This week an article titled Primary Prevention of Cardiovascular Disease with a Mediterranean Diet was featured in the New England Journal of Medicine. The study received a considerable amount of attention, including an article in the NY Times.
Study design
The objective of this study, as its name suggests, was to study the impact of a Mediterranean Diet on the primary prevention of CVD. Primary prevention of X implies looking at patients (ideally those susceptible to X) who have not yet had X to see if your intervention prevents X. Such trials are more difficult (i.e., larger and more expensive) than secondary prevention trials because in secondary prevention trials you start with patients who have already had X and are therefore at much greater risk of having X again.
Let’s use a relevant example. A primary prevention trial for CVD would study subjects who have never had a heart attack or stroke, and look for which treatment (e.g., a drug like a statin) reduces the number of such events (sometimes called MACE – Major Adverse Cardiac Events). A secondary prevention trial would study subjects who have already suffered some MACE and look at interventions to prevent a recurrence.
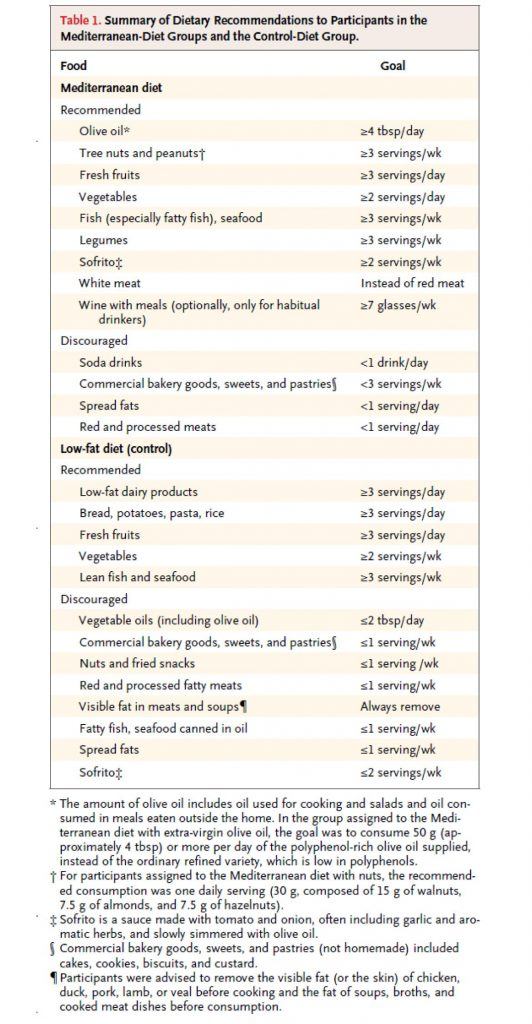
This study, a primary prevention trial, enrolled about 7,500 patients who were at high risk for CVD, but who had not suffered any MACE, and randomized them to one of three diets – two variants of a Mediterranean Diet, and a low fat diet. Table 1 shows the dietary targets. The two variants of the Mediterranean Diet were (i) one that emphasized extra virgin olive oil (EVOO) and (ii) another that emphasized nuts.
(As an aside, my 40th birthday is coming up soon and my wife suggested to my daughter that they make me a cake for my birthday. My daughter – who loves cake, of course – objected immediately by saying, “Mommy, we can’t do that…Daddy hates sugar!” A few minutes later she came back to my wife and said, “Mommy, wait, I have a great idea…we can make Daddy a nut cake!” Those of you who read this post may recall the last point I made. Suffice it to say, if I were in this study, I would have done really well on the nuts arm, though I think I eat closer to 5 or 6x the amount they were recommended per day.)
As you can see all three arms were discouraged from consuming bakery goods, sweets, pastries, red meat, processed meats, and spread fats. The authors report compliance data, but not biomarkers (if I wasn’t so short on time, I’d go back and read the other publications of this study which likely show biomarkers – e.g., insulin, glucose, HDL-C, and triglycerides – which are pretty good for confirming compliance, especially HDL-C).
So, macro point #1 is this:
Everyone in this study, almost by necessity, was consuming a very healthy diet relative to their baseline diet (if you believe most folks were on a “standard” diet, or worse yet, a poor diet, prior to enrollment, which I do). I’ll come back to this point later, but it’s worth remembering this as you read on.
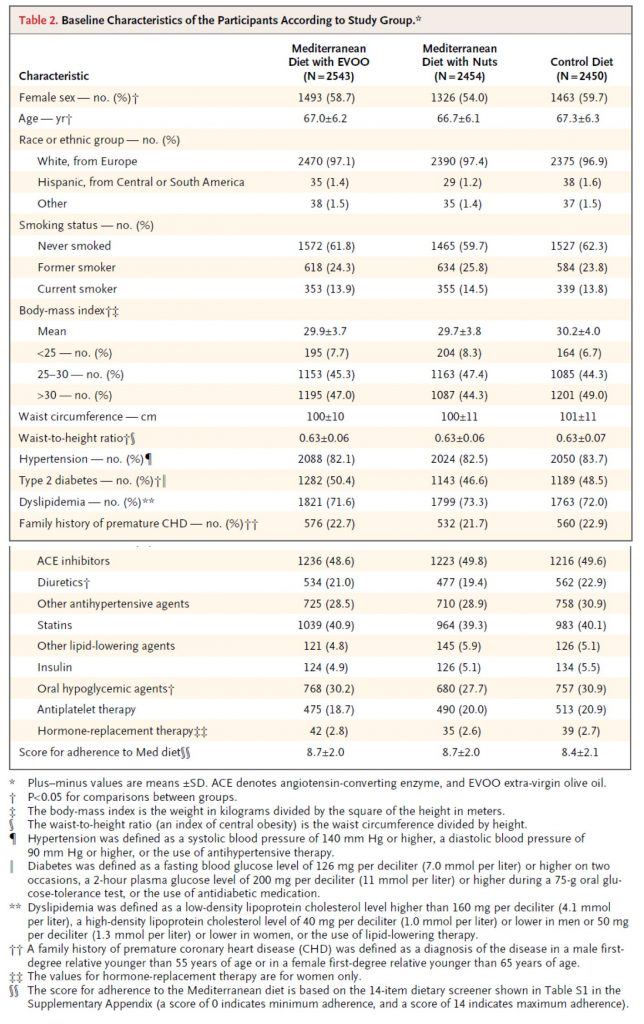
Table 2, below, shows you the baseline characteristics of the subjects in each arm. I must admit, before I saw the results of trial, but knew it was going on, I was a bit surprised at how audacious the investigators were. Primary prevention trials are really challenging! However, as soon as I read the inclusion criteria and saw this table I realized this wasn’t really a garden variety primary prevention trial, per se. Why do I say that? Less than 10% of the subjects were of normal weight. Less than 20% did not have high blood pressure. 50% had type 2 diabetes. Less than 30% had normal lipid profiles (presumably defined by LDL-C and HDL-C cutoffs). Over 40% were taking statins. You get the point. Virtually everyone enrolled in this study had metabolic syndrome.
