors like Celebrex, Vioxx, are all predicated on the fact that we have so many inflammatory conditions today. Inflammation is coming from a deficiency in the long chain fatty acids (EPA, DHA), an excessive amount of the omega- 6 fatty acids (which are proinflammatory) and a high amount of refined carbohydrates and sugar consumption. When people consume an excess amount of bad fats, a deficiency of good fats and lots of sugar, doctors write a lot of prescriptions for Vioxx.
Pam: Why did you avoid chemotherapy and radiation?
Jerry: Neither chemotherapy nor radiation can cure cancer. That’s admitted by the National Cancer Institute the National Institutes of Health. In Fortune magazine, March 29, 2004, there was an article illustrating that survivability rates with people who have had metastatic cancer (where cancer spreads from the primary tumor to distant organs) has not at all improved over the last 30 years. That means that we’ve seen no improvement with the four major killers (breast, prostate, lung, and colorectal cancer). Over 200 billion dollars have been spent on cancer research. There have been 1.56 million published papers on cancer and 64 billion dollars spent annually to treat people with cancer.
Pam: Cancer is a huge industry yet mainstream medicine is not making much headway in finding the cure. People need to start asking more questions, just like you did, Jerry. You initiated your own health campaign after you started doubting the efficacy of mainstream medicine.
Jerry: The reports tell people that tumors don’t kill cancer patients; rather, metastatic illness kills cancer patients. Metastatic cancer spreads to the liver, brain, bones or other vital organs. That’s what kills people with cancer. In order to contain metastasis, you have to have immunity. A strong immune system is the
only ‘drug’ that works against cancer. By the time a tumor is discovered there’s at least a billion malignancies in that tumor and they’re rapidly dividing – they’ve already ‘seeded’ the rest of the body by the time you’ve discovered you have cancer. In other words, you’ve got cancer seeds all over the body. What
determines the survival rate of cancer patients has to do with whether or not the immune system is still operating effectively.
Pam: Can you explain how the immune system works?
ETC?
Have you heard about the new research on how the immune system can regenerate after fasting? Also, have you heard about fasting as being a cure for cancer.
Hello Peter,
I apologize for reaching out in your blog comments, but your contact page suggested this as an appropriate method of contact.
I was doing some research to help StressMarq Bioscience promote their new HSP 70 Resource website: https://hsp70.com and I came across this article. Within this article you link to the HSP70 Wikipedia page, which is a great resource, but I would like to ask that you consider linking to https://hsp70.com instead (or as well as).
The website is entirely dedicated to HSP70 and I believe that anyone following the link from your article would find a very thorough resource.
Thank you for your consideration. If you have any further questions please do not hesitate to contact me.
Kindly,
Chris Whiteley
———————————————————————
bWEST Interactive
bwest.ca
Peter, I realized that you have been trying to squeeze 30 hours out of the day, though, any plans for a follow up post to this article?
Not immediate plans.
I’ve been streaming and watching parts of the new Ken Burns documentary “Cancer: The Emperor of All Maladies” and there is a segment where they follow Steve Rosenberg treating a gentleman with melanoma utilizing his cultured T-cells. I’ve really enjoyed watching it so far and when you get the time I would highly recommend taking a look. We are getting closer and even if we ultimately have to create custom therapies for every single person I believe we will get there, one way or another.
I did my post doc with Steve Rosenberg. My life could only be a fraction of what it is today without his mentorship.
Ty Bollinger’s “The Truth About Cancer: A Global Quest” (2015) is worth seeing (9 episodes). He lost a lot of relatives to cancer and goes globally interviewing naturopath experts & survivors. At http://www.thetruthaboutcancer.com you can see the first 2 of the 9-part series and get enrolled to be notified when the entire series airs again (for free, over 9 days viewable on the internet). After viewing it I bought the “Gold Package” which includes the 900-page book of the 131 complete expert (& number of survivor interviews). Ended up w two copies and just sent one to Gary Taubes. Nutrition plays a huge part in the alternative world. Mind blowing. There has been HUGE progress in the naturopath alternative world concerning cancer. In Matthias Rath, M.D.’s interview, he starts discussing the provenance of chemo (Germany) which destroys the bone marrow & immune system, a “War” with real casualties. “…the unspeakable business of defining disease as a marketplace.” (Patentable drugs which all have side effects which also need to be treated, vs. natural remedies which BOOST the immune system and DON’T have side effects and actually WORK). TY: I don’t think it’s a war against Cancer. I think it’s a war against natural treatments.” DR. RATH: It’s very true. And there’s a reason for that. We talked about concentration camps. They are surrounded by a fence. If someone tries to escape the fences of the modern concentration camp, the ones that confine the cancer patient within the parameter of conventional thinking, of chemotherapy thinking, they are being hunted.” Persecution and prosecution of the naturopaths. Watch the series. It’s not because they’re quacks and endanger us. It’s because they’re successful and very much threaten the business model.
If I’m not consuming carbs and am producing ketones, why can’t my pre-cancer,or actual cancer, cells simply feed on the glucose that I seem to have ever-present in my blood – during disciplined periods of good ketone-friendly eating my fasting blood sugar is around 80 mg/dL. What am I missing?
Dr. Attila,
I’ve read your disclaimer and believe i understand your concern. I’m 68 years old and have been battling my obesity all my life. Have recently discovered keto diet and am at home at last with this lifestyle (and doing great).
I’ve just read your 1000 word blog on cancer. My brother in law (Jim) has stage 4 mesothelioma. I’ve tried to tell my sister about the keto diet and cancer (I know it’s not a sure thing) but their oncologist told them that the keto diet would be “too severe” and they’ve declined to try it. Jim also has type 2 diabetes but is not taking metformin. His diabetes doctor told him he doesn’t really need to worry about glucose as long as it doesn’t get over 200. I don’t know what to ask except if you know of an oncologist that is using diet as a treatment? Maybe it’s you. I haven’t read all your material. I’m motivated by a similar sentiment that you expressed in your Ted talk regarding the diabetic woman.
Please direct me to any information of which you’re aware that might be of most use in this situation.
Thank you for the amazing gifts you’re bring us all with your blog and articles.
Best regards,
Jim Lynn
Jim, unfortunately most oncology practices do not focus on the role of nutrition as an adjunct to standard care and to be clear, I am not suggesting that nutrition alone can address cancer. You might find some value in the work of Tom Seyfriend: https://www.youtube.com/watch?v=SEE-oU8_NSU
Dear Dr. Attia,
Thank you for this informative blog.
I am an oncology nurse who is passionate about cancer prevention/treatment and nutrition. I am on the front lines educating patients how to eat while on treatment, how to eat to prevent recurrence, and myth-busting what is an abysmal knowledge deficit driven by the internet. But I sheepishly admit that I have never heard that a ketogenic diet could be related to prevention, and personally have never advocated for a ketogenic diet because in my educational upbringing, any diet that isn’t plant-based and balanced, low fat, etc won’t provide adequate nutrition overall. Our educational resources aren’t from Joe’s coconut cannabis treatment centers of Aruba, either. If this is the new trend and there is information out there that can change my paradigm and my patients need it, I want it.
I have done my best to read through these posts, and will continue to do so, but find it hard to get a true education amidst all the replies. Would you consider jotting down a few seminal works, or authors, for those recent to this discussion? Maybe those works or studies that you would give to your nursing staff to educate themselves?
Many thanks,
Meredith