Want to catch up with other articles from this series?
- The straight dope on cholesterol – Part I
- The straight dope on cholesterol – Part II
- The straight dope on cholesterol – Part III
- The straight dope on cholesterol – Part IV
- The straight dope on cholesterol – Part V
- The straight dope on cholesterol – Part VI
- The straight dope on cholesterol – Part VII
- The straight dope on cholesterol – Part VIII
- The straight dope on cholesterol – Part IX
Previously, across 8 parts of this series we’ve laid the groundwork to ask perhaps the most important question of all:
What should you eat to have the greatest chance of delaying the arrival of cardiovascular disease?
Before we get there, since this series has been longer and more detailed than any of us may have wanted, it is probably worth reviewing the summary points from the previous posts in this series (or you can just skip this and jump to the meat of this post).
What we’ve learned so far
- Cholesterol is “just” another fancy organic molecule in our body but with an interesting distinction: we eat it, we make it, we store it, and we excrete it – all in different amounts.
- The pool of cholesterol in our body is essential for life. No cholesterol = no life.
- Cholesterol exists in 2 forms – unesterified or “free” (UC) and esterified (CE) – and the form determines if we can absorb it or not, or store it or not (among other things).
- Much of the cholesterol we eat is in the form of CE. It is not absorbed and is excreted by our gut (i.e., leaves our body in stool). The reason this occurs is that CE not only has to be de-esterified, but it competes for absorption with the vastly larger amounts of UC supplied by the biliary route.
- Re-absorption of the cholesterol we synthesize in our body (i.e., endogenous produced cholesterol) is the dominant source of the cholesterol in our body. That is, most of the cholesterol in our body was made by our body.
- The process of regulating cholesterol is very complex and multifaceted with multiple layers of control. I’ve only touched on the absorption side, but the synthesis side is also complex and highly regulated. You will discover that synthesis and absorption are very interrelated.
- Eating cholesterol has very little impact on the cholesterol levels in your body. This is a fact, not my opinion. Anyone who tells you different is, at best, ignorant of this topic. At worst, they are a deliberate charlatan. Years ago the Canadian Guidelines removed the limitation of dietary cholesterol. The rest of the world, especially the United States, needs to catch up. To see an important reference on this topic, please look here.
- Cholesterol and triglycerides are not soluble in plasma (i.e., they can’t dissolve in water) and are therefore said to be hydrophobic.
- To be carried anywhere in our body, say from your liver to your coronary artery, they need to be carried by a special protein-wrapped transport vessel called a lipoprotein.
- As these “ships” called lipoproteins leave the liver they undergo a process of maturation where they shed much of their triglyceride “cargo” in the form of free fatty acid, and doing so makes them smaller and richer in cholesterol.
- Special proteins, apoproteins, play an important role in moving lipoproteins around the body and facilitating their interactions with other cells. The most important of these are the apoB class, residing on VLDL, IDL, and LDL particles, and the apoA-I class, residing for the most part on the HDL particles.
- Cholesterol transport in plasma occurs in both directions, from the liver and small intestine towards the periphery and back to the liver and small intestine (the “gut”).
- The major function of the apoB-containing particles is to traffic energy (triglycerides) to muscles and phospholipids to all cells. Their cholesterol is trafficked back to the liver. The apoA-I containing particles traffic cholesterol to steroidogenic tissues, adipocytes (a storage organ for cholesterol ester) and ultimately back to the liver, gut, or steroidogenic tissue.
- All lipoproteins are part of the human lipid transportation system and work harmoniously together to efficiently traffic lipids. As you are probably starting to appreciate, the trafficking pattern is highly complex and the lipoproteins constantly exchange their core and surface lipids.
- The measurement of cholesterol has undergone a dramatic evolution over the past 70 years with technology at the heart of the advance.
- Currently, most people in the United States (and the world for that matter) undergo a “standard” lipid panel, which only directly measures TC, TG, and HDL-C. LDL-C is measured or most often estimated.
- More advanced cholesterol measuring tests do exist to directly measure LDL-C (though none are standardized), along with the cholesterol content of other lipoproteins (e.g., VLDL, IDL) or lipoprotein subparticles.
- The most frequently used and guideline-recommended test that can count the number of LDL particles is either apolipoprotein B or LDL-P NMR, which is part of the NMR LipoProfile. NMR can also measure the size of LDL and other lipoprotein particles, which is valuable for predicting insulin resistance in drug naïve patients, before changes are noted in glucose or insulin levels.
- The progression from a completely normal artery to a “clogged” or atherosclerotic one follows a very clear path: an apoB containing particle gets past the endothelial layer into the subendothelial space, the particle and its cholesterol content is retained, immune cells arrive, an inflammatory response ensues “fixing” the apoB containing particles in place AND making more space for more of them.
- While inflammation plays a key role in this process, it’s the penetration of the endothelium and retention within the endothelium that drive the process.
- The most common apoB containing lipoprotein in this process is certainly the LDL particle. However, Lp(a) and apoB containing lipoproteins play a role also, especially in the insulin resistant person.
- If you want to stop atherosclerosis, you must lower the LDL particle number. Period.
- At first glance it would seem that patients with smaller LDL particles are at greater risk for atherosclerosis than patients with large LDL particles, all things equal.
- “A particle is a particle is a particle.” If you don’t know the number, you don’t know the risk.
- With respect to laboratory medicine, two markers that have a high correlation with a given outcome are concordant – they equally predict the same outcome. However, when the two tests do not correlate with each other they are said to be discordant.
- LDL-P (or apoB) is the best predictor of adverse cardiac events, which has been documented repeatedly in every major cardiovascular risk study.
- LDL-C is only a good predictor of adverse cardiac events when it is concordant with LDL-P; otherwise it is a poor predictor of risk.
- There is no way of determining which individual patient may have discordant LDL-C and LDL-P without measuring both markers.
- Discordance between LDL-C and LDL-P is even greater in populations with metabolic syndrome, including patients with diabetes. Given the ubiquity of these conditions in the U.S. population, and the special risk such patients carry for cardiovascular disease, it is difficult to justify use of LDL-C, HDL-C, and TG alone for risk stratification in all but the most select patients.
- To address this question, however, one must look at changes in cardiovascular events or direct markers of atherosclerosis (e.g., IMT) while holding LDL-P constant and then again holding LDL size constant. Only when you do this can you see that the relationship between size and event vanishes. The only thing that matters is the number of LDL particles – large, small, or mixed.
- HDL-C and HDL-P are not measuring the same thing, just as LDL-C and LDL-P are not.
- Secondary to the total HDL-P, all things equal it seems smaller HDL particles are more protective than large ones.
- As HDL-C levels rise, most often it is driven by a disproportionate rise in HDL size, not HDL-P.