This is not a criticism of the study, to be clear. It’s merely a statement of why this study, I believe (and hopefully will make a case for), showed a treatment effect in the setting of primary prevention with a dietary intervention. In fact, this is exactly what the authors sought in the enrollment. They specifically looked for high risk patients who had not yet suffered a MACE. In my humble opinion, this was a very good choice for two reasons:
- If they selected healthy subjects, they would have needed 5-10x the number of subjects, and
- This patient population is in desperate need of dietary intervention.
So, my only minor critique of this is the semantics of calling this a primary prevention trial. It would be more accurate to call it a primary prevention trial of patients with diagnosed metabolic syndrome.
One thing I always look for in dietary trials (and trust by now you’re also looking for) is something called performance bias, which is very common in dietary intervention trials. In fact, you’ll recall it was the main flaw of the meta-analysis I wrote about a while ago. The authors of this particular study (you can read about this in the methods section) did a good job avoiding this.
This brings me to macro point #2. This study would have been better if the “control” arm (in this study, the low fat arm), was actually a true control relative to the “standard” patient diet. For example, this might look like the following 3 arms: standard fare diet vs. low-fat diet vs. Mediterranean diet (pick one of the 2 from this study). The drawback of this approach is that patients in the “standard fare” would almost certainly have a performance bias working against them. The other two groups would have a sizable intervention effect, while this (true) control arm would be left on their own.
The final point I want to make is more of a so-called teaching point. Broadly speaking, there are two (and an emerging third) types of studies in human nutrition:
- Efficacy studies – studies that elucidate (under the strictest most controlled conditions ever used to study humans) the mechanism of action of food. In other words, these studies ask, “How does factor X or factor Y actually work at the mechanistic level in the body?”
- Effectiveness studies – studies that elucidate to what extent free-living people will adhere to a dietary change, and determine the long-term safety and effectiveness of that change. In other words, these studies ask, “Does this dietary intervention work over time, and what are the risks and benefits?”
- Econometric studies – studies that elucidate (under free-living conditions) how to change people’s behavior, by changing the defaults, the economic forces, and the cues. In other words, these studies ask, “How do we induce people to change behavior – to eat healthy — once the science provides definitive answers about what that behavior should be?”
Obviously, this study is in the second category, as virtually all “diet studies” are. I mention this for the reason that while it’s tempting to speculate on a mechanism of action in this study, there was not a single design element in this study to elucidate such things. So, at best, we are really looking at the difference between two dietary interventions.
What happened in this study?
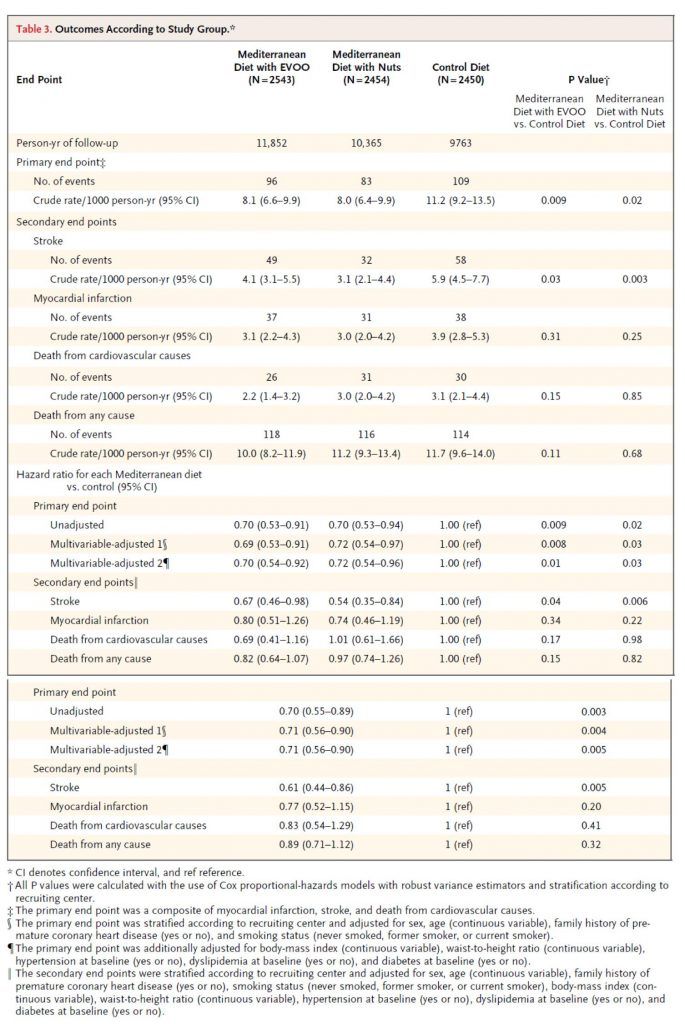
Table 3 shows the outcome of the study and commensurate hazard ratios. I won’t walk you through this table in its entirety, but I’ll show you how to read one row of each.
Consider the first row, the primary end point (recall: this was defined as a composite of myocardial infarction (MI, “heart attack”), stroke, and death from cardiovascular cause). The first row shows the number of crude events. Of course, to see this in an apples-to-apples fashion the number needs to be normalized to a common denominator, in this case events per 1,000 person-years. So, the row that’s particularly important is the one that shows 8.1, 8.0, and 11.2 per 1,000 person-years. (Note, one uses person-years to also normalize for and remove any impact of time in study.) Next to each number I’ve listed above are two numbers in parentheses. These are the 95% confidence intervals. So, even though the first is listed as 8.1, you can be “95% sure” the actual number is between 6.6 and 9.9.
How can you tell if this is “statistically significant?” Most of us don’t possess the ability to do this in our heads. So, the authors do it for us in the last two columns. The right-most column compares the control (low-fat) to the Med Diet (nuts), while the column to the left of that compares the control group to the Med Diet (EVOO). The number shown, called a p-value, is defined as the probability the difference you’re seeing is due to chance. The smaller the better, and generally a number below 0.05 is considered to earn the moniker “statistically significant.” (Not to be confused with “clinically significant,” which I’ll discuss below).
