I remember one of my mentors in surgical residency made a very important distinction for me. He said, “Peter, never forget what you are getting paid to do, and what you are doing for free.” You see, there are some aspects of being a surgeon that are not particularly enjoyable. The hours are long. Sometimes you’re asked to intervene in a situation where there is no hope, and you feel you may only make things worse. A lawsuit is just around the corner. But there are many aspects of surgery that are pure bliss. Though I’m no longer a surgeon, some of my fondest memories in life stem from moments there. Anastomosing a transplanted kidney into a patient (especially the renal vein anastomosis, which is the easiest to screw up). Endartarectomizing a plaque-filled carotid artery. Telling a patient and their family that you were able to remove the entire tumor in their colon, and that the lymph nodes were free of tumor.
Want to learn more? Check out our article on replacing sugar with allulose and our Ask Me Anything podcast all about sugar and sugar substitutes.
What my mentor was saying to me was that those moments of pure bliss are not what we’re getting paid for. In fact, we’d probably pay to do them! What we’re getting paid for is the time we have to be away from our family. The long hours, smelly call rooms, and bad hospital food. The cost of medical malpractice insurance.
What does this have to do with the toxicity of sugar? Well, nothing actually. But I constantly remind myself of this when I feel my personal stress and anxiety mounting. The past year has been a whirlwind of kinetic energy that makes my days in residency, 80 to 100 hours of work every week, seem tame and almost boring. Most of what I do today is wonderful, but some is not. I fly about 12,000 to 15,000 miles a month (in coach, no less) and spend about 8 to 10 nights a month in hotels. Red-eyes are a regular part of my existence. My day starts between 4:45 and 5:00 am and goes until 11 pm or later. I can’t put in words how much I detest traveling and being away from my family. So, I guess, that is exactly what I get paid to do. (By the way, do not feel sorry for me. I’m pretty sure all of this is self-imposed, but I still hate it.)
So, do you want to know what part of my role at NuSI gives me bliss that rivals the finest moments of surgery? It’s exactly what I did a couple of weeks ago (and, fortunately, something I get to do often). I spent a day with some of the best and most thoughtful scientists talking about their work and how we can make it better.
Can you imagine (assuming you’re as much a geek as I am) getting to pick the brains of the best scientists for hours on end? Finding out why they are obsessed with the questions they ask? What keeps them up at night? What are the challenges they face? What’s preventing them from resolving uncertainty?
I would pay to do this part of my job. This is the bliss described by Joseph Campbell. And this meeting a few weeks ago was a great example of it. This particular meeting focused on sugar research, specifically the metabolic impact of sucrose, high fructose corn syrup (HFCS), and fructose. If you need a quick refresher on the distinctions, this should help. Spending so much time with this group got me thinking about a broader issue, which is actually the focus of this post: Is sugar toxic?
What does ‘toxic’ mean?
Before we dive into the main focus of this post, we need to get crystal clear on our semantics. Too much tomfoolery has already taken place for the simple reason that many people don’t understand the words they use.
For the purpose of rigor, let’s turn to the pharmacology literature for a clear understanding of toxicity. Even though we all have an understanding of what “toxic” means, let’s be sure we’re understanding the nuance. If you troll the medical textbooks you’ll eventually settle on a definition something like this (from Harrison’s Principles of Internal Medicine):
TOXICITY: The degree to which a substance can harm humans or animals. Acute toxicity involves harmful effects in an organism through a single or short-term exposure. Subchronic toxicity is the ability of a toxic substance to cause effects for more than one year but less than the lifetime of the exposed organism. Chronic toxicity is the ability of a substance or mixture of substances to cause harmful effects over an extended period, usually upon repeated or continuous exposure, sometimes lasting for the entire life of the exposed organism.
The first thing you may notice from this definition is that toxicity is actually subdivided into acute, subchronic, and chronic toxicity, based on how long it takes to progress from exposure to insult and the number of exposures necessary to cause insult. This constitutes what I call:
Important point #1 – don’t confuse acute toxicity (what most people think of) with chronic toxicity.
Acute toxicity and the LD50
An example of acute toxicity is acetaminophen (abbreviated APAP, but commonly referred to by its trade name, Tylenol) overdose which, if significant enough, requires a liver transplant within days to prevent death from fulminant liver failure. (As an aside, this is particularly tragic because the liver, unlike the heart, lungs, and kidneys, can’t be supported extracorporeally; so if a person overdoses, and the liver is irreversibly damaged, they will need a liver transplant within days, or they will die.)
The question, of course, is what dose of APAP is toxic? (In this case, the toxicity is liver failure, which results in near-immediate death.) Enter the LD50. LD50 stands for “lethal dose required to kill 50% of the population.” How is this quantified for a given substance, including APAP? Obviously, we don’t do randomized trials of increasing APAP doses in people until we definitively resolve this. Instead, we (I’m using ‘we’ pretty liberally here – obviously I have never done this) do 3 things typically:
- Carry out the above experiment in animals to accurately estimate LD50 (in the animal);
- Mathematically model the best human data available and try to estimate LD50 (in humans);
- Compare the two estimates.
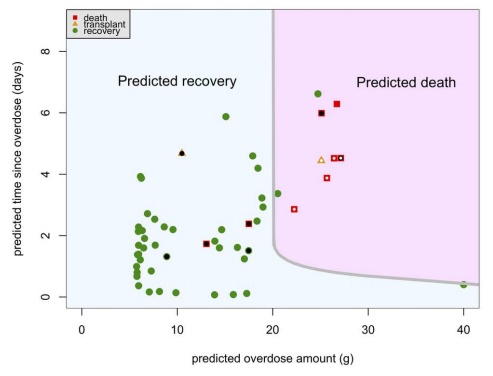
Not surprisingly, the answer to #1 is usually much higher than the answer to #2. In the case of APAP, the LD50 in rats depends on age, but is probably somewhere between 800 and 1,500 mg/kg, suggesting a 75 kg human would expect toxicity (on average) between 60 and 110 gm (120 to 220 extra strength Tylenol tablets!). Is this likely? Let’s go to step #2. Below are data integrating known human toxicity with a mathematical model to estimate LD50, as a function of APAP dose (x-axis) and death versus survival over time (y-axis). As you can see, this analysis suggests LD50 in humans is closer to 20 gm. (These are data from humans who did not undergo liver transplant, except in the case of the yellow triangles.)