- In the trials which were designed to prove that a drug that raised HDL-C would provide a reduction in cardiovascular events, no benefit occurred: estrogen studies (HERS, WHI), fibrate studies (FIELD, ACCORD), niacin studies, and CETP inhibition studies (dalcetrapib and torcetrapib). But, this says nothing of what happens when you raise HDL-P.
- Don’t believe the hype: HDL is important, and more HDL particles are better than few. But, raising HDL-C with a drug isn’t going to fix the problem. Making this even more complex is that HDL functionality is likely as important, or even more important, than HDL-P, but no such tests exist to “measure” this.
Did you say “delay?”
That’s right. The question posed above did not ask how one could “prevent” or eliminate the risk cardiovascular disease, it asked how one could “delay” it. There is a difference. To appreciate this distinction, it’s worth reading this recent publication by Allan Sniderman and colleagues. Allan sent me a copy of this paper ahead of publication a few months ago in response to a question I had posed to him over lunch one day. I asked,
“Allan, who has a greater 5-year risk for cardiovascular disease, a 25 year-old with a LDL-P/apoB in the 99th percentile or a 75-year-old with a LDL-P/apoB in the 5th percentile?”
The paper Allan wrote is noteworthy for at least 2 reasons:
- It’s an excellent reminder that age is a paramount risk factor for cardiovascular disease.
- It provides a much better (causal) model for atherosclerosis than the typical age-driven models, and explains why age is an important risk factor.
What do I mean by this? Most risk calculators (e.g., Framingham) take their inputs (e.g., age, gender, LDL-C, HDL-C, smoking, diabetes, blood pressure) and calculate a 10-year risk score. If you’ve ever played with these models you’ll quickly see that age drives risk more than any other input. But why? Is there something inherently “risky” about being older?
Sniderman and many others would argue (and I agree) that the reason age is a strong predictor of risk has to do with exposure to apoB particles — LDL, Lp(a), and apoB-carrying remnants. Maybe it’s because I’m a math geek, but such models just seem intuitive to me because I think of most things in life in terms of calculus, especially integrals, the “area under a curve.”
[I once tried to explain to a girlfriend who thought I wasn’t spending enough time with her that my interest in her should be thought of in terms of the area under the curve, rather than any single point in time. That is, think in terms of the integral function, not the point-in-time function. Needless to say, she broke up with me on the spot (in the middle of a parking lot!), despite me drawing a very cool picture illustrating the difference, which I’ve re-created, below.]
The reason age is such a big driver of risk is that the longer your artery walls are exposed to the insult of apoB particles, the more likely they are to be damaged, for all the reasons we covered in Part IV of this series. [This paper also reviews the clinical situation of PCSK9 mutations which builds a very compelling case for the causal model of apoB particles in the development of atherosclerosis].
What does eating have to do with cardiovascular risk?
So now that everyone is on the edge of their seat in anticipation of this punch-line, let me provide two important caveats.
First, there are no long-term studies – either in primary or secondary prevention – examining the exact question we all want to know the answer to with respect to the role of dietary intervention on cardiovascular disease. There are short-term studies, some of which I will highlight, which look at proxies for cardiovascular disease, but all of the long-term studies (looking at secondary prevention), are either drug studies or multiple intervention studies (e.g., cholesterol-lowering drug(s) + blood pressure reducing drug(s) + dietary intervention + exercise + …).
In other words, the “dream” study has not been done and won’t be done for a long time. The “dream” study would follow 2 randomized groups for many years and only make one change between the groups. Group 1 would consume a standard American diet and group 2 would consume a very-low carbohydrate diet. Furthermore, compliance within each group would be excellent (many ways to ensure this, but none of them are inexpensive – part of why this has not been done) and the study would be powered to detect “hard outcomes” (e.g., death), instead of just “soft outcomes” (e.g., changes in apoB, LDL-C, LDL-P, TG).
Second, everything we have learned to date on the risk relationship between cardiovascular disease and risk markers is predicated on the assumption that a risk maker of level X in a person on diet A is the same as it would be for a person on diet B.
Since virtually all of the thousands of subjects who have made up the dozens of studies that form the basis for our understanding on this topic were consuming some variant of the “standard American diet” (i.e., high-carb), it is quite possible that what we know about risk stratification is that this population is not entirely fit for extrapolation to a population on a radically different diet (e.g., a very-low carbohydrate diet or a ketogenic diet). Many of you have asked about this, and my comments have always been the same. It is entirely plausible that an elevated level of LDL-P or apoB in someone consuming a high-carb diet portends a greater risk than someone on a ketogenic or low-carb diet. There are many reasons why this might be the case, and there are many folks who have made compelling arguments for this hypothesis.
But we can’t forget the words of Thomas Henry Huxley, who said, “The great tragedy of science is the slaying of a beautiful hypothesis by an ugly fact.” Science is full of beautiful hypothesis slayed by ugly facts. Only time will tell if this hypothesis ends up in that same graveyard, or changes the way we think about lipoproteins and atherosclerosis.
The role of sugar in cardiovascular disease
Let’s start with what we know, then fill in the connections, with the goal of creating an eating strategy for those most interested in delaying the onset of cardiovascular disease.
There are several short-term studies that have carefully examined the impact of sugar, specifically, on cardiovascular risk markers. Let’s examine one of them closely. In 2011 Peter Havel and colleagues published a study titled Consumption of fructose and HFCS increases postprandial triglycerides, LDL-C, and apoB in young men and women. If you don’t have access to this journal, you can read the study here in pre-publication form. This was a randomized trial with 3 parallel arms (no cross-over). The 3 groups consumed an isocaloric diet (to individual baseline characteristics) consisting of 55% carbohydrate, 15% protein, and 30% fat. The difference between the 3 groups was in the form of their carbohydrates.
Group 1: received 25% of their total energy in the form of glucose
Group 2: received 25% of their total energy in the form of fructose
Group 3: received 25% of their total energy in the form of high fructose corn syrup (55% fructose, 45% glucose)
The intervention was relatively short, consisting of both an inpatient and outpatient period, and is described in the methodology section.
Keep in mind, 25% of total energy in the form of sugar is not as extreme as you might think. For a person consuming 2,400 kcal/day this amounts to about 120 pounds/year of sugar, which is slightly below the average consumption of annual sugar in the United States. In that sense, the subjects in Group 3 can be viewed as the “control” for the U.S. population, and Group 1 can be viewed as an intervention group for what happens when you do nothing more in your diet than remove sugar, which was the first dietary intervention I made in 2009.
Despite the short duration of this study and the relatively small number of subjects (16 per group), the differences brought on by the interventions were significant. The figure below shows the changes in serum triglycerides via 3 different ways of measuring them. Figure A shows the difference in 24-hour total levels (i.e., the area under the curve for serial measurements – hey, there’s our integral function again!). Figure B shows late evening (post-prandial) differences. Figure C shows the overall change in fasting triglyceride level from baseline (where sugar intake was limited for 2 weeks and carbohydrate consumption consisted only of complex carbohydrates).