Before we go back to the other endpoints, let me comment quickly on the hazard ratio for this endpoint. A hazard ratio is essentially the probability of an event in the treatment group divided by the probability the same event occurs in the control group (hence, control groups have a hazard ratio of 1.0).
So, the hazard ratio of 0.70 means there was relative risk reduction of 30% for the Med Diet relative to the control diet. This should not be confused with absolute risk reduction, which I’ll get to shortly. For the sake of time and space, I will not go into the details of unadjusted and multivariate adjusted analyses.
But there was no difference in MI or death?
As you can see from Table 3, there was no statistically significant difference in death (CVD or otherwise) or MI across the three groups. It’s very tempting to make the following mistake:
“Hey, none of this matters, because you won’t live longer.”
Remember that pesky little statistical thing called power. This study was powered (at 80%) to detect a difference in the primary outcome, which it showed. In fact, the intention-to-treat was greater than 7,500 because the authors expected no more than a 20% relative risk reduction. But they saw a 30% difference, and the study was halted early.
So, we don’t actually know which of the following statements is correct:
- This dietary intervention does not result in a difference in MI or death; or
- It does, but this study was not large or long enough to detect it.
Very important distinction. I can’t emphasize this enough.
Back to absolute versus relative risk
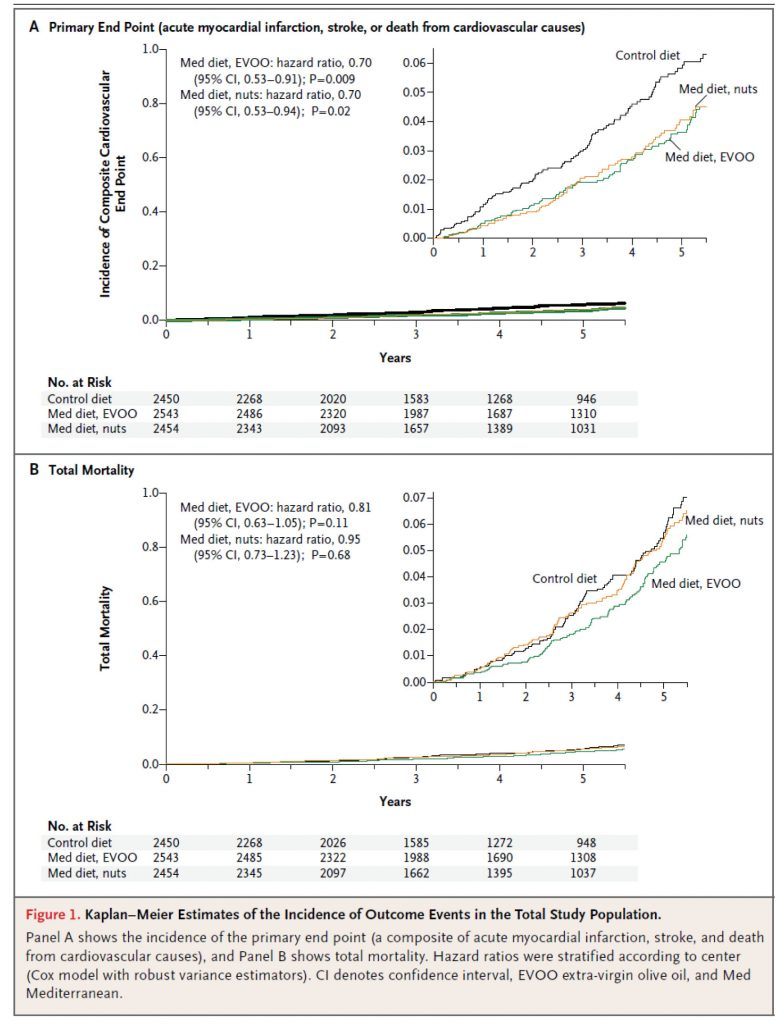
Figure 1, below, shows the Kaplan-Meier estimates for the primary end point (A) and total mortality (B). Each figure shows both the full y-axis (which always varies from 0 to 1) and, in the upper right corner, a zoomed view to show the difference. The fact that the zoom view is necessary tells you something about the absolute risk reduction. It’s small.
Here’s a quick calculator to determine the absolute risk reduction (ARR). When you plug the numbers in from this study (I’ll just do it for the low-fat vs. EVOO group), you’ll see the ARR is 0.3065%. The reciprocal of this number is 1/0.003065 = 326. This is called the number needed to treat (NNT). This means that 326 people would need to undergo this dietary intervention for about 4 or 5 years to prevent one “count” of the primary outcome.
Is this important? Or, to be more specific, is this “clinically significant” as I asked earlier? Well, it depends on the intervention. If this study were testing a drug with a 1% major toxicity rate, the answer would be emphatically, no. Obviously, we could not justify treating 326 people to save 1, if 3.26 people (on average) will experience a major toxicity!
Conversely, if this study were testing a drug with a 1% minor toxicity rate (e.g., headache) and a 0.001% major toxicity rate (e.g., kidney failure), the answer is not so clear. For perspective, most drugs fall into this second category (e.g., statins, aspirin).
I could go through the exact same argument using Quality-Adjusted Life Year (QALY) instead of toxicity. While this approach is not used in the United States (perhaps it should be), it is certainly the cornerstone of other healthcare systems, such as the NHS in the United Kingdom.
While it’s beyond the scope of what I wanted to write about today, the key to sorting through this grey zone is better defining patient susceptibility and outcomes in large clinical trials. For example, I would argue that the data on statins could be much better if the treatment target was LDL-P or apoB instead of LDL-C, especially in high risk patients with metabolic syndrome, at least half of whom have discordant LDL-P and LDL-C.
So, what to make of the modest ARR in this study? Well, question 1 should be: what is the toxicity of a Mediterranean Diet? Question 2 should be: what is the QALY impact of a Mediterranean Diet?
I can’t really answer either of these questions. The former is objective but has not been quantified to my knowledge. The latter is subjective, and each person needs to answer it for themselves.
My conclusions
Overall, I think this is a good study, and a better study than the study prompting it, the famous Lyon Heart Study. That said, I would have much preferred to see only one Mediterranean arm (in retrospect this is obvious, of course, given the lack of difference between them), in favor of a true control or another arm such as Very Low Carb.