I’ve looked at several other models and they all appear to suggest about the same thing, The LD50 of APAP in humans is about 10 to 20 gm (10,000 to 20,000 mg or 20 to 40 Extra Strength Tylenol tablets), and most sources point to the lower end of that range.
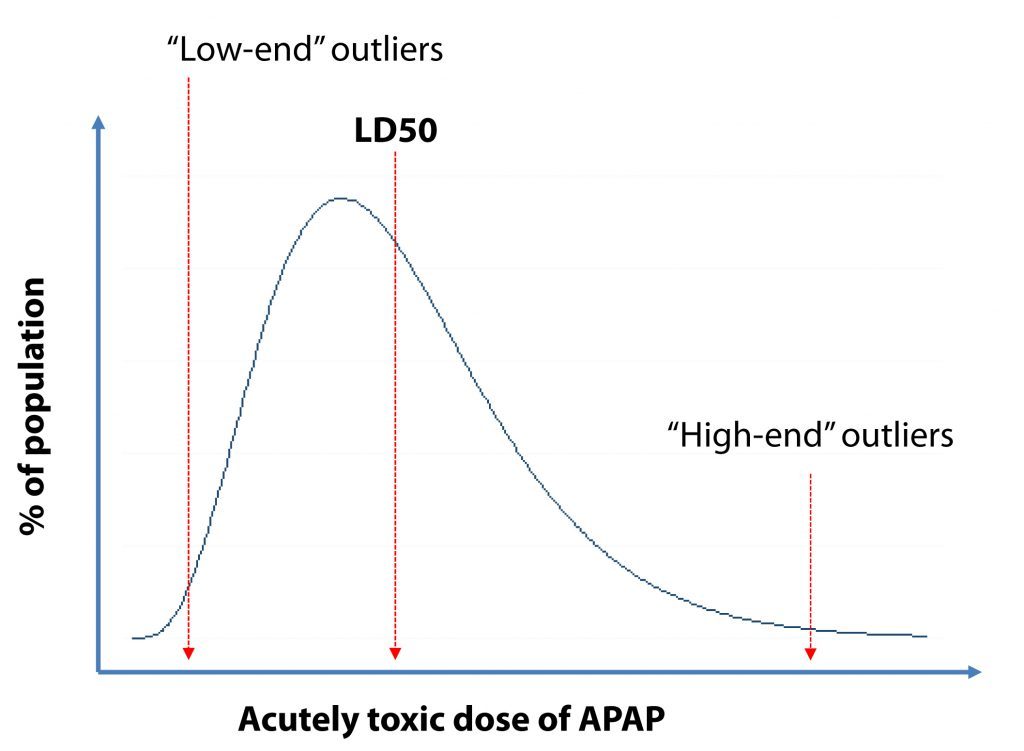
So what’s my point of this? My point is that there is a statistical distribution (see figure below) of the toxicity, which is why it’s called LD50 and not “LD” (which would imply everyone would experience toxicity from the same dose). In other words (let’s simplify and ignore weight differences since this is in mg/kg and just assume I’m talking about a 75 kg human), some people will experience toxicity at 6 gm and others not until 16 gm. In the figure above, you can see one person lived, despite a dose of 40 gm (given that he received the antidote early enough) and another at 25 gm, without antidote.
Important point #2 – there is a spectrum of susceptibility to any toxin.
What about chronic toxicity?
Sticking with APAP as our example, it turns out that much lower doses than the LD50, if taken day after day, are also toxic to the liver. How much lower? As you’ll see below, the answer is highly dependent on the timing of these doses and other host factors. In general, though, some authorities suggest repeated daily doses of more than 6 gm are toxic, while repeated doses below 4 gm daily are rarely toxic. The point is that much smaller doses, if taken repeatedly, are still toxic.
Important point #3 – just because a dose does not result in acute toxicity does not mean it can’t or won’t cause chronic toxicity.
Complicating things a bit further…
There is no reason to expect physiology to be simple or binary, so adding one more layer of nuance to this already-longer-than-you-wanted-to-read-explanation is the following point. Factors such as alcohol consumption, underlying liver disease, viral infections, and genetic susceptibility are highly influential in both acute and chronic toxicity from APAP. This shouldn’t be surprising, of course, though it complicates our discussion. Since APAP taxes hepatocytes (liver cells), taking other drugs that do the same, consuming alcohol (uniquely metabolized by hepatocytes), or having underlying liver disease are invariably going to reduce hepatic reserve. So, an individual’s ability to tolerate APAP is highly dependent on both measureable (e.g., cirrhosis) and idiosyncratic variations.
Important point #4 – host factors play a significant role in susceptibility to toxins.
Parting shot
I would be surprised if anyone reading this has not taken or used APAP (i.e., Tylenol or some generic equivalent). In fact, most of us have experienced great relief from it. That does not change any of the points above.
Important point #5 – the term “toxin” does not imply something is “bad” or universally harmful.
What does APAP have to do with sugar?
There must be some reason I’ve gone through all of this, right? After all, the question of sugar’s toxicity is a somewhat polarizing one. On the one hand, folks like Dr. Rob Lustig have argued that fructose is harmful at the doses most people are consuming it today. On the other hand, folks like Dr. James Rippe have argued the opposite. Having read just about every paper and review article on this topic (I think) over the past year, I can say the debate has many facets, which I’ll outline briefly:
-
- The PRO sugar folks** argue that sugar, while void of any nutritional value, is no more or less harmful than a calorie of any other nature. In other words, it has no unique metabolically harmful consequence.
- Depending on affiliation, some of the PRO sugar folks debate back and forth about the advantages or disadvantages of sucrose (natural sugar from beets, cane, etc. composed of a linked glucose and fructose molecule) and HFCS (synthesized sugar composed of 55% fructose, 45% glucose mixture). (There may be some merit to this discussion, though it would probably qualify as a “higher order” term. To a first or second order approximation, they are biochemically equivalent.) It appears this debate is a convenient way to avoid really confronting question/point #1. The “natural sugar” producers can point at the corn growers, and vice versa, without really confronting the jugular question. Both of these groups (sugar and corn) downplay research on pure fructose (which is pretty rare in nature and even our current environment), which is a valid point, though a distraction from the issue above.