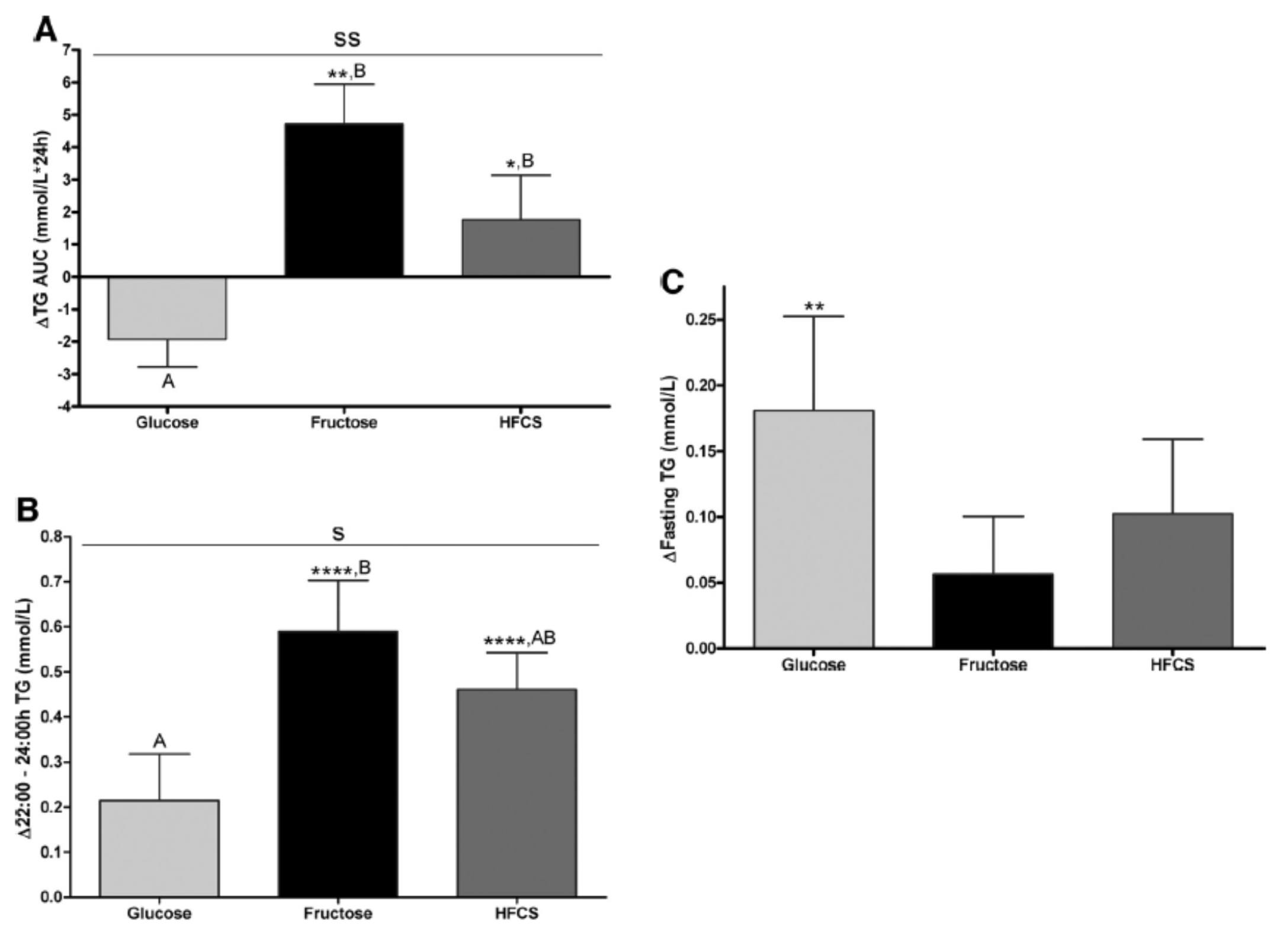
The differences were striking. The group that had all fructose and HFCS removed from their diet, despite still ingesting 55% of their total intake in the form of non-sugar carbohydrates, experienced a decline in total TG (Figure A, which represents the daily integral of plasma TG levels, or AUC). However, that same group experienced the greatest increase in fasting TG levels (Figure C). Post-prandial TG levels were elevated in all groups, but significantly higher in the fructose and HFCS groups (Figure B). The question this begs, of course, is which of these measurements is most predictive of risk?
Historically, fasting levels of TG are used as the basis of risk profiling (Figure C), and according to this metric glucose consumption appears even worse than fructose or HFCS. However, recent evidence suggests that post-prandial levels of TG (Figure B) are a more accurate way to assess atherosclerotic risk, as seen here, here, and here. One question I have is why did the AUC calculations in Figure A show a reduction in plasma TG level for the glucose group?
The figure below summarizes the differences in LDL-C, non-HDL-C, apoB, and apoB/apoA-I.