It’s impossible to guess what the ARR would have been for the Med Diet if the control was a standard fare diet (complete with 138 gm per day of sugar!), rather than a much improved low fat diet. If I had to guess, I’d ballpark the ARR at 1-5%, for a NNT of 20 to 100 people, but this is nothing more than speculation. Remember, I think the Low Fat arm in this study experienced an enormous benefit over their baseline.
In the coming months and years, as NuSI begins funding remarkable clinical trials, we’ll have plenty more to discuss…
Photo by Carlos Santiago on Unsplash





Studies Methodology Questioned
1….. You could learn the same thing or similar by putting 10 people in a metabolic ward for three months and measuring their arterial health – and extrapolating that arterial health into a reasonable heart/stroke event outcome –
saving millions – accomplishing the same in three months instead of five years of fatally flawed nonsense (people failed to follow diet)
Arterial health can change rapidly – plaque and calcium decrease or increase or or stay the same – other markers of arterial health can also make rapid changes – again – extrapolating these findings into a heart risk event makes sense – at least to me – contrary opinions welcome (let me know how stupid I am)
Jeff, not stupid at all. In fact, I struggle with this exact question more than any other in my role at NuSI. Are there ways to study and fully elucidate the impact of food on health without hard outcome studies if we can identify good enough biomarkers?
One of the problems in asking Spaniards (or Greeks or Italians) to use corn oil or other such poison instead of olive oil is like asking a Canadian to watch cricket instead of hockey. It’s just not going to happen. No wonder compliance was poor in the “control” group.
Good job bringing forth some of the good points we can take from this study (and for explaining the power correctly).
As a Canadian, I can vouch for that. I don’t think I’ve ever watched a cricket match..
Peter,
I recently had both a VAP Profile and a NMR done on the same day but the results are off somewhat on TC and Triglycerides. Which is more accurate analysis?
A little history,
Was low fat forever, TC 221, HDL 42, Tri 105, LDL 158
Doc wanted me to take Statin, so instead I went low carb.(perhaps 50 net carbs a day)…..some good news some bad….TC 282, HDL 73, Tri 98, LDL 189 (lost 5 lbs and 2 inches on waist, and got lean)
Then a year later went very low carb (less than 30 net carbs a day) with a lot of nuts and a fat shake every morning, but TC 359, LDL 259, HDL 67, Tri: 115, LP(a) 6.0
Got nervous, added ‘safe starches’, perhaps 10-15% of calories, cut out nuts, cut out fat shakes, continued 2-3 tablespoons of coconut oil (in coffee) a day.
Got VAP Profile and NMR. Results slightly improved but different.
VAP Profile
TC 315
HDL 67
Tris 103
LDL 220
LP(a) 7.0
Sub-class:
LDL1-Pattern A 49.8
LDL2-Pattern A 67.5
LDL3-Pattern B 60.5
LDL4-Pattern B 0.0 (good?)
NMR Profile
TC 292
HDL 69
Tris 71 (way off from VAP PROFILE)
LDL-C 209
Small LDL-P 711 (good or bad?)
LP-IR Score: 10
LDL size 21.3 nm
Why are the results so different? Would you recommend I start a statin? If not, what can I do?
Evan, I can’t give medical advice or comment on this.
Evan, just curious about your history, given the results you’ve had in various trys
“A little history,
” Was low fat forever, TC 221, HDL 42, Tri 105, LDL 158″
What was the version of low fat you were on.
As we saw in this recent study of the Mediterranean Diet, the fat as a percentage of calories was 37% for the low-fat group. The American Heart Associatons version of low-fat is about 30% of calories as fat.
While the Ornish, Esselstyn low-fat heart healthy types, often portrayed as the sterotypical “low-fat” doctors both limit fat to 10% of calories.
Where did your years of eating low-fat fall in to that spread of <10% to 37% seen in this study?
And what was the low-fat level when you got those results ( TC 221, HDL 42, Tri 105, LDL 158)
Sure. I understand.
Can you comment on which is a more accurate test, VAP or NMR and why any difference?
Thanks in advance
Evan
NMR is better, but VAP doesn’t actually do what NMR does, so it’s not apples-to-apples.
ARGH!!! That darn doctor thing!!! Evan keep us posted if you take this to another site and get some answers or recommendations. (note: fully understand why Peter can’t answer)
I started my journey Jan 1.. Got both a VAP-NMR. Doc didn’t know what an NMR was, that was a knock down drag out. Last time I was in (thyroid) the blood draw assistant, whispered into my ear, “the Doc is now ordering those NMR things for everyone”, this made me chuckle. Any way my biggest fear is my TG/HDL ratio (right now) 5.2 gets better, but my over all numbers blow up. Since I can’t consult a MANUAL, your information may be helpful if I find myself in same situation. This probably goes for others as well.
So don’t be put off if Peter can’t answer you, I am sure he (sort of) wants to, and we are all paying attention.
KC
Peter –
I have been prescribing low carb/real food (high fat) to most of my patients (family doc) and am now checking NMR lipoprofile on all patients that are borderline or that I am considering statins for. However, I don’t have a good resource for numbers to treat – do you have any info on that? Most of these people have been LDL-P >1500, with a few in the 2200 range, and I just can’t find any guidelines of where a statin should be used in people who have not had previous cardiac disease with a high LDL-P.
Also, I follow several blogs now (dietdoctor, authority nutrition, protein power, etc) and have been searching for any and all info on constipation in the low carb diet – seems to be a common issue and just wanted to see what all the low carb gurus are doing. Any advice as to where to look? (aside from the usual psyllium flakes, miralax, etc – anything better while doing low carb that you know?)
Thanks!
Jenn Lentz
The guidelines (see the work of Sniderman, Dayspring, and company) exist. The challenge, however, is the context of the results. I’ll elaborate in Part X of my cholesterol series. In the interim, check out the work of Rakesh Patel (also a family doctor) in AZ: https://azsunfm.blogspot.com/2012/09/font-definitions-font-face-font-family.html
Hi Peter
Could you comment on the study linked below, which basically found that substituting high omega 6 linoleic acid for saturated fats actually increases risks of cardiovascular disease. “Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis” [https://www.bmj.com/content/346/bmj.e8707?view=long&pmid=23386268]
In Table 1 of the study, only two oils had low Omega 6 linoleic acid: canola and olive oil. Olive oil is said to be an important constituent of the “Mediterranean Diet”.
