Dr. Patricia Corby is Associate Professor of Oral Medicine and Associate Dean of Translational Research at Penn Dental Medicine. Her work focuses on the value of integrating dental services into other healthcare and public health settings. In this episode, Pat provides an overview of dental anatomy, the importance of oral hygiene to overall health, and the association of poor oral health and systemic diseases like cancer and diabetes. She addresses tooth decay, oral hygiene in children, the utility of dental products, and ideal oral care regimens for different populations. She also discusses issues specific to immunocompromised patients and those with chronic illnesses as well as her own research with cancer patients undergoing radiation treatment.
Subscribe on: APPLE PODCASTS | RSS | GOOGLE | OVERCAST | STITCHER
We discuss:
- Anatomy of teeth and the purpose of the dental pulp—a highly vascularized and innervated region of the tooth [3:00];
- Types of teeth and the different purpose they serve [14:15];
- Anatomy of the oral cavity, bacteria in the mouth, and what a healthy mouth looks like [18:10];
- Pat’s study demonstrating the importance of flossing [23:00];
- Detrimental effects of sugar and the importance of fluoride and oral hygiene [31:45];
- Oral health challenges for cancer patients and immunocompromised people [39:45];
- Pat’s current research on cancer patients undergoing radiation treatment and the oral health risks associated with human papilloma virus (HPV) [50:00];
- Periodontal disease: caries and root canals [57:30];
- The relationship between poor oral health and systemic health diseases [1:11:00];
- Potential connection between oral hygiene and COVID-19 [1:17:45];
- Dry mouth leading to oral infections and ways to prevent it [1:22:30];
- What determines the appearance of teeth, methods of teeth whitening, and whether you should remove mercury fillings [1:27:30];
- Importance of fluoride for preventing tooth decay, and dental care for children [1:32:45];
- Useful dental products: floss, electrics toothbrushes, and more [1:39:15];
- Ideal oral care regimens [1:47:30]; and
- More.
Get Peter’s expertise in your inbox 100% free.
Sign up to receive An Introductory Guide to Longevity by Peter Attia, weekly longevity-focused articles, and new podcast announcements.
Anatomy of teeth and the purpose of the dental pulp—a highly vascularized and innervated region of the tooth [3:00]
- Pat likes to talk about oral health with MDs because the connection to health is important
- Peter has long wanted to discuss oral health, which is “a very underappreciated part of health” that is more than just cavities and cosmetic concerns