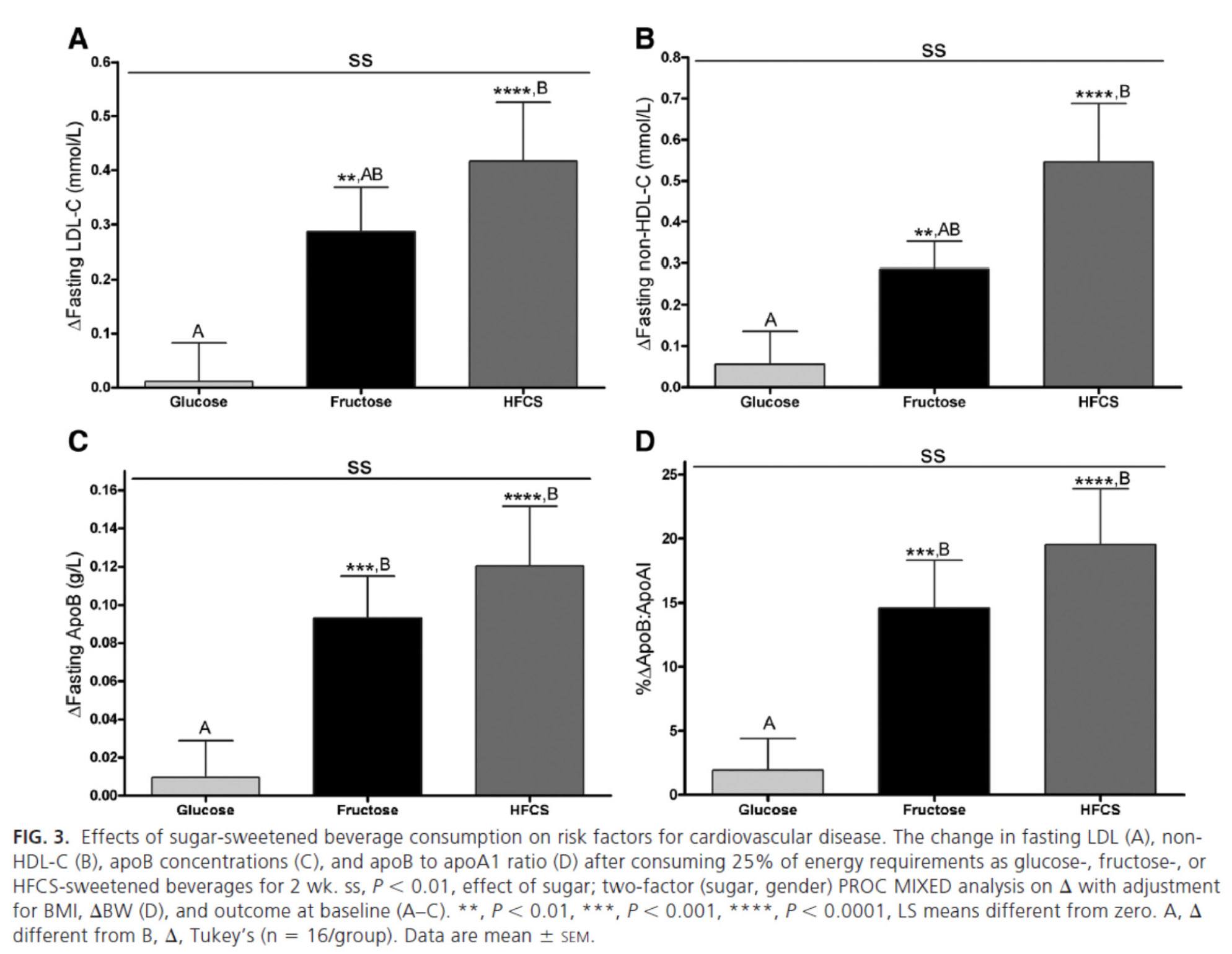
Again, the results were unmistakable with respect to the impact of fructose and HFCS on lipoproteins, and by extension, the relative lack of harm brought on by glucose in isolation. [Of course, removal of glucose and fructose/HFCS would have been a very interesting control group.]
One of the simultaneous strengths and weaknesses of this study was the heterogeneity of its subjects, who ranged in BMI from 18 to 35, in age from18 to 40, and in gender. While this provided at least one interesting example of age-related differences in carbohydrate metabolism (older subjects had a greater increase in triglycerides in response to glucose than younger subjects), it may have actually diluted the results. There were also significant differences between genders in the glucose group.
What was most interesting about this study was the clear difference between the 3 groups that was not solely a function of fructose load. In other words, the best outcome from a disease risk standpoint was in the glucose group, while the worst outcome was not in the all-fructose group, but in the 50/50 (technically 55/45) mixed group. This is a very powerful indication that while glucose and fructose alone can be deleterious in excess, their combination seems synergistically bad.
The role of saturated fat in cardiovascular disease
In the next week or two I’ll be posting an hour-long comprehensive lecture I gave at UCSD a few weeks ago on this exact topic. Rather than repeat any of it here, I’ll highlight one study that I did not include in that lecture. The study, Effect of a high saturated fat and no-starch diet on serum lipid subfractions in patients with documented atherosclerotic cardiovascular disease, published in 2003, treated 23 obese patients (average BMI 39) with known cardiovascular disease (status post coronary artery bypass surgery and/or stent placement) with a high-fat ketogenic diet. Because the study was free-living and relied on self-reporting, not all subjects had documented levels of elevated serum B-OHB. However, the subjects were instructed to avoid starch and consume 50% of their caloric intake via saturated fat, primarily in the form of red meat and cheese. There were no restrictions on fruits and vegetables, which may have accounted for the observation that not all subjects were ketotic during the 6-week intervention. In total, only 5 of the 23 patients achieved documented ketosis.
All of the subjects were on statins and entered the study at a goal LDL-C level target of 100 mg/dL, which may have been the only way the authors could get the IRB to approve such a study.
The table below shows the changes in lipoprotein fractions following the intervention (there was no control group):
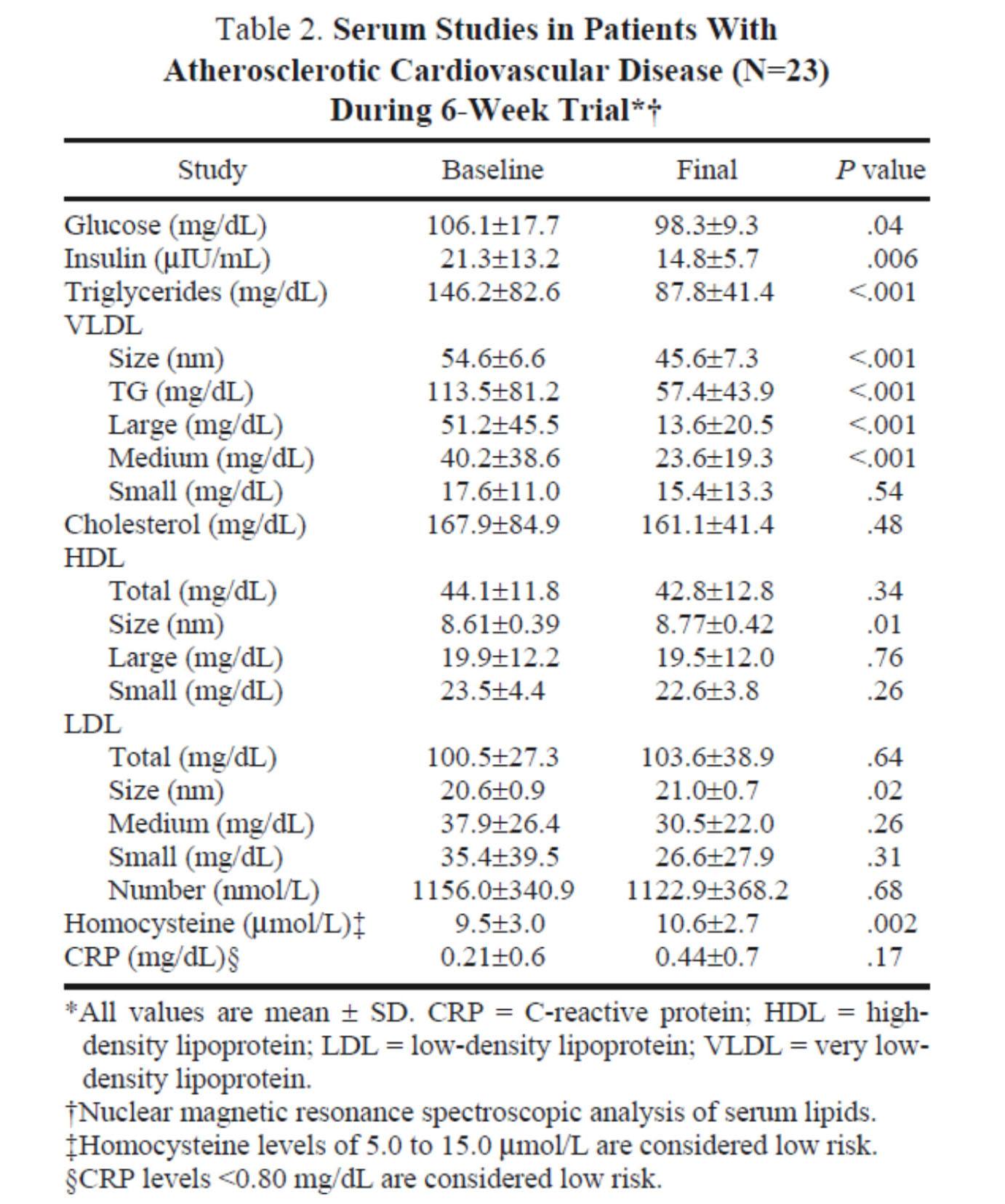
This study was conducted during the height of the “outcry” over the Atkins diet. While most doctors reluctantly agreed that Dr. Atkins’ diet could reduce body fat, most believed it was still very dangerous. In the words of Dean Ornish, “Sure you can lose weight on a low-carb diet, but you can also lose weight on heroin and no one would recommend that!”