Could you also comment on canola oil, as there seems to be some reservations about the heathiness of this oil by readers on certain health websites.
In another post, at another time. Far too complicated to address with a short response, which is all I can muster these days.
Another great post — thanks!
What about weight change during the study? Specifically, did the control group continue to gain weight while the test groups maintained or loss weight? If so, might that not explain the important observed differences?
Surveys like the ones in this study are notoriously inaccurate, and biomaker analyses are limited. It seems like weight change would be an important objective measurement of what and how much the subjects ate. More importantly, as you noted these subjects were mostly overweight with metabolic syndrome, and many were on statins. Almost any weight loss (or weight improvement relative to the control group) would be beneficial in reducing the tested events.
I don’t have access to the study details. Do you? Did they consider weight change at all?
Thanks!
I think there was actually a bit of weight gain.
Excellent review: Unless before and after NMR is done to measure LDL-P and correlated with events, I do not place much validity in any diet study. Ornish/Esselstyn low-no fat seems to get some results as do high fat low carb diets. Note I am only speaking with regard to CAD/Heart events. Weight loss seems to be accomplishable by many different kinds of diets, and as you have written most have success as they eliminate/drastically reduce sugar and junk carbohydrates.
While we don’t know why, I would bet that the many who still incur any event under any diet are not at LDL-P level for their risk profile. Of course, that is just my view.
My ldl-p of 2320 scares the heck out are me.
Not sure how much comfort I should derive from a 71 TG and nearly 70 hdl.
I believe cholesterol is essential and low is bad. Would explain cognitive issues etc for those on statins.
I also believe a low ldl in itself is not the solution. Check the Get With it Guidelines by the AHA and ASA showing half of those with events had ldl below 100 and 3/4 had ldl below 130. Yet very very few with high hdl had an event, almost regardless of ldl levels.
Question is if cholesterol is essential but if your body can’t get it, I mean extract what it needs from the bloodstream, and then what? Reduce via statins?
If genetically disposed to high cholesterol / faulty receptors is stains the only choice?
However for non genetic reasons like faulty receptors due to diet or thyroid issues, what can be done?
Can’t find a flow chart on the Web to run diet and supplement changes.
Some of what I found was:
Supplement with iodine, along with selenium and copper and Zinc. But all very balanced and measured amounts. I did that for 4 months. Did feel better, much less fatigue etc. Did low low carb induce adrenal fatigue?
I added some carbs in the former of safe starches like white rice, to the tune of 60 more carbs a day, total then to about 15 percent of calories. I did notice far less muscle fatigue during Cardio and a far easier time going to the bathroom. (low carb does reduce mucin production). Even with these carbs weigh stayed low.
Before alot of nuts (mostly almonds) and I mean alot, and didn’t notice much change in TC.
However I am pretty convinced my high ldl is driven by high saturated fat intake. Once I added daily Attia fat shakes my numbers popped 60 points. Removing them it fell by same amount. Since going low carb I eat a ton more meat and cheese which I believe is the cause of my high ldl. But I believe this food and the subsequent lack of sugars grains and most carbs helped my hdl and TG.
The 64,000$ question is, Is it worth it, high ldl for better everything else.
I do realize that on the same diet I have a few of my buddies who saw no pop in ldl but saw the benefits on the other lipids. However, I have run across a subset of individuals in the same predicament as me.
My next self experiment perhaps is the exclusions of all cheese? Hopeful that I can achieve this before I drop dead or my cardiologist scares me into a statin.
Evan, I want to suggest you investigate another line of thinking… i.e. maybe higher LDL-P is not bad if inflammation is low? See Robb Wolf’s AHS12 talk beginning at 18:40 where he explicitly notes of his own discussions with our own Dr. Attia here on this subject…
Video – https://www.youtube.com/watch?feature=player_embedded&v=ns2oS1WXDvc
Slides – https://www.slideshare.net/ancestralhealth/ahs-2012
I agree we don’t know from scientific studies yet, but we have at least one piece of anecdotal evidence from Dr. Rakesh Patel’s self treatment of a paradoxically *improved* arterial thickness score in the presence of an *increase* in LDL-P…
https://azsunfm.blogspot.com/2012/09/font-definitions-font-face-font-family.html
If you don’t have it already, one thing you might consider is genetic testing (e.g. via 23andMe) and look at your APOE allele status. The behavior you describe is consistent with something that appears to be common for people with at least one APOE4 allele. What we don’t seem to have definitive evidence on is whether this is good or bad in such cases?
Check out these recent videos by Dr. Tom Dayspring (who Peter has referenced on the blog). I don’t know that it answers your question per se about LDL-P but will show you the latest thinking. (I don’t think there is a conclusive answer based upon the state of our knowledge and if there is a lack of inflammation). Depending on your age, perhaps you will need additional and/or more invasive testing. If no plaque, no worries . . .
https://www.youtube.com/watch?v=joTrnnFHw-E
https://www.youtube.com/watch?v=jKS3A_uRVdU
(1) How does consuming 4tbs of EVOO per day compare with the amount and type of fat in the typical American daily diet?
(2) In general it seems that the direct consumption of olive oil while satiating the need for fat does seem to discourage taking in excessive amounts . (Your thoughts please!)
Hi Evan,
Have you seen this Graph?
https://perfecthealthdiet.com/wp/wp-content/uploads/2011/09/GregoryBarton.jpg
I am in fear, I will see the same results as you, as I have Hypothyroid. I have talked to my Endo about taking Armour T3/T4, but he wasn’t buying it, so I am now currently flooding my system with T4 to improve my TSH.
KC,
Yes. I have followed Paul quite frequently on PHD in my attempt to avoid a statin via diet modification.
I really wish there was a ‘recipe’ for me. I am willing to stick to something proven and make sacrifices. Heck, I haven’t had pizza or pancakes or more than a nibble of bread since November 2010. I forgot what frozen yogurt, ice cream or chocolate cake tastes like. But heavily buttered veggies, steak, cheese, whole eggs seafood are more than a fantastic trade off.
Energy levels super and high hdl gives me some comfort. My primary says he agrees with my diet but my ldl is just too high not to take a statin. I have low body fat, and bp of 120/75 and gained 5 pounds since college (25 yrs ago) mostly muscle mass.
Perhaps Peter provides suggestions to optimize lipids in Part X of his cholesterol series…….. I’m waiting for it.