Pat’s background
- Pat grew up in Brazil
- Wanted a career involving systemic health
- specialty is in periodontics and implant dentistry
- Always wanted to do research
- Stayed in US because so many professional opportunities
- Peter mentions the anniversary of the death of Ayrton Senna
- Pat was watching the race on TV
- Peter says he’s never met a Brazilian person who was over 5 on that day who doesn’t remember it
- Peter says Senna is his personal hero, and he is wearing a Senna bracelet for the occasion
- Peter did not go to the dentist for about 10 years during medical school and residency, but now he takes dental care very seriously
Anatomy of teeth [6:15]
- The periodontium is very complex system
- Peter points out that there’s a vascular supply quite high in the tooth even though many people might assume that the white crown is just bone
- Tooth enamel, made of minerals, is the hardest surface in the human body
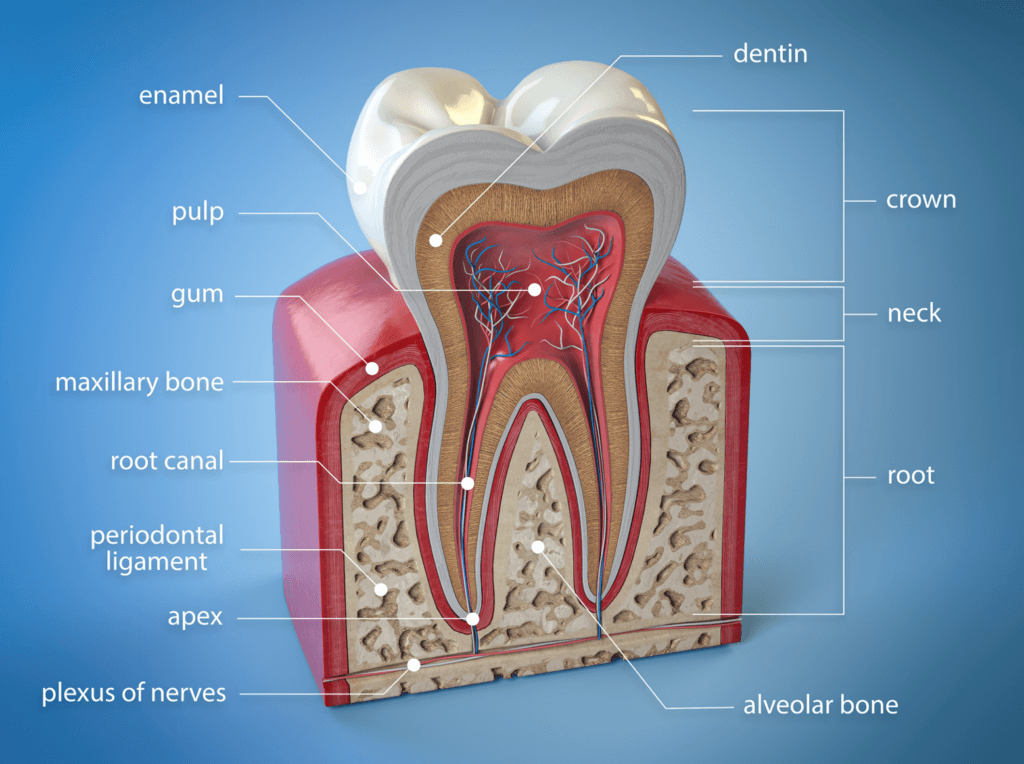
Figure 1. Individual tooth anatomy. Image courtesy of Pat Corby.
- On the top is enamel and cementum (around the root), then dentin, then pulp
- The enamel protects the layers underneath (hardest surface of the human body)
- The second layer provides cushioning and is hyper sensitive
- the heart of the tooth is the pulp, which has a lot of nerves – explains why tooth pain can be so bad
- ligaments around the roots provide cushioning against impact
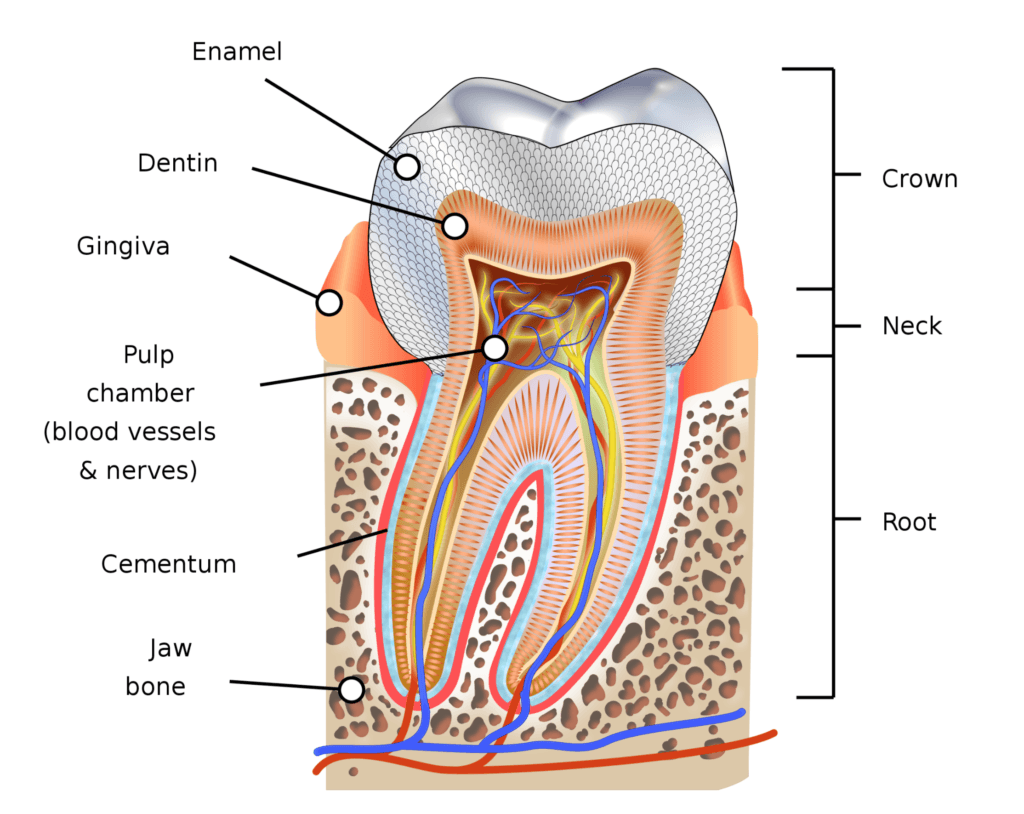
Figure 2. Anatomy of a tooth showing cementum. Image credit: Wikipedia
The role of the nervous connection and vascular supply to the tooth [10:40]
- Tooth decay
- Tooth decay first affects the pulp
- If you excise the pulp, you can preserve the root
“The way you want to think in dentistry is that … you want to preserve function.” —Pat Corby
- Try not to extract teeth because the space they hold is important
- If necessary, do a root canal or put in an artificial crown
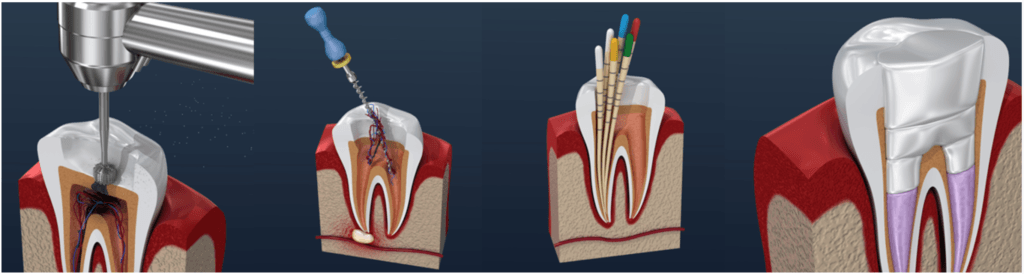
Figure 3. Progression of a root canal treatment. Images courtesy of Pat Corby.
- Put implants in if you have to extract an entire tooth; not as good as a real tooth but can still hold the space and provide some function
- Can still get inflammatory periodontal disease with an implant
- Peter wonders why teeth are so highly innervated
- Implants without nerves can still break down food
- Our fingers are highly innervated because we need fine motor control, but why so much beneath the hard enamel?
- Pat says it preserves blood flow and connection with the immune response to fight infection