Fair point. In fact, the authors of this study acknowledged that they “strongly expected” this dietary intervention to increase risk for cardiovascular disease, which is why they only included subjects on statins with low LDL-C. However, as you can see from the table above, the authors were startled by the results. The subjects experienced a significant reduction in plasma triglycerides and VLDL triglycerides, without an increase in LDL-C or LDL-P. In fact, LDL size and HDL size increased and VLDL size decreased – all signs of improved insulin resistance. Furthermore, fasting glucose and insulin levels also decreased significantly. The mean HOMA-IR was reduced from 5.6 to 3.6 (normal is 1.0) and TG/HDL-C from 3.3 to 2.0 (normal is considered below 3, but “ideal” is probably below 1.0) in just 6 weeks. Taken together, these changes, combined with the dramatic change in VLDL size, suggest insulin resistance was dramatically improved while consuming a diet of 50% saturated fat!
As all of these patients were taking statins, we’re really robbed of seeing the impact of this diet on LDL-P, which did not change. Also, CRP levels rose (though not clinically or statistically significantly).
Putting it all together
It is very difficult to make the case that when carbohydrates in general, and sugars in particular, are removed or greatly reduced in the diet, insulin resistance is not improved, even in the presence of high amounts of saturated fats. When insulin resistance improves (i.e., as we become more insulin sensitive), we are less likely to have the signs and symptoms of metabolic syndrome. As we meet fewer criteria of metabolic syndrome, our risk of not only heart disease, but also stroke, cancer, diabetes, and Alzheimer’s disease goes down.
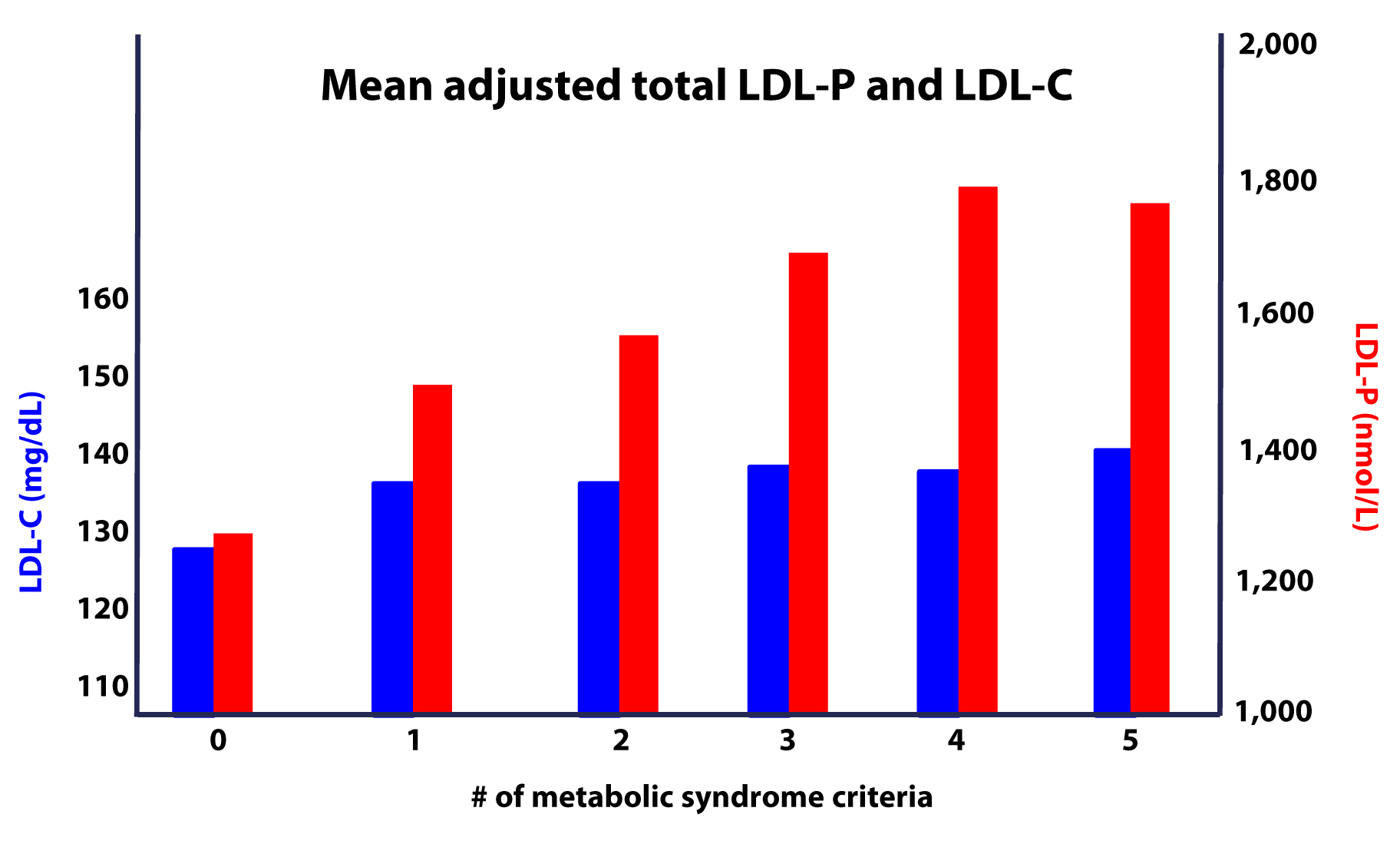
Furthermore, as this study on the Framingham cohort showed us, the more criteria you have along the spectrum of metabolic syndrome, the more difficult it becomes to predict your risk, due to a widening gap in discordant risk markers, as shown in this figure.