Fact was when I went low fat my TC was much lower, and ldl much much lower, and but hdl dangerously low…. Even dropping under 40. This low hld resulted n a TC/hdl ratio just over 5x. Now I’m just under 4x due to high hdl. But is that enough to save me? TG/hdl is at 1x. But does all this make up for ldl-p of 2300 particles?
I like it at 70ish like now, but as per Peters series ldl-p is all that matters (not my big fluffy particles), so at 2300 particles I am at a loss. 95+ percentile. Just horrible.
And many many others have the same problem and are seeking solutions. Start googling, you will find them.
FYI. My doc said statins are safe and any side effects can be reversed since I will be monitored. Drink the cool aid, I mean statins?
Evan you and I have almost exact stories. I have also been on diet since abt. 2010, however my journey on low fat is much like Peters in that if I look at a carb I gain weight. NOTE: I too have not had pizza for 3 year, or anything else bad for that matter, with exception of Thanksgiving.
Once I discovered metabolic syndrome it all came together for me. In 2012 I discovered I was hypothyroid about mid year which is exactly the same time I discovered met. syn. The one thing that seemed to be a reoccurring theme was Paleo/LCHF/ Atkins community with thyroid issues is your exact outcome and fingers crossed hopefully not mine but probably so. So on Jan1 I scheduled a battery of tests, and got in a fight with my Doc about NMR’s. I was able to win him over (sort of) . He agreed June 30 we do second round of testing. Meantime we are trying to treat the thyroid with minimal response. I gently broached the T3 data but my GP didn’t feel comfortable with his knowledge on T3 so he sent me to Endo. The good thing is, thanks to Peter, Jimmy, Jeff, Eric, etc. I was able to talk to the Endo at a level which I think allowed him to upen up to me. But he too doesn’t want to mess with T3 he stated it acts much like speed on the body and only prescribes as last resort .
Like you I have good BP, FEEL BETTER than I have for a long time, some things that have plagued me since my 20’s have disappeared. I am at abt. 80 to 85% fat, and haven’t deviated since Jan1. As I said before I am worried my TC is going to blow up on June 30s testing. I have more data to give to my doc after I pull him off the ceiling about T3 to try to make my case.
At one point Peter stated he was going to do a Thyroid article. Fortunately (unfortunately for me) Peter is busy trying to save the planet. There are some great T3 articles on PubMed, and it looks to me that there needs to be more research on T3 effects on LDL /LDL-p. To me, it appears thatT3 has a massive effect on LDL. Problem may be it is too hard on the system as a whole.
KC
Although studies in vitro and in hypothyroid animals show that thyroid hormone can, under some circumstances, modulate the actions of low-density lipoprotein (LDL) receptors, the mechanisms responsible for thyroid hormone’s lipid-lowering effects are not completely understood. We tested whether LDL receptor (LDLR) expression was required for cholesterol reduction by treating control and LDLR-knockout mice with two forms of thyroid hormone T(3) and 3,5-diiodo-l-thyronine. High doses of both 3,5-diiodo-l-thyronine and T(3) dramatically reduced circulating total and very low-density lipoprotein/LDL cholesterol (?70%) and were associated with reduced plasma T(4) level. The cholesterol reduction was especially evident in the LDLR-knockout mice. Circulating levels of both apolipoprotein B (apo)B48 and apoB100 were decreased. Surprisingly, this reduction was not associated with increased protein or mRNA expression of the hepatic lipoprotein receptors LDLR-related protein 1 or scavenger receptor-B1. Liver production of apoB was markedly reduced, whereas triglyceride production was increased. Thus, thyroid hormones reduce apoB lipoproteins via a non-LDLR pathway that leads to decreased liver apoB production. This suggests that drugs that operate in a similar manner could be a new therapy for patients with genetic defects in the LDLR.
For anyone interested in the use of T3 in hypothyroidism, I strongly suggest my own endo’s new book:
https://www.amazon.com/Functional-Approach-Hypothyroidism-Traditional-Alternative/dp/1578263875/ref=sr_1_1?ie=UTF8&qid=1362831552&sr=8-1&keywords=Kenneth++Blanchard+thyroid
He probably has more experience with combined T4/T3 therapy for hypothyroidism than anyone in the world.
Be forewarned, however, that after many years of experimenting he has found that neither conventional nor holistic medicine has gotten this subject right, despite very strongly held dogmas on both sides. For example, he has found that while, contrary to conventional dogma, almost all hypothyroids need T3 as well as T4 replacement, the optimal T3 dose is at least an order of magnitude lower than that commonly used by “alternative” practitioners, whether in the form of pig thyroid extract (e.g., Armour thyroid), Cytomel, etc.
He has also learned much more about how to construct optimal therapy, including seasonal dose variation, the limitations of standard thyroid blood work, and the relationship between hypothyroidism and other health problems. Highly recommended.
I will say, though, that while I feel better than I ever have under his care, it hasn’t prevented my LDL-C from skyrocketing on low carb. I’m not convinced that’s a problem, but if lowering LDL is judged to be an important goal, not sure this is the way to do it.
KC,
Perhaps Peter can correct what is wrong in what i am about to say, but from what my very limited medical knowledge surmises is that the benefits of statins may actually be driven from their inflamation lowering abilities.
That lower inflamation and not lower LDL is what helps to avoid CHD or stroke.
With that in mind, do you think doctors, and perhaps Peter, would say that taking an aspirin a day (or a baby aspirin) is a vary safe way to mitigate potential adverse effects of high ldl. That is, ldl by itself is not a problem as long as inflamation can be avoided.
Then heck, high ldl, hdl etc would be desired as it good at containing infections etc……
Have you read Paul PHD book, the Perfect Health Diet, great read (but i wish he picked a different title). At half the cost of a co-pay at my doc office, getting this book is a no brainer.
Other good links to review (in my attempt to bring comfort to myself i am not about to drop dead at any moment):
https://www.ncbi.nlm.nih.gov/pubmed/19074985 – Diabetics taking statins had an increase of 2% in total death rates and an increases of 31% in death from cardiovascular diseases.
https://www.ncbi.nlm.nih.gov/pubmed/18757089 – Virtually no difference in mortality rates and cardiovascular incidents between statin-takers and placebo.
https://jama.ama-assn.org/content/291/18/2243.abstract – No difference in overall mortality between statin-taking women and non. Heart disease mortality was actually HIGHER for women who began taking the drugs *before* they had heart disease.
https://www.jnrbm.com/content/10/1/6/abstract – A HUGE observational study following statin use in the general population of Sweden between 1998 and 2002. Statin use tripled. Rates of heart disease were unchanged.
https://archinte.jamanetwork.com/article.aspx?volume=170&issue=12… – Here’s a meta-analysis study which finds that the risk reduction for all cause mortality when taking statins is an almost insignificant less-than-1% for all groups. Many statins also include an anti-inflammatory, which could easily explain the entire reduction.
and this article: https://www.drbriffa.com/2010/11/15/recent-review-on-statins-ignores-body-of-evidence-that-suggests-these-drugs-dont-work-through-cholesterol-reduction/
and this: https://chriskresser.com/the-truth-about-statin-drugs
Two questions.