- The ANTI sugar folks argue that sugar is indeed a “unique” macromolecule distinct from other carbohydrates. Whether solely due to the fructose content, the combination of fructose and glucose, and/or the kinetics of the fructose (i.e., the speed with which the fructose requires hepatic attention when not accompanied by fiber) is a matter of debate and speculation, but those in this camp do agree that sugar is not “just” an empty calorie. The toxicity of sugar, they argue, is primarily related to its hepatic metabolism. Specifically, “excess” (see below) ingestion of fructose increases VLDL production which increases apoB or LDL-P due to greater triglyceride load. Additionally, at least at reasonable doses according to most literature, insulin resistance is worsened which amplifies the harm caused by other foods.
- Even among those who don’t subscribe to the idea that sugar is metabolically unique (and harmful), with or without a dose-effect, some argue that fructose consumption impacts subsequent food consumption in a way that glucose does not. In other words, eating sugar may fail to satiate you and/or make you subsequently hungrier. These data are sometimes confounded, as are many data in this area, by the use of pure fructose, rather than the glucose-fructose mixture found in sugar. Furthermore, evidence is emerging that sugar is addictive, much in the same way that a drug like heroin or cocaine might be, as suggested by functional MRI. So, while folks in this camp argue that sugar per se isn’t harmful, it does make you eat more (sugar and non-sugar, alike), and that is the harm.
- Perhaps the largest debate in this area stems from the dose issue. The PRO sugar folks argue that at the doses most Americans consume sugar, there is no harm (even if there is a theoretical harm at very high doses). The ANTI sugar folks argue that there is a dose-dependent (and probably a context-dependent – e.g., the insulin resistant person vs. the insulin sensitive person) deleterious impact of sugar, AND that current consumptive patients are indeed in this zone of toxicity. (This is probably the most comprehensive single review I’ve read on the entire topic, and I’ve discussed it point-by-point with 2 of the 3 authors.)
- Speaking of the dose issue, no area of this debate (in my opinion) has generated so much controversy. How much sugar, defined as added sweetener (so this does not include the fructose found in fruit, for example) do Americans actually consume? This is important, of course, if we want to know how applicable the above studies are to the question at hand. Where to begin? (This topic alone is really a 3-part blog post.) Estimating how much added sweeteners Americans consume is primarily done via two methods:
- Taking the difference between food availability data and waste data (ERS); or
- Using nutritional surveys (NHANES).
One of my colleagues, Clarke Read, looked into this recently. Here is what he found (this was in response to a recent NY Times article suggesting sugar consumption is less than typically reported):
The adjustment to loss rates was done by RTI International in this report to the USDA Economic Research Service (ERS). Section 4-1, which is an example calculation, is most useful. RTI was asked to calculate estimates of loss, not estimates of consumption, and rather than working down from availability data, they in fact used NHANES 2003-2004 data to estimate consumption, then basically compared this to availability numbers (with a few adjustments) to find amounts of loss. These loss percentages calculated from 2003-2004 then became the standard, and all other consumption data was calculated by applying this % loss to the availability data.
This means that all consumption numbers are effectively derived from NHANES data. This is especially relevant for added sugars. Since NHANES data tracks only consumption of foods, not ingredients, this availability-versus-consumption comparison initially leads to a 96% loss of cane and beet sugar (seen on page 95 of the 2011 USDA document — the “4 percent” referred to in the NY Times article), since NHANES data only reflects sugar added to foods directly, rather than used as an ingredient. The judgment of a panel of experts was then used to determine the percentage of available sugar used as an ingredient, which led to their 34% loss estimate for sugars. For HFCS, which is never consumed as a food and always as an ingredient, they simply gave it the same value as honey (15% loss between availability and consumption). The ERS, however, overruled them (as described in the NY Times article — see the end of the Losses at Consumer Level section in the link for ERS evidence) and used the 34% loss estimate instead.
Page 10 of the 2011 USDA document shows who these 6 experts are. The NY Times article asked 2 of these 6 about these sugar estimates, who don’t recall making them, though it’s implied that they simply don’t remember what happened back in 2008. In other words, while the overall trend in sugar data is determined by availability data (since % loss is assumed to be constant over time), the absolute amount consumed on any given year, as estimated by these loss-adjusted numbers, is entirely dependent on this RTI loss estimate which, for added sugars, is almost entirely dependent on an expert’s estimation. All foods that are primarily consumed as foods rather than as ingredients have consumption levels that are based on an extrapolation of 2003-2004 NHANES data.
Translation: this is a complete cluster. If you triangulate between the ERS and NHANES data, you wind up with an estimate of about 90 pounds of added sweetener per person, per year, or about 110 gm per day which, on average, works out to about 15% of total caloric intake. Of course the actual consumption is much more nuanced (what isn’t?), since consumption varies a lot by age, gender, and socioeconomic status. Furthermore, this estimate doesn’t include the fructose in fruit juice or fruit, though the latter probably isn’t nearly as high, or relevant, as the former.
Another very interesting point uncovered by colleague, Clarke, was that in a 2009 paper in The Journal of Nutrition, Dr. James Rippe (one of the leading proponents of sugar) noted the following:
“…fructose, as a component of the vast majority of caloric sweeteners, is seen to be particularly insidious.”
“It has also been shown to increase uric acid levels, which in turn promotes many of the abnormalities seen in the metabolic syndrome including hypertriglyceridemia.”
“There is considerable evidence of a detrimental effect on metabolic health of excess fructose consumption.”
Whether by accidental omission or otherwise, this paper is not listed on Dr. Rippe’s CV on his website.
**Sadly, it’s difficult to really interpret the data objectively from those in the PRO sugar camp because of the conflicts of interest. Most of the PRO sugar scientists are heavily funded by the sugar industry. For those interested in the historical context on science and the sugar industry, you’ll find this article particularly interesting.
Take home messages
What I find frustrating about this debate is that most people yelling and screaming don’t fully define the terms, perhaps because they don’t appreciate them (forgivable) or because they are trying to mislead others (unforgiveable). The wrong question is being asked. “Is sugar toxic?” is a silly question. Why? Because it lacks context. Is water toxic? Is oxygen toxic? These are equally silly questions, I hope you’ll appreciate. Both oxygen and water are essential for life (sugar, by the way, is not). But both oxygen and water are toxic – yes, lethal – at high enough doses.
What did the APAP example teach us? For starters, don’t confuse acute toxicity with chronic toxicity. Let’s posit that no one has died from acute toxicity due to massive sugar ingestion. But, what about chronic toxicity? Can eating a lot of sugar, over a long enough period of time, kill you (presumably, through a metabolic disease like diabetes, Alzheimer’s disease, cancer, or heart disease)?