As I noted at the outset, the “dream” trial has not yet been done, though we (NuSI) plan to change that. Until then each of us has to make a decision several times every day about what we will and won’t put in our mouths. Much of this blog is dedicated to underscoring the impact of carbohydrate reduction on insulin resistance and metabolic syndrome.
The results of the trials to date, combined with a nuanced understanding of the lipoprotein physiology and their role on the atherosclerotic disease process, bring us to the following conclusions:
- The consumption of sugar (sucrose, high fructose corn syrup) increases plasma levels of triglycerides, VLDL and apoB, and reduces plasma levels of HDL-C and apoA-I.
- The removal of sugar reverses each of these.
- The consumption of fructose alone, though likely in dose-dependent fashion, has a similar, though perhaps less harmful, impact as that of fructose and glucose combined (i.e., sugar).
- The addition of fat, in the absence of sugar and starch, does not raise serum triglycerides or other biomarkers of cardiovascular disease.
- The higher the level of serum triglycerides, the greater the likelihood of discordance between LDL-C and LDL-P (and apoB).
- The greater the number (from 0 to 5) of inclusion criteria for metabolic syndrome, the greater the likelihood of discordance between LDL-C and LDL-P (and apoB).
I would like to address one additional topic in this series before wrapping it up – the role of pharmacologic intervention in the treatment and prevention of atherosclerotic disease, so please hold off on questions pertaining to this topic for now.



In your summary, you state:
“The addition of fat, in the absence of sugar and starch, does not raise serum triglycerides or other biomarkers of cardiovascular disease.”
Listening to an interview with Jimmy Moore and Dr. Dayspring (see https://www.askthelowcarbexperts.com/2012/10/29-dr-thomas-dayspring-cholesterol-testing-what-matters-most/ ) there is some discussion about individuals who see their LDL shoot up when going on a low-carb diet (and also the possibility of elevated LDL due to weight loss).
It seems like these two ideas are in conflict — it seems like there may be some people for whom a ketogenic or low carb diet could cause LDL-P to skyrocket (I suspect I may be one of these people, but obviously haven’t permuted through the possible variables).
If this is true, it seems like the benefits of a low-carb diet on heart disease markers may need an asterisk for some portion of the population…very confused here! Any light you could shed on this?
That’s correct. This will be discussed in part X of the cholesterol series if I can get to it.
Peter,
Do you have a best guess about when you will be likely to get to Part X ?
Your explanations are so clear! It looks to me like there are several (many? hundreds? thousands?) of us out here who are very eager for your next cholesterol tutorial.
Thank you again.
My goal is to get to Part X before I stop blogging (the date for which I have not yet decided, of course).
https://www.nytimes.com/2013/07/10/health/rare-mutation-prompts-race-for-cholesterol-drug.html?nl=todaysheadlines&emc=edit_th_20130710&_r=0&_r=0
Not a cut and dried issue IMO because the drug will lower not only sdLDL-C, but large. Also, typical it doesn’t address the possible side effects either. Thoughts?
I comment (briefly) on PCSK9 in both the cholesterol series (I don’t recall which part) and in my talk on YouTube (https://www.youtube.com/watch?v=dAWdHYSrh7M).
I sent this information to my cardiologist
01-13-2012 12-18-12 02-23-13 07-02-13
LDL-P 1137 1099 1103 1209
Small LDL P 761 731 711 677
He replies “Just keep in mind that no one knows if these are markers of risk or mediators of risk. If they are just markers, then changing them won’t matter. It takes clinical trials to learn whether changing the readings meaningfully changes your health. The healthcare highway is littered with the burned out wrecks of therapies that treated markers, not mediators.”
What do you do to stay healthy when you are trying to do what is best?
True, but in this case the data are pretty good that LDL-P or apoB track closely, at least in SAD-consuming populations.
Hi Dr. Attia, I don’t remember which part of the Cholesterol Series discussed calcium, but I remember it was not advisable to take calcium supplements because calcium can be involved in plaque formation. On a low carb or ketotic nutrition plan, should a female (because of the concern for the prevention of bone loss) who is lactose intolerant supplement calcium at all, or to some specific dose, since no dairy or cheese is in the diet? Thank you very much, maryann
Dr. Attia, I appreciate the work you are doing. I have a few risk factors that probably place me with metabolic syndrome. I’m trying to do the research and determine what diet I should adopt, as a lifestyle – not a quick fix. This has proven to be a much more difficult task than I imagined. I’ve tried to limit my reading to sites that seem to operate with academic integrity. I’ve gleaned a lot of information from your site but was surprised and frustrated when I read in point #7 above where you wrote:
“Eating cholesterol has very little impact on the cholesterol levels in your body. This is a fact, not my opinion. Anyone who tells you different is, at best, ignorant of this topic. At worst, they are a deliberate charlatan. Years ago the Canadian Guidelines removed the limitation of dietary cholesterol. The rest of the world, especially the United States, needs to catch up. To see an important reference on this topic (the link you provided takes you to a site where only 2 pages of the research document are available)
Here is where I was surprised – You took such a dogmatic approach, stating that anyone who thinks differently is either ignorant or a charlatan. Really? I don’t necessarily think differently because I don’t know what to think yet. I’m looking for the truth – which has become very hard to find. I read the 2 pages that were available on the link. The article that you are pointing to as proof states, “the relation between dietary cholesterol and the risk of CHD is not clearly understood”. That doesn’t sound like very compelling proof. Am I missing something? The last paragraph in the available 2 pages states that both LDL and HDL appear to be influenced by dietary cholesterol. There is more to the paper that I didn’t have access to. But, the abstract clearly states that the relationship between dietary cholesterol and CHD is not clearly understood. So, if the relationship isn’t clearly understood, how could you label people that disagree with your opinion, which you are calling a fact, as ignorant or a charlatan?
Again, I don’t have any agenda other than trying to find the truth to help me determine what diet changes I need to make. A big question for me while gathering information is, can I trust the author? The way you stated your cased on this issue called that into question for me. It’s surprising, because up until I read this it appeared that writing with integrity was very important to you. I’m sure I must have misunderstood something because you seem to be a person of high character, ethics, and integrity. Please let me know what I’ve misunderstood.