Who is the only person to win 2 (non-shared) Nobel Prizes?
Do you think this person’s advice can be followed?
Well, Linus Pauling believed that plaque, CHD, etc was the manifestation of stressed and “cracking” arteries which Lp(a) got stuck onto. Peter, please correct my mis-understanding I won’t be offended.
Veins don’t have the same stresses, and I guess don’t need the same collagen to repair its membrane walls. As we all know, our lipids (esp LDL) are in the veins too (our blood is taken from there) yet plaque doesn’t form there.
That being said, cutting to the chase, Pauling advises (well advised – before his death), that hardening of the arteries can be avoided and even “fixed” by:
Increasing collagen via high doses of vitamin C.
And, being the chemist that he was, and a specialist (and genius) on bonding between elements etc, that if you can “inactivate” LP(a) by binding it with lysine it won’t “adhere” to arteries.
Dubbed the Pauling Protocol and composed of natural vitamins and amino acids, no drug company wanted to sponsor studies etc.
So then what?
Well, what I found is compelling. And Pauling was a winner. Perhaps that is worth its weight in gold, in and of itself?
Better than a statin huh?
Well, I am starting it. Wish me luck.
I finally got the results of my blood test, and the basic numbers were better than my last test. The “doctor” I mentioned in my last comment turned out to be a Physician’s Assistant, only they didn’t tell me that.
When I complained about having a person who isn’t really a doctor giving me advice, the nurse said, ” Well, just because some people can’t afford to get State certified as a doctor, doesn’t mean that they’re not just as qualified.”
I said, “You’ve got to be kidding!” This guy gave me tons of moronic advice!” She took off.
Apparently, there’s only one doctor at this walk-in clinic, and they give you a PA unless you ask for the doctor.
Business as usual in GHI NY health insurance care.
Anyway, I’ve been on a low carb diet for about nine months, and my HDL went from 41 to 46, My LDL went from 110 to 99, my Triglycerides went from 99 to 73,
However, there were some tests I’ve never seen before done:
Oxidized LDL- 45
OxLDL/HDL – 38
CRP High Sensitivity 1.33
All three of these were a little higher than the safe range. Should I be concerned about them?
The new PA they gave me didn’t say a word about them…
TIA
Here we go again–care to comment on THIS one?
https://shine.yahoo.com/shine-food/like-bacon–sausage-and-hot-dogs–too-bad–cause-that-stuff-l-kill-you–new-study-finds–174609721.html
I eat only “uncured,” nitrate and nitrite free prodcuts like Applegate Farm. Safer? I personally do not believe at ALL that the “fat” is the factor.
There is a positive association between women who have had breast augmentation and suicide rate. Do you think getting a breast augmentation increases the likelihood a woman will go on to kill herself?
From the source paper:
We cannot exclude residual confounding, in particular
due to incomplete adjustment for active and passive
smoking. The sub-group analysis for processed meat
showed heterogeneity according to smoking, with signif-
icant associations only in former and current smokers
and no significant associations in never smokers, which
is compatible with residual confounding by smoking.
Although EPIC includes ten European countries with a
wide range of dietary behaviors, we observed relatively
little heterogeneity in the association between meat con-
sumption and overall mortality.
Also, this the paper that they rely on for their statement:
“Both high saturated fat and cholesterol intake have been found to be related to
the risk of coronary heart disease.”
Mozaffarian D, Micha R, Wallace S:
Effects on coronary heart disease of
increasing polyunsaturated fat in place of saturated fat: a systematic
review and meta-analysis of randomized controlled trials.
PLoS Med2010,7:e1000252.
Amateur’s reading of this paper’s issues – All of the studies were pre-1993, may be selection bias, does not address cholesterol at all (so where does the original paper get that claim?!), the largest study (n=9,000) is larger than all of the rest combined and is a feeding trial and shows the opposite effect (and I am sure that there are more).
Another example of the need for NuSI?
Only if she can’t find a bra that fits! ; )
Thanks–I’ll continue to enjoy my bacon without wondering if it’s killing me. Now, the bourbon . . . !
I wasn’t really trying to be glib. I’m not saying that just because something has a positive associate it is categorically false. It just doesn’t contain causal information. Maybe something (e.g., a chemical) in the implant does drive women to kill themselves at a higher frequency than the general population. Without ever having looked at this problem, I do not find that hypothesis particularly compelling, but it does not guarantee it’s wrong. Similarly, it’s possible that bacon is bad for us, but this study does not prove it, even to the most modest level of evidence available by epidemiology (e.g., Hill’s criteria).
So, I choose to still consume bacon, because I believe, on average, and in most populations, bacon consumption is merely a marker for bad eating habits. If you want to better understand this topic, I did a post on red meat once. Should have “red meat” somewhere in the title.
Peter, Love your work and cite it often in conversation with others, so want to note I was a bit blunt in concurring with Bob up above. So I want to address directly to you in case I’m missing something…
Per that comment, Table 2 indicates that the control group was instructed to eat >3 servings/day of “potatoes, bread, pasta and rice” and the study group was asked to avoid “commercial bakery goods, sweets and pastries.” Not knowing what they actually did, stands to reason that unless the study group got really about making their own bread and pastries, they were differentially reduced in consumption of grains. To make matters worse as regards confusion by lay readers, wherein bread and pasta are understood to be an acceptable part of the Mediterranean Diet, why is this not a fatal flaw? How can the study possibly make the conclusions that it does? Am I the one missing something?
Certainly a flaw, though I’m not sure if fatal. This, of course, underscores the challenges of free-living studies. They can’t be perfect, but experimenters should strive to equalize the bias.