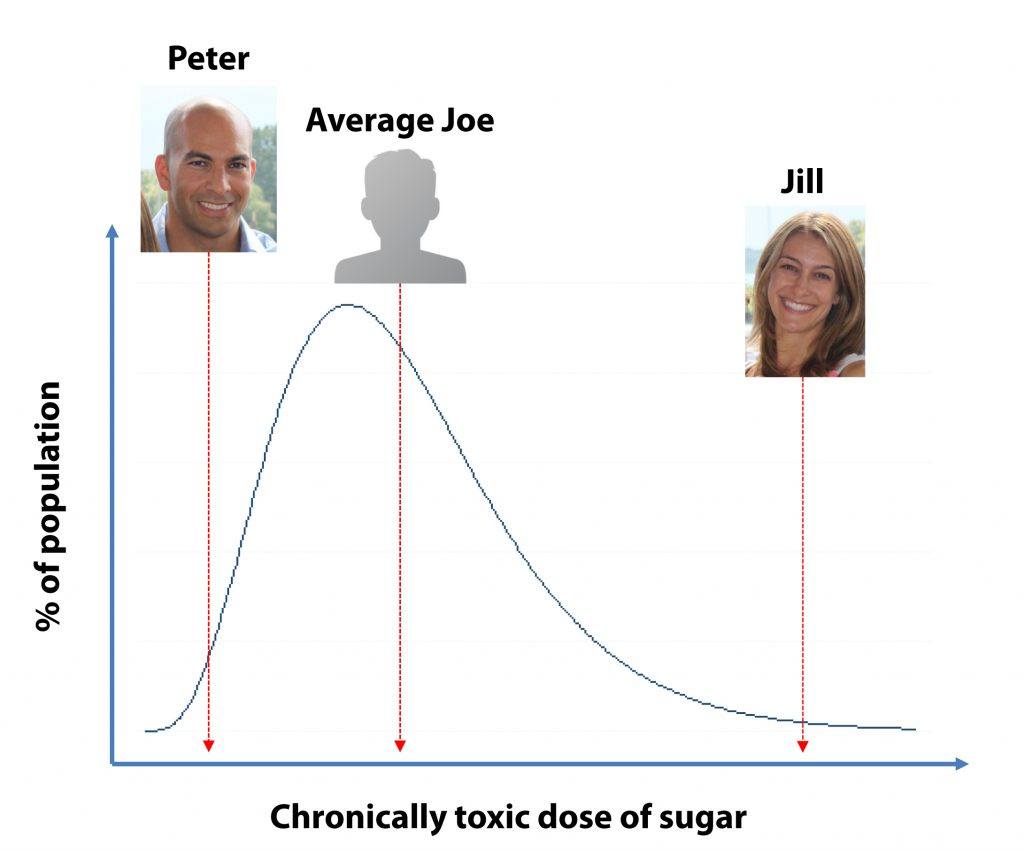
Even among a healthy population (i.e., people without overt liver disease), toxicity is a distribution function. What’s toxic to one person may not be toxic to the next. This is true of APAP and it’s true of sugar. It’s true of most things I can think of, actually, including tobacco, alcohol, cocaine, and heroin. Ever wonder why “only” about one in six smokers dies of small cell lung cancer? Maybe it’s the same reason some people (e.g., me) get metabolically deranged from even modest doses of sugar, while others (e.g., Jill, my wife) can mainline the stuff and not appear to suffer many adverse effects.
I posit that Jill and I are both outliers on the distribution of susceptibility, probably driven mostly by genetic difference (rather than, say, exercise as we both exercise a lot). So, I offer you a framework to consider this question. I know some of you just want an answer to the question, Is sugar toxic or not? But I hope this slightly more nuanced response can help you figure out what you should be asking: Are you like me? Like Jill? Or like an Average Joe somewhere in between us?
This is what you will need to figure out on your own. You could play it safe, assume you’re like me and eliminate all sugar from your diet (I eat no more than about 5 gm of sugar per day, almost exclusively in 85%+ dark chocolate – so less than 4 pounds per year). But if you have Jill’s genes, maybe this is overkill. (Though, I would argue, and may do so in a later post, that even Jill has noticed a change in her energy levels and a number of biomarkers by reducing her sugar content somewhat over the past 3 years.)
It’s pretty easy (conceptually) to figure out where you are on this spectrum, but it does involve a few deliberate steps:
- Without making any adjustment in your current eating habits (i.e., fight like hell to avoid the Hawthorne effect), record everything you eat for a week and, using a database like this one (or something fancier like Nutritionist Pro), calculate exactly how much sugar you consume.
- Collect blood work (paying special attention to lipoproteins, triglycerides, glucose, and insulin among other things) and other measurements (e.g., DEXA if you want to assess body composition, waist measurement).
- Get intimately familiar with all the places sugar shows up that may seem counter-intuitive (e.g., “healthy” cereals, sauces, salad dressings, bread). To do this experiment, you need not restrict your complex carbohydrate intake, but you’ll have to substitute products without added sugar. For example, before I was in ketosis but beginning to discover my own susceptibility to sugar, I had to make my own spaghetti sauce from scratch rather than pour it out of jar. I had to make steel cut oatmeal rather than eat Quaker oats. I had to buy bread made with zero sugar (at $7 a loaf!) rather than my usual “whole wheat” bread. You get the idea. It takes time, and you should expect to spend a few extra dollars on food. But, it’s actually possible to find foods that contain minimal to zero added sugar.
- With this information in hand, begin the intervention: aim for a reduction of at least 50% from step #1. (In my first experiment I did 6 days per week of zero sugar, and one day of all I wanted. Ultimately, this became too difficult, and it actually became easier to just go zero every single day.)
- Repeat the measurements (i.e., step #2) after about three months. If you’ve seen minimal effect, assuming you were methodical and consistent, you’re probably in the Jill camp. If you’ve lost fat, seen a reduction in your triglycerides, fasting glucose and insulin levels, increased your HDL-C, and decreased your apoB or LDL-P (assuming you were able to measure them), you’re probably in the Peter camp.