Thank you,
Craig
Craig, many things are still unknown. This, however, is not one of them. So while I’m not dogmatic with respect to many things in nutrition, I am with respect to this. And the laws of gravity. BTW – the statement that dietary dietary cholesterol and the risk of CHD is not the same as the (much simpler) statement I made — dietary cholesterol levels have little impact on (serum) cholesterol levels in the body. Does this nuance make sense? Consider the following, also, look at the largest association study of dietary cholesterol and serum cholesterol (Framingham Heart Study). Here is what they found, though this was unpublished in 1968 at the time of the first publication. They compared cholesterol intake of those with serum levels above 300 mg/dL to those below 170 mg/dL. No difference. They concluded, “There is considerable range of serum cholesterol within the Framingham Study Group. Something explains this inter-individual variation, but it is not diet (as measured here).” So while SFA consumption impacts HDL-C and LDL-C, it’s not the dietary cholesterol per se. Another way to think about this is by considering the chemistry of cholesterol (i.e., esterified vs. free) and the path for CE to enter the body via the NPC1L1 transporter on enterocytes. Can’t happen unless cholesterol is UNesterified. Back to laws like gravity.
Peter,
I’m glad to say that today I finally went and got my blood work(NMR Lipo Test) done after following a pretty restrictive Ketogeic diet for about 5 1/2 months now. My only regret is that I didn’t know about the in’s and out’s of this diet and your teachings until about a quarter of the way through. I’ve lost 38 pounds to date and feeling great. I’ve post on your blog before and there is a lot of information to digest on here, so even using your search tool its hard to find specific things sometimes. Like yourself, I think I’m very carb sensitive and have to keep em pretty low to stay in Ketogenic state. I’ve looked on the blog for a simple breakdown of what you think the ideal numbers should be for the NMR Lipo Test (The particle test). Is there a quick guide that you know of that explains the numbers line by line or an NMR for dummies. Are your numbers of your most recent test listed anywhere on the blog? I get my results back in a couple days and I want to know what I’m looking at. What should my LDL-P be (in a perfect world) considering i’ve been doing this for 5 to 6 months now.
Side Note:
You weren’t lying when you said most doctors wouldn’t be familiar with this test. This MD had never even heard of LDL-P, much less NMR LipoProtein test. I told him that if he knew what I knew, he would never prescribe another standard Lipid test again. This guy was about 50 I think. I told him not to feel bad about it because he was probably never taught these things in med school and its probably not required reading once you got your credentials behind your name. He actually admitted that he wasn’t up to snuff on all the things he should know on cholesterol. I was highly surprised he said that, but I wasn’t a prick about it. He was curious how I knew so much about the subject and I told him a MD by the name of Peter Attia told me on youtube and his blog. So it’s funny, I had to go to a doctor to get a prescription for a test that the doctor had never heard of. I had to pay him for his lack of knowledge on the subject because I couldn’t go straight to the source and get what I needed. He should have waived the fee for the office visit in my personal opinion, that’s definitely what i would have done if it were my practice . Then, I go to the lab and they’ve never heard of the test and they were curious how I knew so much. Crazy right? So, they drew the blood and sent it to Labcorp. Quest didn’t offer the test. It was about 166 bucks in case your readers as interested. Its amazing how curious people get when you tell them you lost 38 pounds in 5 months with no exercise. Women seem to get way more curious than guys for some reason. I’m always happy to tell them that all you have to do is break your addiction to sugar, which is harder than to stop drinking alcohol and regulate a low insulin level all day every day.
Randy, I have not done a how to read your NMR test per se. Most of the info is embedded within the cholesterol series, though. Sorry it’s such a hassle to get the test done, but glad you did.
In response to Randy’s difficulties in getting his NMR profile done, there is a way, in the USA at least of ordering this yourself without going through your doctor. There is a company called health testing centres healthtestingcentres.com who will arrange any blood test you might want e.g. nMr profile currently costs $129 I think. You pay for the test online and then arrange to have blood drawn at a convenient location, results get emailed to you in a few days. NMR is not available in New Zealand where I live so I organised this when I was in San Francisco earlier this year at a conference. It worked flawlessly. The only problem is that you then have to interpret the data. Even though I am a physician (not a lipidologist though) it took me several goes to understand the data. They give quite a good risk profile assessment as part of the report which helps. I would think that, if you are not fully conversant with the ins and outs of NMR, doing your apoA and apoB would be be easier to understand, and maybe give a simpler assessment of the effect of any intervention you are undertaking, and give almost as much information as the NMRprofile at a lower cost.
I am not sure.
I guess I wondered, in the absence of expert interpretation of an NMR, it would be easier for an individual to make sense of apoA and apoB. The test is also going to be cheaper and does not need fasting to do. One of the problems I could foresee in ordering a test without your doctor’s OK or against his advice, is that said doctor may feel quite threatened by this , particularly if you appear to be more knowledgeable or adopt an assertive position, and become ” non cooperative” with one’s future health care. Sadly, not all doctors have as much openness and humility as you Peter!
Very similar information. The “expertise” is necessary to put numbers in context, based on other risk factors.
Thanks for the input guys.
Peter,
Got my results back today and they were pretty discouraging. Really couldn’t believe them. I’ve lost weight down to my goal of 172, I feel great, I sleep great, energy level is up all day, and I’m making plenty of ketones. Maybe you can give me some advice. I’m eating pretty much all or alot of the same things as yourself. Here are my NMR RESULTS:
LDL -P 1579 nmol/L
LDL -C 150 mg/dl
HDL -C 55 mg/dl
Triglycerides 100 mg/dl
Total Cholesterol 225 mg/dl
LDL and HDL PARTICLES
HDL -P (Total) 27.5 umol/L
Small LDL -P 586 nmol/L
LDL Size 21.1 nm
My LP – IR test assessment for insulin resistance was 24
Any suggestions would be great.
Thanks in advance.
I also had an NMR lipoprofile done lately. Had to escalate from GP to internist to get it, and the internist also supplied no interpretive guidance (but of course suggested going on statins, even though the two numbers that really matter, my small LDL and trig, are extremely low, and there are zero other indications; so much for his credibility). My total LDL-P, like yours, is highish (near the 1600 nmol/l level).
I had the numbers looked at by an independent cardiac MD, who just happens to be working on (but hasn’t completed) a “how to read your numbers” article – which isn’t trivially simple, due to the variety of labs available.
His assessment in my case was mild hypothyroid, possibly to be resolved merely by going back on the iodine (kelp) I had discontinued a month before the lab. I’ll be on it for the follow-up, and I will also be insistent on getting the complete thyroid panel I asked for last time (FT3, FT4, RT3) and didn’t get (TSH and TT4 are about as useful as TC and LDL-C). It is likely to be the case that once major other side effects of a full-time glycemic diet are cleared away, underlying thyroid problems will often be exposed, if they are correctly measured, assessed and treated (which, as with CVD, they usually are not). I also have family history of thyroid issues.