Function and innervation of the pulp (this section contains additional information provided by Pat after the podcast was recorded)
- The main four functions of the pulp:
- formation of dentin – one the most important roles, carried out by odontoblasts
- support of dentin through nutritional support (albumin, transferrin, tenascin, and other proteoglycans)
- innervation of the tooth
- immune system protection of tooth: occurs through the development of new dentin, which can provide a barrier between irritants and slow the rate of carious decay
- Two main types of nerves are found in the pulp:
- Sympathetic autonomic fibers to the smooth muscle cells of pulp arterioles control contractile forces that regulate blood flow
- Afferent fibers are involved in temperature sensing and mechanical nociception
- Peter reflects that dental pain seems to serve as such an early warning indicator as a breach of a barrier
- He says, “Having been through so many miserable dental experiences, I’ve often cursed our evolutionary gods for giving us so much innervation in that tooth”
{end of show notes preview}
Would you like access to extensive show notes and references for this podcast (and more)?
Check out this post to see an example of what the substantial show notes look like. Become a member today to get access.

Patricia Corby, D.D.S., M.S.
Dr. Patricia Corby is an Associate Professor of Oral Medicine and the Associate Dean of Translational Research at the University of Pennsylvania Dental Medicine. She is also the Director of the Penn Dental Medicine Center for Clinical and Translational Research. She is an experienced researcher with over 20 years of experience designing and running high-impact clinical research projects and has served as Principal Investigator, Co-Investigator, or Consultant on a number of projects funded by the National Institutes of Health (NIH), foundations, and industry. Dr. Corby’s work focuses on the value of integrating medical and dental services in different healthcare and public health settings to prevent systemic complications of populations with unmet oral health needs and associated chronic diseases. After receiving her DDS and completing her residency in Periodontics and Implants in her native Brazil, she obtained her MS in Biomedical Informatics from the University of Pittsburgh School of Medicine completed a postdoctoral training in Molecular Biology and Microbial Genetics at Harvard University and the Forsyth Institute.
Professional website: https://www.dental.upenn.edu/faculty/patricia-corby/