Last point I’ll make, as I suspect at least some of you are wondering. How do two genetic outliers treat their genetic hybrid (i.e., our daughter)? I’ve written about this previously. In short, we limit the sugar she eats in our house, but not so much outside of the house (e.g., birthday parties). I estimate she eats about 25% of the sugar a “normal” kid does. There is no doubt she loves it, and even a week ago when we went on a daddy-daughter date, I got her ice cream with sprinkles for dessert (the irony of me carrying a bowl of sprinkle- and Oreo-covered ice cream through a crowded restaurant was not lost on me).
What does amaze me is how it seems to override her senses. That night, she had a big plate of salad, a bowl of soup, and even a large slice of pizza (if you’re wondering, I had 3 large plates of salad with chicken). She claimed to be absolutely full, and I believed it. But when I brought that ice cream out, it was like she had never seen food in her life. She simply devoured it. The best part? When she looked like she was done, I said, “OK sweetie, looks like you’re done, time to get going…” only to have her say, “No daddy! I’m still finishing the chocolate broth!” She literally left not one drop of melted ice cream (“chocolate broth”) or one single sprinkle or one single crumb of Oreo behind.
This does not seem “normal” to me, and for this reason I guess I refuse to accept, personally, that sugar is just a benign empty calorie. But, one day our daughter will have to decide for herself where she lies on the distribution and how much she cares to do anything about it. Until then, we’ll save the chocolate broth for special (and not too common) treats.
So, in response to the question, “Is sugar toxic?” it seems to me the answer is, “yes, sugar is probably chronically toxic to many people.” And so is water. And so is oxygen. My sincere hope, however, is that you now understand that this is probably the wrong question to be asking. The better question is probably “What dose of sugar can I (or my child) safely tolerate to avoid chronic toxicity?” The goal should be to figure out your toxic dose, then stay well below it. (It’s probably not wise to consume 95% of the toxic dose of APAP just because you have a really bad headache.) What makes this important, of course, is that with water and oxygen, the toxic doses are so far out of the range of what we normally consume, it’s not really necessary to expend much mental energy worrying about the toxicity. But with sugar, at least for many of us, the toxic dose is easy to consume, especially in world where sugar resides in almost everything we eat.
Photo by Joanna Kosinska on Unsplash





Peter,
I have been fascinated by your blog for quite some time and frequently send links to friends when they tell me what I am doing is wrong. I have been eating a low carb diet for quite some time but never felt great with it until I read some of your advice and really upped my electrolytes and fat intake. With that said I CAN NOT SLEEP lol, I find that I have nearly unlimited energy at all times. I have tried cutting out coffee but that has not helped. I take 3mg of melatonin every night to help me get to sleep, as I have had trouble falling asleep in the past but the melatonin has never failed me before. This has been going on for about a week. Any advice? Thanks in advance.
Phil, I have heard this from several folks. I wish I could say I knew why, but I don’t. In addition, I’ve heard some folks (this happened to me, too) complain of transient vivid dreams. It is possible that your brain is “adjusting” to the new substrate of B-OHB (in addition to glucose).
Sounds like you’re doing the right stuff re: sleep hygiene, but I suspect it takes a while. Full sleep regimen would be: no caffeine or alcohol after, say, 2 pm. No exercise late in the day. Stop desk work after dinner, etc. Hopefully this effect is transient.
Phil,
Could you say exactly what you’ve been eating to up the electrolytes and fat? I’m just wondering because I feel quite fatigued on the low-carb diet (and I keep trying but eventually give up and later try again), although I do try to have broth every day and lots of fat. I thought if I try exactly what you did maybe I could get all that energy, too! But I hope you start sleeping well soon–good luck!
This may be from the ketogenic effects on adenosine (it can kick the switch caffeine too inhibits). I don’t know the counters off-hand, whether it’s transient or just a sign ketogenic diet is not for you (sleep is kinda important-sarcasm alert). What came to mind as natural forms (there’d be pharmacological ones too) would be valerian and/or hops, however, there is no medical literature on the interaction of these two pulls on adenosine, so I would use caution and a fantastic doctor. There may be other strategies if investigated, or again there may be subtypes or times when/where ketosis is not a well suited strategy, in my understanding.
Adenosine, Ketogenic Diet and Epilepsy: The Emerging Therapeutic Relationship Between Metabolism and Brain Activity. S.A Masino, M Kawamura, Jr, C.D. Wasser, L.T Pomeroy and D.N Ruskin. Curr Neuropharmacol. 2009 September; 7(3): 257–268. doi: 10.2174/157015909789152164
The fixed combination of valerian and hops (Ze91019) acts via a central adenosine mechanism. Schellenberg R, Sauer S, Abourashed EA, Koetter U, Brattström A. Planta Med. 2004 Jul;70(7):594-7.
Peter, extremely brilliant posting. Thank you for your comments. Your distinction between acute and chronic toxicity is very important.
I stopped measuring my lipids quite some time ago, because they had all reverted to normal after carbohydrate reduction. The thing I track now is my weight and waistline. I would also like to say that it is possible to be carbohydrate-reduced on a strict vegan diet, whether for ethical or health reasons. No need to throw out the baby with the bathwater there! The only sugar I consume is from vegetables or very small amounts of fruit. As with you, I am highly sensitive to (dys)metabolic syndrome.
I have had some success with coaching patients to cut down on their sugar and starch intake, with impressive reductions in body weight, plaque burden (though a few deteriorated), and lipid measures. I believe you use LDL-P. We don’t have much access to that here in Canada, although I understand Atherotech has recently added it to their battery of tests.
I would appreciate hearing what you think, in a nutshell, about fruit consumption. Or is that somewhere else on this site?
Many thanks,
Dan Hackam
Low GI fruit are fine for all, and most fruit (incl high GI like banana) for some. Even in ketosis one can consume a modest amount of berries.
Hi Peter
Your site is great.
My question is: Do you know or know of any research in regards to how carbs impact hyroid hormone (T4/T3) production within the body.
I’m an Endurance guy, Triathlon. My Thryroid was removed in 2005 due to Thyroid cancer and I take synthetic T4. My perception is that carbs somehow influence T4 conversio to T3 but have not been able to find any research.
If I reduce my carbs it seems I need more T4. So I am trying to figure out the science to validate what I experience. Thanks……..Mike
I suspect it’s not about carbs influencing conversion of T4 to T3 and perhaps more to do with ATP sensing in the liver and those changes driving TSH, which in turn drive T3 and T4.