The above, of course, might have no bearing on your case – where the first question that came to mind actually was: are you still losing weight? My understanding is that this does skew lipid reading whilst in progress.
Boundless,
Thanks for you comments first off. My weight loss has stalled at 172 morning weight. I think because that’s actually how much I should weight normally. My belly button circumference is 32 inches now from 43 inches. It was my goal weight from the beginning and I just got there about 2 weeks ago. It’s very interesting that you bring up potential thyroid imbalance. Unlike you, I don’t really know of my family having thyroid issues, but I wouldn’t rule it out because my Mom and Dad really never cared about knowing there potential health problems. I will say that I have had an uncomfortable feeling in my throat for the last 3 months. It seems to come and go and feels kind of like a tugging or a constant pulling sensation. Doesn’t hurt though.
A little background on my diet and exercise might shed some light. I have done essentially no exercise to lose the weight and like Peter I inhale saturated fat. A lot of the fat I’ve been taking in has been through the yogurt and heavy whip cream in my scrambled eggs and coffee. I’m beginning to think this is my problem. I should have done moderate exercise along the way, but didn’t. I just love telling people I lost all the weight and didn’t do any exercise. The look on their faces are priceless. I will be exercising for the next 3 months and building muscle. I will be eating more of the same things. I think I will go and get a thyroid work up. Its been in the back of my mind, but haven’t done it because I haven’t seen any of the commonly know symptoms. I have done some reading on the subject though and have found that most people that get diagnosed never even knew they had it.
I’ve been looking for part x on the role of pharmacologic intervention in the treatment and prevention of atherosclerotic disease and can’t find it. Am I missing it?
Still in my head, unfortunately.
Is there any way I can convince you to write it? I’ve got a great almond ball recipe I’ll swap for it.
I will at some point. My day job is pretty demanding, though.
Btw, thank you for an amazing series and blog! 🙂
This video may speak to my issue as it relates to active weight loss. The next 3 months shall be a good test. Steve Phinney
https://www.youtube.com/watch?v=MNfjkTyBUdQ
I lost 26 pounds 154 to 128 lbs and my cholesterol went from 190 to 274 and my ldl went up as well. It occurred during menopause. I am not a fan of statins. Both my father and grandmother developed diabetes about a year after taking statins. Can you give me any advise?
Christina,
Happened to me, too. I’ve lost 30 pounds, my BP is fine now, and I stopped taking a statin and niacin. My total cholesterol and LDL-C are both high after my LC diet. But my TG/HDL-C ratio is now under 2, which makes me think I’m probably OK.
This seems to be common (or not uncommon) occurrence after LCHF diets. They discuss it at length in “Cholesterol Clarity,” by Jimmy Moore and Eric Westman. Dr. Westman also said that after a patient has lost a lot of weight, he waits until the patient’s weight has been stable for a while before checking lipids and lipoproteins.
The main thing I think most of the experts would say is for us to check our ApoB or LDL-P levels. If they are OK, then the old measurements of TC and LDL-C don’t matter. I plan to have mine checked before long.
I cannot give advice,but i will repeat what Peter has said. Cholesterol levels have little to do with what you feed your face and is probably an under lying issue causing higher than normal levels. By reading this blog, the problem seems pretty common. In my case, only a little bit of time will tell. i may have to re evaluate after that and until then i will keep doing more of the same. Correct me if im wrong Peter.
Hi Peter,
Brilliant resource on cholesterol, I think I stuck with it and follow ‘most’ of it. It’s quite a rabbit hole and I’ve read so much that I can’t see the wood for the trees. I have 2 very quick questions though. I have just had my blood tested (national health service here in the UK) lipids, liver, thyroid, electrolytes, b21 & folate, GFR. I understand that at best these are nothing more than an indication and their usefulness is limited. so 1) should I ignore them or only focus on certain ratio’s / numbers 2) if I should only focus on certain things, can you point me in a direction of a useful resource / website where I can make some sense or meaning from my results?
Dear Peter,
Could you speak to the reported hyperlipidemia of children on KD for epilepsy? It has become common wisdom that their KD-induced hyperlipidemia can be corrected by lowering saturated fat and cholesterol in the diet. This seems to go against what you and many others have found to be true for adults on the KD. Here some examples of this common wisdom:
https://jama.jamanetwork.com/article.aspx?articleid=197131
https://can.sagepub.com/content/1/6/338
https://www.sciencedirect.com/science/article/pii/S092012111100204X
Yes, there may be other things going on kids on KD, and to be honest, I’m not an expert on the formulations of the diets in kids, though I can only imagine how much more difficult it is. I had read the JAMA paper before and reached out to the lead author to learn more, but he did not respond, unfortunately. I would be curious what Elizabeth Thiel’s experiences have been. She’s at Boston Children’s Hospital and probably has one of the largest practices in the world using KD for epilepsy. I’d also like to know the apoCII status of the kids the respond well to switching out the SFA for MUFA and PUFA.
Peter,
Reading this series was like reading a serial novel — I couldn’t wait to get to the next chapter.
At one point, I think you said that those who were favorably discordant (high LDL-C, low LDL-P) had even lower risk that those who were low and concordant. Any theories why that would be so?
I understand that insulin resistance is implicated in those with unfavorable discordance. Is there anything common about those who are favorably discordant? (Other than the fact that their LDL particles must be relatively large.) Just curious.
Thanks for all you do.
Just based on the longitudinal survival data I presented. Not sure why, though. The differences is minor.
Dr Attia really takes on the lipid world. Well worth your time to look at his site if your health issues relate to heart, inflammation, sugar, diabetes or weight. Bravo for taking on the myths and fallacies with facts and concrete recommendations.
I will not send my numbers, but having read all nine parts – more than once – along with The Truth About Statins and much more, I still need to know…straight up…what should I do?
I know you can’t and won’t give advice, so this is a hypothetical question. What do I do now? I’m 58, can’t handle any more mental fog than I already have! so really, really do not want to take statins. My doctor – who actually is very careful about reading the primary literature and who is well-versed in these questions – is still recommending statins.
I don’t eat animal protein except for fish and an occasional egg (for reasons other than health; it is personal preference); I eat only slow carbs (low glycemic index), non-starchy vegetables, fruit. I exercise an hour a day and 3-4 hours on Saturday and Sunday. All since November 2012. Take 81 mg aspirin per day.
The LDL-P is still in the very high range though its concordant with the LDL-C (all measured via NMR). HDL-P is low, triglycerides are low.
Weight is appropriate, blood pressure is fine, blood sugar is fine.
Family history unknown except for immediate family (father, two uncles, mother – no heart disease).
What else can I do besides taking statins?
Oh. forgot to say – I’m female.