Peter,
For months I have read your blog without comment. In the past few years, I have also read dozens of low-carb books, including those by Gary and Atkins. Your example inspires me more than all of these books because it’s tangible and because I’m an endurance runner fighting the uphill battle of “we all need to carb load to perform well”. I’m also 47 and have a very strong history of heart disease and diabetes in my family. Although I don’t understand everything you are saying (you are beyond smart ;-), I do find tremendous hope in your work, passion, example and dedication. THANK YOU a thousand times over for fighting the good fight!
Melisa Zachrich
Findlay, Ohio
Thanks so much, Melisa. Very happy to hear this is helpful.
Evan,
Thanks for all the links. Yeah I have read all of those. I too, like you have armed myself with just about all the information I can find on the subject. NOTE; I did click through all the links. I too am looking for a certain amount of confirmation bias to make sure I am not going to keel over. Anyone who thinks people can’t be programmed I urge them to try eating a “healthy” high fat diet, then walk into a supermarket.
Bill,
Thank you for the link. Had not seen that book, will be downloading that onto the old Ipud. MORE Information!
KC
Keep me posted as well.
BTW did u see my post above (got to scroll up to our prior discussion) on March 15 on the Pauling Protocol?
I pinged Jaminet on it as well before I start it.
Have u done a heart/artery calcium scan? I think much comfort or overwhelming fear will result from it. I will ask my doc for one.
Curious, did u add carbs? I did as per Paul’s recommendation,but just 15 percent in form of white rice (safe starch).
Helped on…eh hemm…dry stools, and muscle soreness due to cardio.
No weight gain!
KC and Peter,
Good summery here.
Peter, as a MD what is your take on this? Voodoo science? Safe to try? Makes scientific sense but not validated via controlled studies?
Tx
Oops here is link,
https://ehealthforum.com/health/topic10681.html
Sorry bout that.
Evan, I’ve been reading your posts, and made a follow-up of your post on March 4. You may have missed it since it was so far up in the thread. Or you may not want to respond, which is OK.
Wade H March 9, 2013
Evan, just curious about your history, given the results you’ve had in various trys
“A little history,
” Was low fat forever, TC 221, HDL 42, Tri 105, LDL 158?
What was the version of low fat you were on at that time?
As we saw in this recent study of the Mediterranean Diet, the fat as a percentage of calories was 37% for the low-fat group. The American Heart Associatons version of low-fat is about 30% of calories as fat.
While the Ornish, Esselstyn low-fat heart healthy types, often portrayed as the sterotypical “low-fat” doctors both limit fat to 10% of calories.
Where did your years of eating low-fat fall into that spread of 10% to 37% ?
And what was the low-fat level when you got those results ( TC 221, HDL 42, Tri 105, LDL 158)
Hello Wade,
Sorry, missed your original post.
Perhaps the best representation of my low fat diet was Ornish like, 10 -15% max.
Breakfasts would be cheerios with skim milk or an egg white omelet with dry whole wheat toast and some lettuce or tomato. A treat would be high carb pancakes with syrup.
Lunch, grilled chicken sandwich on multigrain bread and mustard, or perhaps turkey lettuce and tomato.
Plenty of salads for lunch with non or low fat dressings.
Dinner would be pasta with a can of tuna on it (and perhaps plain old tomato sauce and spices). Or, more salad and grilled chicken. Or ground turkey burgers (not the high fat turkey, but 99% lean), same for ground beef, i would buy 90% lean and then drain the fat like crazy.
And let me tell you, i was always hungry! No matter how many calories i consumed.
I could and would 3BIG bagels in one sitting.
Snacks during the day were all fruits (some candy too like good and plenty but no chocolate bars etc). Plenty of apples….many in fact, bananas too, pears, oranges……
Mayo, butter, oils, nuts, avocado, egg yolks, all avoided……cheese was a rare treat.
sorry Wade, i tend to be detailed (and long winded) when it comes to diet.
short answer, 10-15% MAX with the TC 221, HDL 42, Tri 105, LDL 158.
I am convinced very low fat is bad for optimal HDL.
I am also certain that saturated fat increases LDL in ~30% of people, but regardless, beneficial on TG and HDL
But does that really matter?
My Lp(a) of 7 gives me some comfort.
What eating style do you follow? Results?
Wade,
my low carb diet was 10-15% by fat. perhaps closer to 10%
egg white omelets, dry whole wheat toast
cereals with skim milk
turkey lettuce and tomato with mustard on multi-grain
pasta with a can of tuna and tomato paste (hey its good!)
grilled chicken on salad
no butter
fat free frozen yogurt
sugary candies
diet soda
bagels with low fat cream cheese
low fat this and that, etc
my diet is completely different now
feel great
appetite under control
lost a few pounds
damn LDL !!!
Lp(a) a 7 though…can i be proud of that??
Hello KC and Wade.
CORONARY CALCIUM SCAN RESULTS……….looking inside my arteries…..got the test!!! some suspense first.
Reposting here as I wanted to give you both an update (and to hear how I made a cardiologist lose a bet)
Recap, low fat diet for 20+ years (age 18-42)
Lipids at age 27 (on low fat diet):
TC:155, LDL 96, HDL 43 TG 82
Fast forward to age 42 (still on low fat diet)
TC:221, LDL 158, HDL 42 TG 105
numbers crept up, same diet, same exercise, etc
Doc says take statin. Research lead me to low carb.
Age 43 (one yr on low carb)
TC:282, LDL 189, HDL 73 TG 98
Doc scared of LDL, prescribes statin. I tear up script.
Age 45 1/2 (~2 more yrs on low carb with last 6 months adding more carbs, perhaps 10-15% and sticking close to PHD with supplements)
TC:292, LDL 209, HDL 69 TG 71
(note LDP-p 2323, with small LDL-p 711, LP(a) 7, LP-IR 10)
Doc sends me to cardiologist as I say I don’t want a statin and I refer to my great HDL and TG numbers and ratio of nearly 1.0, LP(a) of 7, LP-IR of 10, my 7% body fat, and 120/76 BP.
Cardiolist says, do you want to take a statin?
I say No, (of course).
Would you go for a coronary calcium scan?
Sure.
If calcium shows up will you take the statin?
I just say, I’ll take the test.
Cardiologist called today. Seemed quite upset to give me the good news. ZERO. Nada. Nothing on the scans.
I said now what?
Doc says, The right thing to do is take the statin due to high LDL and father who had heart attack at 50 (but smoked 30 yrs and was overweight), the later (family history) being thrown in my face.
But I got a zero, shouldn’t I just be retested in 3 yrs or so.
“yes”
conversation over…..
question: Did I make the right call?