I was thinking of your blog as I read this disaster https://www.huffingtonpost.ca/jane-dummer/sugar-myths_b_3417321.html and this nice little bit of information at the bottom
“Jane Dummer is a registered dietitian and expert in nutrition. Jane serves as a consultant to the food and beverage industry, including The Coca-Cola Company.”
Last week I took my boys to a movie and was subjected to a 2 minute Coca-Cola propaganda piece that dovetails nicely with the message in this article.
Funny. But not funny, too.
Yes, it is one of those head scratchers where you are not sure whether to laugh, cry or get angry.
Peter, this is not directly about your post, but have you noticed that the “Recent Comments” list has started to have links to apparently unrelated posts on other web sites, that definitely are not comments, and that do not reference your blog?
This morning I am seeing an entry in your comment list for https://excellentjourney.net/2013/06/15/primal-summer/ and another for https://healthylivinghowto.com/1/post/2013/06/why-the-body-needs-saturated-fat.html
These actually look like interesting reads, but they’re not comments and they’re not on your site. Looks like a peculiar bug in your blog software. I first saw this a few days ago and assumed you would fix it, but maybe you haven’t seen it on your end (?). Hope this will help (and I hope I’m not the only one getting this!)
Bob.
I think these are links from other sites to this one. The 3 I looked at are not spam and do make an actual reference. I’ll keep an eye out.
Those are called “trackbacks”. Others linking back to your site, usually a good thing.
https://en.wikipedia.org/wiki/Trackback
Yes. I get about 10 a day, however they usually don’t show up as comments. Maybe they have all along and I’ve just missed it.
What a relief to find this blog and the topics you are discussing. Granted, there will always be parts that are over my head, but it is very thought provoking.
I’ve been involved in various types of self-experimentation for many years, not necessarily by conscious choice.
I do want to add one point to what you say about finding alternatives to foods with added sugars. Yes, it is possible. Be prepared, though, in our culture of many choices, to discover that many, if not most products wind up being off your radar. You wind up being surrounded by people puzzling over what foods to choose in a supermarket or restaurant while you are scanning around for what (or whether) there is anything there you CAN eat.
Granted, in my case, I have sensitivities to MSG and for some bizarre reason, to citric acid, which is a common preservative, which basically means that if I want to eat it, I need to prepare it myself, and NO, I do not always have the energy to do this!
In any case, I am so happy to have found this place where this discussion is happening and to following along as new information comes along.
In the end, each of us needs to get to know their own metabolism and its quirks and since our bodies change throughout our lives, this learning has to continue as well.
I’m tempted to think some of the difference in sugar tolerance between you and your wife comes down to sex-based differences re carb metabolism. I think pre-menopausal women do better with carbs than do men. Indeed, many women of reproductive age cannot healthily sustain a true VLC (or “paleo”) diet.
Probably not in her/my case, though these differences do matter over time.
I’m glad someone is looking into this. Someday there will be recognition that sugar addicts need opportunities for help rather than judgement about the resulting obesity and diabetes. Unfortunately, there is no such official recognition of foods/sugar being addictive “drugs” and there is no such thing as sugar rehab.
Your article/blog post is very interesting to me. Two years ago, I had “perfect” cholesterol levels, great HDL/LDL ratio, but my Dr. noticed my fasting glucose was at 103. (It’s always been around 95-100 anyway) Then 6 months later, labs again, crept up to 109. Dr. said cut carbs and exercise. I weighed 155lbs at 5’8″, not obese. So, I went on the “Atkins diet” for 6 months. I exercised some. I do not RUN. 🙂 I do have to tell you that I did not eat much chicken or fish (not a big fan of either in great amounts) but I cut carbs enormously. 50-75 max a day. I lost 15lbs -20lbs without exercise. Felt FABULOUS. I was 46.
Labs again to see the results at about the 6 month mark, new Dr-other left private practice- fasting glucose had only fallen to 106. I was VERY disappointed. I had cut the sugar out of my diet tremendously. I love sweets! 🙂 But I did it. Diabetes runs on both sides of my family and this is a concern though my mother’s was elevated (but not diagnosed diabetic) up until she died at 79.
So that makes me wonder what camp i am in.
I cut massive amounts of sugar out of my diet and saw little change in my fasting glucose levels.
And the biggest disappointment was that my LDL/HDL went wonky on the Atkins. My good cholesterol went up (it was already good to start out with) but so did the BAD. My triglyceride level DROPPED. It was good before but it had a 30point drop! but now my LDL was over the legal limit! The ratio stayed the same but I received a phone call from the nurse with a call-in for Lipitor.
I unofficially fired my Dr. at that moment.
That Dr. just called in a cholesterol med and never once asked any questions about my diet!! I will get with a new Dr. and hopefully have an intelligent conversation about what’s going on with me and how to avoid having to take cholesterol meds and exactly HOW I need to modify my diet!
ALL MY LIFE I have had fabulous cholesterol levels. GREAT LABS. Except that stinkin’ fasting glucose. And then the elevated cholesterol after following some version of the Adkins Diet!
I’m very confused. I had a “normal diet” and had great HDL/LDL levels, but slightly elevated glucose. Went low carb, now wonky 225 cholesterol and still slightly elevated glucose.
Ugh. Thanks for listening.
The ‘straight dope on cholesterol’ series may be interesting for you to read.
Sorry that comment is so long. Perhaps you can edit it? I’ve had a lot of coffee today. 😉
My wife talked to you about lipids in Boston at the AHS conference last year.
I, a lawyer, was also present. Below is part what I got out of the conference & what it has led to. You will find it interesting:
https://buffalo.ynn.com/content/top_stories/670200/buffalo-lawyer-files-lawsuit-against-makers-of-high-fructose-corn-syrup/
I wanted to put in Jay Wortman’s comments from Richard Feinman’s post on “Fructophobia”.
“What is the downside of making sugar less accessible? You argue that in the current climate of lipophobia, the only place to go then is more starch. Yes, technically true. But in the real world, possibly not. When my 11 year old son leaves our sugar-free home and goes out into a sugar-soaked world, he is not tempted by pizza, rice and potatoes (well, maybe chips), it is the soda, juice, cookies, candies, etc that he is bombarded with that challenge his resolve to eat according to our wishes. If those are gone, will he then over-indulge in pizza, rice and potatoes? I don’t think so. And, even if more starchy things become available, they are usually combined with fats when eaten (eg pizza) which, I believe, mitigates the harms of refined carbs by reducing post-prandial hyperglycemia. If they are not combined with sugar (eg cakes, cookies) what will people eat instead? Excess starch consumption in the absence of sugar would be not that appetizing, methinks.
“It is for these reasons that I think a pogrom against sugar is perhaps not a bad place to start.
“My son at 11 already thinks he’s 14. And he has put us on notice that his first act after emancipation will be to return home and consume a chocolate bar in front of his father. To which I reply, “if you want to damage yourself, why waste your money, why not just hit yourself on the head with a rock? And why wait?”.
My son and I have a great relationship and he has a wicked sense of humour. ”
By the way, the documentary made regarding Jay Wortman’s Big Fat Diet in Canada is worth watching.
Refined sugar, I think is toxic regardless of whether you are a Jill or a Peter. Whole foods, preferably raised without antibiotics, pesticides, or GMO’s. We don’t need it. We can get plenty of natural sugar from fruits in our diet in moderation. I come from an alcoholic background that goes back three generations. I remember when my Father quit all alcohol that he suddenly started sucking in anything with sugar in it. I.E. cakes, ice cream etc. Well, he was just replacing his alcohol with pure sugar. Growing up I was a Jill.
I sucked in deserts but I had a very high metabolism and was very active. I stayed slim. Fast forward to age 45 to 50. Slowly eating anything I wanted was no longer working. And I started to gain weight eating the same way I had always eaten. So, I started trying every kind of diet. Atkins, no carbs, raw foods. The hardest thing to eliminate were salty chips, and fresh bread. I easily gave up the sweet desserts. I could bake a loaf of bread and consume the entire loaf. Of course bread is starch is sugar. Same Same Same. Fast forward to age 60. Suddenly a cancer crops up on tonsillectomy scar tissue. After seven weeks of horrid radiation (it was stage one) And refusing all tube feeding. I then weighed 104 pounds. Having started at 150 pounds (before treatment) and I am 5 feet 6 inches tall. I refused tube feeding because I knew that if I accepted it, then I would not continue to eat food by mouth and eventually I would have to wean off the tube feeding plus I saw the infections that could result from leaning on tube feeding. So began my battle to gain back to a healthy weight. I found that now sugary foods held no joy. I had lost the ability to taste sweet. The best foods were pure, simple foods. Like fresh tomato (which I was advised not to eat but I have anyway, in fact craved them) I also could not now eat the salty dry foods because of lack of saliva. So, in fact, it took supplementing with protein Carnation to gain to 120 pounds. I imagine I was in ketosis without even trying since I had to eliminate all breads, and sweets. The best foods when you have no saliva are juicy fresh foods. Ie berries, avocado, peaches, tomato, etc. Meats were also difficult. A group of octogenarians who are on the CR slowing aging plan helped me to understand why I could not gain weight. Here is what they told me. Also this very low calorie diet is very good at reducing re-occurence of cancer cells. Cancer loves sugar in any form. This was a life saving email for me. I cannot thank the CR group enough. Also know that they thyroid can have great influence on cholesterol. Too little thyroid hormone and cholesterol will go up, as will weight gain. For me, I think sugar is poison. We don’t really need refined sugar. Be careful what you wish for. Life is strange.
Hello Candy,
My wife and I are on CR 8+ years now. She is 5’6″ and weighs 120, age 60.
Wound healing is very slow when on a CR diet.
You can add protein via protein powders added to smoothies. Whey and rice protein powders are frequently mentioned by our members. Be sure to do weight bearing type exercise so you add muscle instead of body fat.
CR will inhibit the return of cancer based on lab animal evidence. Be sure to use diet tracking software to assure all essential nutrition. Those vitamins, minerals, and amino acids are what your body uses for maintenance and repair.
You are finding it hard to gain weight because your body has established a new set point and will defend that set point. Continue eating additional calories from all sources and your body will finally accept that it cannot keep burning off the excess calories to defend the set point. It is similar to people reaching a plateau when losing weight. There are plateaus during weight gain as well.
Alternative medicine is a sound approach to health maintenance, but modern medicine is where you want to look when you become ill. The best preventative approach is a diet high in vegetables and fruit. Restrict saturated fat and use olive oil as a healthy source of fat as well as fish and fish oil capsules. Regular exercise is also wise for age related disease prevention.
Good luck and email again if you have further questions.
Bob Cavanaugh
Managing Director
CR Society Intl.
I found this fascinating. Here in the UK the BBC ran a series a short while ago called ‘The Men Who Made Us Fat’, which closely mirrors what is being suggested in this blog. A precis can be found here: https://www.bbc.co.uk/news/health-18393391
I went through the menopause at 32, then almost doubled my weight in a couple of years. I was thoroughly beaten down by docs saying ‘eat less, exercise more’. I have kept a food diary for the last six years and rarely go over 1800 calories & 50g of fat, walk continuously at work and do 30mins a day exercise. Still I’m seen as just a fat woman who’s lying to herself.
I’m going to follow your suggestions and see if this helps. It does make sense!
I’ve seen parts of it, Teresa. Very interesting.
maybe all the ideas are correct?
in the early 2000s i worked for an integrative medicine clinic. serving a primary population of cancer patients. they manipulated chemo to minimize the effects with heavier dosing at night, gave high dose iv vitamins, herbal supplements, psychotherapy, biofeedback, body therapies like massage. and of course diet. every patient was told they were getting an individual program but the diet was almost the same for everyone. a modified macrobiotic diet. no sugar, very minimal eggs, minimal to no dairy, cold water fish, lots of vegetables, beans, tofu tempe seitan. one of the personalizing factors was if a patient had an estrogen receptor positive tumor they were steered away from soy.
i believed in the clinic and the diet & brought the diet home. no sugar (yes brown rice syrup, barley malt and agave). from few eggs to no eggs, from occasional dairy to no dairy and then no fish.
i got sick. always freezing in the summer – from my bones. losing weight. constant fatigue unable to exercise, molluscum. my cbc bmp thyroid all normal. one of the clinic dietician / researchers deviated from the party line and told me my genetic background was not allowing me to follow this vegan diet, the best thing i could do was return to my omnivore roots or at least eat some chicken soup from time to time. i did and the molluscum went away i could run daily and lift weights. At the time i could not leave a meal feeling full without bread or pasta. recently life has changed, over a decade has passed i started putting on weight. now i feel best with bread once a week, mostly vegetables, meat – high fat – which has had multiple positive effects.
is it user specific and time specific too? maybe all the researchers are correct – for some people some time – no fat or no sugar… could it be that the optimal diet based on stress, environmental exposures, sleep availability, physical demands and genetics at age 30 may not be appropriate for the different environment, other demands and the same genetics at age 50.
Peter, I arrived here through your ted talk. It was quite compelling, and I impressed very much by what you shared there. I strive to grow that much in my own life.
On sugar: I am relatively sure that I react poorly to sugar as well, when I went cold turkey I went from about 220 to about 200 in a few months (I am 6 1 and am fairly dense). I started doing crossfit and loosened up my diet a little (partially due to added calorie burn from the intense cardio) and my weight has shot back up to the 220 range.
My trouble is that I actually have a reasonably hard time figuring out what is/isn’t on the “converts to sugar” list. Rice is bad, bread is bad? I guess? I can safely assume Ice Cream/Candy are bad, but that “Not obviously sugar” list is harder for me to find in a way that I can easily remember. According to some people it seems like nearly everything converts to some form of sugar, and I should be eating close to paleo if not actual paleo. Can you recommend a resource for finding an easy to understand list?
Thanks!
I think you may be confusing 2 ideas… when I say sugar I really mean sucrose and HFCS. Rice, etc. gets converted to glucose, which is not the same. The speed with which a carbohydrate gets converted to glucose is loosely proxied by its glycemic index (GI).
Thanks for the reply!
I guess the clarification to my question is that I don’t know what words I should be triggering on avoiding. I know sugar in all it’s various forms (Cane, evaporated cane juice, HFCS certainly, etc etc). What I don’t know is what else is on the list, I guess I sort of thought that all bread was inherently sugar, maybe that isn’t true. You are telling me Rice isn’t on your list of foods to avoid? Or it is?
That sort of starts to get at the fact that I don’t know how to look at a food label and tell if it’s carbs are simple or complex, (Unless they are specifically labeled simple). Maybe that’s just internet research for me to do. I looked around your site and didn’t find anything like a discrete list.
Thanks!
Hi Peter,
I have found your post very interesting and educational to read. Recently I have been diagnosed with IBS and we have been trying to work out triggers and also if it could be food and my doctor had recommended the LowFODMAP diet. Information about the diet from Monash Uni – https://www.med.monash.edu/cecs/gastro/fodmap/.
As part of the diet you cut out Fructose and Sugar Polyols to see if these can cause issues. I have found that this isn’t the only issue – the next step is a low carb diet, because we have seen a trend in carb heavy foods causing issues even within the limitations of the Low FODMAP diet.
I also have been reading information from Sweet poison (https://sweetpoison.com.au/) which I thought you might find interesting.
Thanks for an interesting post and I am off to read some more of them.
Belle
limiting intake of this addictive substance makes so much sense. In regards to children, is it possible their bodies metabolize sugar differently so that its effects are less harmful until they are full-grown – (mother’s milk is high in sugar)
Hi Peter,
Sorry if this comment doesn’t quite go along with the topic of the post, but my brain says it does, sort of.
My husband and I started a low carb (<20g) diet over a month ago. We both lost 10 or so pounds of water in the first two weeks. He has continued to lose weight, about 1 pound a week. My weight has been another story. Starting the low carb diet seemed to expose another condition in me. It all started when we went for a hike on a Saturday two weeks ago. As soon as I started to feel the exertion from the hike, I noticed my hands starting to tingle, like they were losing circulation. Then it began in my feet, legs, and face. The tingling was leading to numbness until I told my husband I had to stop and rest. At this point I had already formed several hypotheses as to the cause and ruled out them all except low BP. To confirm, resting and squatting seemed to help, as well as guzzling water. After I drank about a liter of water, I was able to continue the hike with only minor tingling in my hands (I kept drinking water throughout). Since then, I've been trying to drink at least 80 oz of water everyday (even though I don't "feel" thirsty and often feel like I'm forcing it down) and get adequate electrolytes. However, my body is retaining the water like crazy (up and down 2-6 lbs everyday), but even though I'm urinating like crazy too, I still have symptoms of dehydration (dry lips/skin, lethargy, const., headaches, etc). Doing some research into the matter, it seems that probably I've been chronically dehydrated the majority of my life, but it somehow was always masked and mitigated by the water I retained with my glycogen load. My hope is that if I continue taking in a lot of water, my body's cells will stop acting like I live in a dessert (even though I do) and the retention and symptoms will cease.
All of that to say this: My research led me to the book "Water for Health, for Healing, for Life: Your Not Sick, Your Thirsty!" by F. Batmanghelidj, M.D. In the book, Dr. Batmanghelidj makes claims that almost all of our chronic diseases (asthma, allergies, obesity, diabetes, hypertension etc) are caused by an underlying chronic dehydration and that 75% of Americans are dehydrated. These claims are based on his clinical and personal experiences (healing peptic ulcers by having patients drink water etc) and his own research, but he rarely cites scientific literature in the book. So, while the concepts are compelling, they might should also be taken with a grain (or pinch?) of salt.
Here is where my brain connected with the posted topic: One of the claims he makes is that in the case of diabetes, dehydration and subsequent low sodium/potassium levels cause the brain to "peg up the glucose threshold so that it can maintain its own volume and energy requirements." This would explain why "stressed people resort to eating sweet food." Se essentially, people crave sweet food because they are dehydrated.
But here is my real reason for posting: He also says that when water, sodium, and potassium levels are low, "the responsibility for holding water in the body and outside the cells falls onto the sugar content in the blood" and that insulin is a water regulator because it forces potassium into cells. He doesn't ever really touch on a dehydration-cause of insulin resistance. In fact, he claims that dehydration causes insulin to not be secreted, which causes diabetes. However, we know that in most individuals who end up getting diabetes, there is a hyper secretion of insulin and resistance to it before the pancreas gives out. However, assuming the above quotes are true, what if dehydration IS the root cause of insulin resistance? The logic would be as follows: the volume of water in the body is lower than optimal as well as sodium and potassium levels. The individual is eating excessive sugar because she is misinterpreting thirst signals. The pancreas pumps out insulin because the glucose load is too high. The cells, however, reject the glucose that the insulin is trying to usher in because they "sense" the body's dehydration level and are rejecting it in order to maintain adequate blood volume in the circulation.
Do you have any insight in regards to this or chronic dehydration?